
The American Academy of Sleep Medicine (AASM) recently published new practice parameters on the treatment of sleep-related movement disorders, entitled “The Treatment of Restless Legs Syndrome and Periodic Limb Movement Disorder in Adults—An Update for 2012: Practice Parameters with an Evidence-Based Systematic Review and Meta-Analyses” (Sleep. 2012;359:1039-1062). The new parameters, an update of a 2004 guideline (Sleep. 2004;27:557-559), provide new recommendations for medical treatment based on the most current evidence.
According to Lee Shangold, MD, assistant clinical instructor of otolaryngology-head and neck surgery at Stony Brook University School of Medicine in Long Island, N.Y., these new practice paramenters provide, for the most part, an easy way to determine the standard of care for treatment of sleep-related movement disorders, primarily for restless legs syndrome (RLS).
For Dr. Shangold, one of a subset of otolaryngologists who are also certified in sleep medicine, these practice parameters may be particularly applicable. However, he also emphasized that all otolaryngologists must be aware of all conditions, including sleep-related movement disorders, that may affect sleep, to ensure that patients with disturbed sleep affecting daytime functioning are correctly diagnosed and treated.
Pell Ann Wardrop, MD, an otolaryngologist and medical director at the St. Joseph Sleep Wellness Center in Lexington, Ky., and chair of the American Academy of Otolaryngology-Head and Neck Surgery (AAO-HNS) Sleep Disorders Committee, agrees. “Otolaryngologists need to be aware of leg movement disorders, because a large number of patients with sleep apnea have an additional sleep disorder,” she said. “We need to be aware of all of the sleep disorders so that we don’t miss those patients with a sleep disorder other than, or in addition to, sleep-disordered breathing.”
Medication Recommendations
The primary focus of the 2012 updated practice parameters is the medical treatment of idiopathic RLS. Although the guideline also mentions periodic limb movement disorder (PLMD) in the title, the lack of evidence on this condition did not permit providing recommendations on its treatment.
According to R. Nisha Aurora, MD, a sleep specialist and assistant professor in the department of internal medicine at Johns Hopkins
University School of Medicine in Baltimore and lead author of the study, the updated practice parameters were less complicated to develop than many similar parameters in sleep medicine due to the strength and amount of evidence available, particularly the data related to the dopaminergic agents used to treat RLS. “The number and quality of studies looking at therapies for RLS is better than what we see for other sleep disorders,” she said. “Often, studies in the sleep medicine literature are small or of limited quality because sleep medicine is still a young and evolving field.”
Seth Schwartz, MD, the current chair of the AAO-HNS Guideline Development Task Force, thinks the practice parameter provides a nice review of the evidence on using a methodology that is presently considered state of the art. “The recommendations are evidence-based and pretty clear cut,” he said.
The study used principles of evidence-based medicine to develop three main levels of recommendations based on the quality of the evidence. Recommendations based on the highest quality of evidence are labeled “standard,” those based on clear evidence but not the highest quality are labeled “guideline” and recommendations based on data that is not of very high quality but is thought to be reasonable are labeled “optional.” To further clarify the strength of the recommendation, the AASM committee provided a data-based benefit/harm/burden assessment of each agent indicating the committee’s confidence that the true effectiveness of the drug is close to its estimated effectiveness.
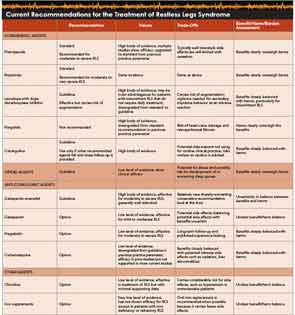
Based on the current evidence, the dopamine agonists pramipexole and ropinirole are the two main treatments for movement disorders. See “Current Recommendations for the Treatment of Restless Legs Syndrome,” below.
Along with these recommendations, the practice parameters list a number of agents for which no recommendations are given. One of these agents, rotigotine, was taken off the market in 2008 due to inconsistent dosing. However, rotigotine has been upgraded from a “no recommendation” to a “guideline” recommendation based on the availability of a new formulation of the patch that now meets FDA approval (Sleep. 2012;35:1037).
