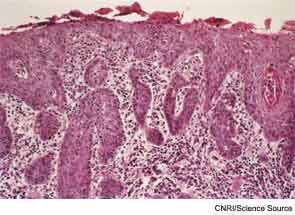
A natural outgrowth of the decades-long movement toward evidence-based medicine is an increased focus on the assessment of physician performance in applying the best evidence to diagnose and treat a patient with a specific condition. To this end, quality of care measures are being developed for specific conditions within most specialties to guide physicians and assess their performance in implementing the best care based on the most up-to-date evidence.
Two current initiatives offer otolaryngologists a way to join the growing ranks of physicians in other specialties who are using quality measures to assess their performance. In 2008, the American Head and Neck Society (AHNS) launched quality of care measures for oral cavity cancer. In February 2013, the American Board of Otolaryngology (ABOto) rolled out a Performance Improvement Module (PIM) on oral cavity cancer that uses the AHNS quality measures. The PIM is one component of Part IV of the Maintenance of Certificattion (MOC) program offered by ABOto.
“The aim of both initiatives is to provide feedback to otolaryngologists on their strengths as well as on areas that need improvement in diagnosing and treating patients with oral cavity cancers,” said Robert H. Miller, MD, executive director of ABOto and physician editor of ENTtoday, who hopes physicians will participate in the initiatives in the spirit in which they were developed, not as a stick but as a carrot to encourage participation to improve performance and, ultimately, patient outcomes.
Oral Cavity Cancer Quality Care Measures
The oral cavity cancer quality care measures developed by the AHNS include quality measures in three areas: pre-treatment, treatment and post-treatment. Key pre-treatment measures are the need for pathologic confirmation of disease, appropriate TNM staging documentation and tobacco cessation counseling. Key treatment measures are radiation oncology referral for all patients with advanced T stage or metastatic lymph node disease, and referral to a medical oncologist and a radiation oncologist for all patients with positive pathologic margins or metastatic lymph nodes showing extracapsular extension. Key post-treatment measures are the need for follow-up visits for symptom management and for recurrence and second primary tumor
surveillance, and assessment of serum thyroid stimulating hormone level within 12 months for patients treated with radiation therapy to the neck to detect hypothyroidism.
According to Amy Chen, professor of head and neck surgery at Atlanta’s Emory University, who chaired the AHNS multidisciplinary committee that developed the quality measures, oral cavity cancer was the first disease to be chosen to develop these measures because the committee wanted to pick a condition that is commonly seen by otolaryngologists and is a surgical condition handled by members of the AHNS on a daily basis.
To develop the measures, Dr. Chen and her colleagues followed a process similar to those used to develop quality measures by larger organizations such as the American Cancer Society and National Quality Forum, but on a much smaller scale. They conducted a literature review and ranked the evidence, culling the highest evidence available, to come up with yes and no questions that reflected good quality of care.
She emphasized, however, that these quality measures are not the same as clinical guidelines. “I view clinical guidelines as more of a cookbook: They tell you what to do, but they do not measure the process,” she said. “Quality measures measure the output of what you are doing, so they can be seen as on the backside of clinical guidelines, more like a report card.”
Randal S. Weber, MD, professor and chairman of the department of head and neck surgery at the University of Texas MD Anderson Cancer Center in Houston, who was also involved in initiating and developing the AHNS measures, described the quality measures as an extension of practice guidelines. “We have practice guidelines that are the best evidence available for treating oral cavity cancers, and the quality measures are really a measure of how well you are following those guidelines,” he said.
Physicians who want to measure how they are doing in managing patients with oral cavity cancers can complete a simple form that lists the key quality measures identified (available at ahns.info). AHNS members can use this form to obtain patient information, which is then entered into a database. The physicians are given feedback on how well they are adhering to each quality measure. Although Dr. Chen said that some physicians may find inputting the data burdensome, she emphasized that efforts are underway to make the system as user friendly as possible.
William Lydiatt, MD, professor and division chief of head and neck surgical oncology at the University of Nebraska Medical School in Omaha, whose division has adopted the AHNS quality measures, said that the measures are practical and can be implemented. “We started with a review of what we had been accomplishing and found that there were areas where we could improve,” he said, adding that one particular area that his division is working on improving is smoking cessation. For Dr. Lydiatt, one key issue is that the measures require significant resources, such as speech and swallowing therapy, and these can be time and personnel intensive.
PIM
More recently, the AHNS quality measures have been used to develop the first PIM in otolaryngology that fulfills one of the ABOto’s MOC requirements. According to Dr. Weber, who chairs the ABOto MOC committee, the AHNS quality measures are appropriate for the PIM because they indicate the best quality of care identified for oral cavity cancers. Physicians can use the measures to analyze their practice, find areas needing improvement, implement changes to improve those areas and retest their practice based on the changes made. This is a classic performance improvement methodology, he said, and one that fulfills Part IV of the MOC requirements.
The aim of the PIM is to provide feedback to physicians on their strengths as well as on areas that need improvement in a given clinical area, said Dr. Miller. “The PIMs are not meant to be punitive,” he said.
The PIM consists of three stages, he said: A, B and C. In stage A, physicians enter patient information, based on the AHNS quality measures, into a registry. The information is de-identified, said Dr. Miller, so that the patient is anonymous and the focus is only on the quality measures. Currently, physicians are asked to submit information on 10 patients with oral cavity cancer.
Once stage A is completed, physicians receive feedback on how they are doing based on the quality measures. This is stage B, and each physician’s performance is shown as it compares with other head and neck surgeons and all physicians who complete the PIM (including physicians other than head and neck surgeons), as well as the AHNS quality measures.
In the final stage (C), physicians are asked to enter a new series of five patients that indicate the changes made based on the feedback in stage B. In an ideal world, the changes would be tracked to see if physicians improve after going through this quality improvement process, said Dr. Miller, adding that the current focus is to encourage physicians to participate in the hope that they will meet the quality measures and show improvement.
As of the time this article was written, he said, about a dozen people have accessed the ABOto website to participate. Eventually, the ABOto plans to develop two or three more PIMs in each practice focus area, including otology, laryngology, rhinology and pediatric laryngology. Among the PIM topics currently in production are rhinosinusitis and allergy immunotherapy. The board has also identified other quality measures needed, including parotidectomy, thyroidectomy, dysphagia, subglottic stenosis, tympanoplasty, pediatric hearing loss assessment, conductive hearing loss, aging face, nasal deformity, facial trauma, chronic sinusitis, adult sleep disorder and pediatric sleep disorder.
For more information on MOC and how to participate in the PIM on oral cavity cancers, contact Lauren Durst, the ABOto MOC coordinator, at ld@aboto.org, or visit aboto.org.
Leave a Reply