 TRIO Best Practice articles are brief, structured reviews designed to provide the busy clinician with a handy outline and reference for day-to-day clinical decision making. The ENTtoday summaries below include the Background and Best Practice sections of the original article. To view the complete Laryngoscope articles free of charge, visit Laryngoscope.
TRIO Best Practice articles are brief, structured reviews designed to provide the busy clinician with a handy outline and reference for day-to-day clinical decision making. The ENTtoday summaries below include the Background and Best Practice sections of the original article. To view the complete Laryngoscope articles free of charge, visit Laryngoscope.
Background
Peritonsillar abscess (PTA) is one of the most common deep space head and neck infections. Standard treatment involves drainage of the abscess through formal incision and drainage, needle aspiration, or quinsy tonsillectomy, followed by antibiotic therapy. Our knowledge of PTA’s pathogenesis and best management is supported by a limited amount of reliable evidence. Once thought to be secondary to acute tonsillitis, more recent studies have suggested that there may be multiple predisposing factors, including blocked Weber glands, smoking, periodontal disease, compromised immunity, and previous antibiotic use. These may contribute to the development of PTA and may impact the type of bacteria associated with it. Many studies have recommended broad-spectrum antibiotic therapy based on abscess microbiological data but have lacked information on patient outcomes. Fewer studies have evaluated the effect of various antimicrobial regimens on the resolution of a PTA. This article reviews these studies and offers the best available evidence supporting specific antibiotic treatment of PTA in otherwise healthy adults following drainage.
Best Practice
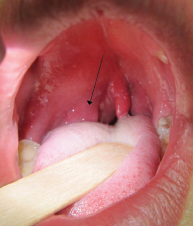
Right-sided peritonsilar abscess.
© James Heilman, MD
The accumulation of evidence on the microbiology of PTA has resulted in recommendations for specific antibiotic utilization. The bacteria identified range from group A streptococcus, to anaerobic organisms, to several β-lactamase–producing species. The studies we cite examined antibiotics as independent variables in the treatment of PTA, and all found that patients treated with drainage and penicillin alone had comparable outcomes to those treated with drainage and broad-spectrum or multiple antibiotic regimens. The route of administration of penicillin appears to be based on patient compliance or inpatient routines, rather than evidence supporting IV versus oral effect on outcome. It should also be noted that the earlier studies may not have been sufficiently powered to find increases in treatment failures, if there were any. Despite this, the findings of all the reviewed studies were consistent.
Why patient abscesses have resolved after treatment with drainage and penicillin alone, despite the identification of penicillin-resistant organisms in the aspirates, remains an empirical question. A possible explanation may be that an adequately drained PTA does not require antimicrobial therapy for resolution. However, the frequent finding of group A streptococcus in PTA aspirates supports the use of penicillin to prevent the possibility of rheumatic or other streptococcal complications. Such complications, though infrequent, are serious. Future research into this question may be more valuable than head to head comparisons of more elaborate antibiotic regimes. The accumulation of evidence to date supports a recommendation that penicillin alone is the only antibiotic necessary, in addition to drainage and supportive care, in the routine management of an otherwise healthy adult with a PTA (Laryngoscope. 2018;128:297–298).