Caution with Long-Term Use of Dopamine Agonists
According to Dr. Shangold, the main differences between the 2004 and 2012 updated practice parameters is the shift in the level of recommendation given to the medications used to treat RLS. He emphasized that although the evidence accumulated over the past eight years shows that the medications with a standard recommendation—the dopaminergic agents—have a high benefit with minor risks, they do still carry risks. “This is our dilemma,” he said. “How many otolaryngologists are comfortable prescribing dopamine-agonists, which are neurological drugs? I’m not sure many of us will be using these commonly.”
Dr. Shangold’s discomfort is warranted. According to Dr. Aurora, one concern raised during the evaluation of the literature on the dopamine agonists was their long-term use. Studies have shown that patients on dopamine agonists can exhibit behavioral disturbances over time, such as pathologic gambling, shopping, eating or hypersexuality. These medications can also lead to augmentation, a worsening of the RLS symptoms. The concern over this potential long-term adverse effect is briefly touched on in the conclusion of the practice parameters. The authors state, “It is worth noting that the late development of augmentation (even after one year of continuous therapy on dopaminergic agents) remains a significant concern, and patients need to be monitored throughout therapy for this particular side effect.”
Dr. Wardrop highlighted the need for otolaryngologists to be aware of these potential complications. “Even if you don’t treat someone for RLS, you need to be aware of the side effects of these medications,” she said.
For Richard P. Allen, PhD, research associate in the department of neurology at Johns Hopkins University in Baltimore and a member of the International Restless Legs Syndrome Study Group (IRLSSG), recognition that the short-acting dopamine agonists ropinirole and ramipexole make RLS worse when used as chronic treatment over a period of years is a major advancement in treatment that was not adequately addressed in the practice parameter. He said gabapentin enacarbil and rotigotine are now better options for first-line treatment of RLS. “These should be seriously considered to avoid the significant worsening of RLS seen with long-term treatment using the current short-acting dopamine agonists.”
Dr. Wardrop agreed that gabapentin enacarbil and rotigotine may turn out to be better first-line treatment choices for RLS. However, she emphasized that both medications are relatively new, implying that longer-term evidence is needed before a standard recommendation can be given to use these drugs as first-line treatment.
Dr. Shangold pointed out that in practice many otolaryngologists already choose gabapentin enacarbil as first-line treatment because it is more familiar to them and carries fewer side effects. Use of rotigotine may also increase now that it has once again been approved by the FDA and is back on the market, he said.
Potential Application to General ENT Practice
Although most otolaryngologists who do not also practice sleep medicine may never see patients who complain of RLS, most do treat patients for sleep apnea, and some of these patients may have problems with RLS or PLMD that will need to be treated along with the sleep apnea.
One way for otolaryngologists to determine the potential for RLS and PLMD is to look more comprehensively at the information they obtain from a sleep study conducted on a patient with suspected sleep apnea. Although RLS is determined only by clinical history (see “Diagnosing Restless Legs Syndrom, left), periodic limb movements (PLM) are diagnosed using sleep studies. According to Dr. Shangold, 85 percent of patients with RLS will show PLM in a sleep study, whereas a much smaller percentage of patients with PLM detected on a sleep study will have RSL as determined by history. “In my mind, PLMD is the motor manifestation of RLS, and RLS is the sensory component,” said Dr. Shangold.
Dr. Shangold, who taught an instructional course on sleep studies with Dr. Wardrop at September’s annual AAO-HNS meeting in Washington, D.C., emphasized that many physicians only look at the apnea-hypopnea and respiratory disturbance indices on a sleep study. “There is so much more information on a sleep study, including periodic limb movement,” he said, adding that although periodic limb movements during sleep are quite common, PLMD is quite rare. The disorder is diagnosed if the limb movements at night are contributing to excessive daytime sleepiness and there are no other causes, he said.
“If you see a significant number of limb movements on a sleep study and you don’t have a root cause for excessive daytime sleepiness, that is when the light bulb goes on,” he said. Additionally, he said, the treatment of PLMD is similar to that of RLS.
Dr. Allan also recommends that otolaryngologists look for RLS symptoms, noting that RLS occurs in a reasonable number of sleep apnea patients and in a very high number of patients with chronic obstructive pulmonary disease. He emphasized that treatment of RLS symptoms in sleep apnea patients may be necessary to help their patients sleep well at night. “Current approved medications for RLS are not known to increase sleep apnea and have been used with sleep apnea patients,” he said, but added that opioids, which are sometimes used, may exacerbate sleep apnea.
Leave a Reply