CHICAGO—Investigators from around the country presented their findings at the 119th Annual Meeting of the Triological Society, held here May 21-22, 2016, in conjunction with the 2016 Combined Otolaryngology Spring Meetings. Here are some research highlights from the event.
Medical Spending

zimmytws; Monkey Business Images; Dean Drobot/shutterstock.com
Alden Folsom Smith, BMus, a researcher from Fox Chase Cancer Center in Philadelphia, presented his analysis of the geographic variation in Medicare spending. He and his colleagues began their research by hypothesizing that Medicare expenditures for otolaryngology physician services are affected by the regional location of the Medicare beneficiary. To address this hypothesis, their cross-sectional study averaged expenditures for otolaryngology physician services in each hospital referring region (HRR). They utilized the work relative value units (wRVUs) collected by otolaryngologists and divided them by a thousand Medicare beneficiaries in the region (wRVUs/kMCB). While the expenditures by HRR did not change over the two-year period, Smith reported a marked variation in wRVUs/kMCB among HRRs for otolaryngologist services.
Additionally, the researchers found that the relative supply of otolaryngologists, medical specialists, and primary care physicians was strongly associated with the regional expenditures on otolaryngology physician care. The great variation in the supply of otolaryngologists in the regional physician specialty mix was thus driving the differences in regional Medicare expenditures.
Sigsbee W. Duck, RPh, MD, an otolaryngologist with the Sweetwater Medical Group in Rock Springs, Wyo., led a discussion following the presentation, during which he acknowledged the regional variation. “You have more Medicare supply with older physicians and hospital-employed physicians,” he said.
Smith suggested that future studies should address the effect of an otolaryngology residency training program on Medicare spending.
Bottom line: The relative supply of otolaryngologists, medical specialists, and primary care physicians is strongly associated with the regional expenditures of otolaryngology physician care.
Acute Specialty Care
zimmytws; Monkey Business Images; Dean Drobot/shutterstock.com
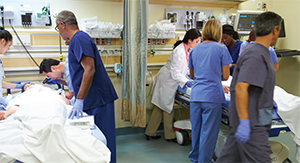
Matthew R. Naunheim, MD, MBA, resident at Massachusetts Eye and Ear in Boston, presented on the role of acute care in otolaryngology. He explained that, typically, acute otolaryngologic care is provided in emergency rooms (ERs), urgent care, primary care, or otolaryngology offices. There are, however, a few dedicated otolaryngology ERs, one of which is the ophthalmology- and otolaryngology-specific ER at Massachusetts Eye and Ear.
Dr. Naunheim and his colleagues designed the study to determine the value of acute otolaryngology services, measuring health outcomes achieved per dollar spent. The researchers approached the question using contingent valuation, explaining that “goods and services that have no explicit market value can still be valued using contingent valuation.” Contingent valuation directly assesses patient preferences, thereby valuing perceived health outcomes. The study authors distributed a survey of 17 questions to 327 patients to assess demographics as well as valuation of care. The valuation questions explained scenario benefits of specialty care versus general care.
The survey responses revealed that the reputation for specialty care was the most common reason that patients presented to their specialty ER. Patients were willing to pay an average of $340 per visit but, said Dr. Naunheim, “A certain number of patients were not able to answer this question.”
He concluded that contingent valuation and willingness to pay can be used to determine the value of surgical services and that patients desire direct access to specialists.
Bottom line: Patients place an explicit value on specialty emergency services of $340 per visit on average. Ultimately, contingent valuation data using willingness to pay methodology may help inform statewide resource allocation and the availability of direct-to-specialist care.
Wrong Site Surgery
Yarah M. Haidar, MD, a resident at the University of California in Irvine, explained that while the Joint Commission has been tracking wrong site surgery (WSS) cases since 1995, it does not mandate that hospitals report all incidences of WSS. The California Department of Public Health (CDPH), however, does require WSS reporting, and Dr. Haidar presented her team’s retrospective analysis of original WSS reports to the CDPH from 2007 to 2014. The team’s analysis, which focused on 95 cases, found that the most common source of WSS was orthopedic surgery (35%), while the most common site was the knee (7%). The CDPH also documented three otolaryngology cases. The first was a Baha case that was noticed after incision. The second was a stapedotomy that was noticed after the middle ear was entered and the stapes were noted to be mobile. The third was a postauricular lipoma resection that was noticed by the patient.
Dr. Haidar offered several suggestions to avoid WSS, including calling for the patient or family to verify the surgical site during the perioperative encounter; however, in a discussion following the presentation, Dr. Duck said, “I really don’t know if we can completely stop this problem. We must continue to follow the established protocols and be acutely aware that wrong site surgery does occur.”
Bottom line: While otolaryngology has a low incidence of reported wrong site surgery, proper communication among team members in the perioperative setting and adequate medical record keeping should be reinforced to curb occurrences. Additionally, correct marking of the surgery site, identification of the wrong site separately, and adherence to universal surgical safety protocols may substantially reduce the rate of WSS.
Should the ESS Questionnaire Be Self Administered?

zimmytws; Monkey Business Images; Dean Drobot/shutterstock.com
In the majority of cases, the ESS questionnaire is self administered by the patient. An ESS score of 10 or higher is considered to be a predictor of obstructive sleep apnea (OSA). Lauren B. Bonzelaar, MD, of Rush University Medical Center in Chicago, posed the following question: Should the ESS questionnaire really be self administered? For example, she noted that the questionnaire includes questions such as, “How likely are you to doze in the following situations?” The research team hypothesized that patients may be in denial about their daytime sleepiness levels. If this is the case, then the accuracy of the ESS could be improved by having a close friend or family member who is aware of the patient’s daytime sleepiness fill out a second ESS questionnaire.
Dr. Bonzelaar and her colleagues hypothesized that ESS scores might differ if the questionnaire were filled out by a partner or friend of the patient rather than the patient. Their retrospective chart review of 100 patients compared the ESS score
obtained from a patient with the ESS score obtained from the patient’s friend or partner. The patients were suspected of having OSA, and the questionnaires were completed as part of standard practice upon completion for sleep apnea treatment in an otolaryngology clinic. On average, partners rated the patient higher than the patient rated himself. She concluded that the ESS questionnaire should be filled out with a partner or roommate in order to create a consensus of scoring.
Bottom line: The difference in mean ESS score obtained from the patient compared with the score obtained when a friend or partner fills out the form implies that this diagnostic form should be filled out by the patient in the presence of a partner/friend. A consensus by the patient and the friend may provide a more accurate score.
Improved Treatment of OSA
lightspring/shutterstock.com
Respiratory stress from nighttime OSA causes concern for many reasons, one of which is that it leads to increased cardiovascular risk. Continuous positive airway pressure (CPAP) is an effective treatment for OSA only if the patient uses the device. Research has shown that nasal surgery can reduce the mean therapeutic CPAP pressure and increase compliance.
Taken together, these facts lead to the question, Is nasal surgery a cost-effective way to increase compliance?
Judith S. Kempfle, MD, postdoctoral fellow at Massachusetts Eye and Ear Infirmary in Boston and her colleagues performed a two-way sensitivity analysis to identify patients for whom septoplasty is cost-effective. They found that, across a range of plausible values in a clinically relevant decision model, nasal surgery is a cost-effective strategy for increasing CPAP compliance.
Bottom line: Across a range of plausible values in a clinically relevant decision model, nasal surgery is a cost effective-strategy to improve CPAP adherence in OSA patients with nasal pathology.
Lara Pullen is a freelance medical writer based in Illinois.