The way David J. Terris, MD, performs thyroid and parathyroid surgery today bears almost no resemblance to the way he learned to do it in residency 15 years ago-but with the strides being accomplished in robotic surgery, there could be another sea change in techniques that might make his work today obsolete as well.
In a series of lectures by a panel at the 111th annual meeting of the Triological Society meeting, Dr. Terris, Porubsky Professor and Chairman of the Department of Otolaryngology at the Medical College of Georgia in Augusta, described the current state of thyroid surgery, when performed with endoscopic techniques, as a drainless, sutureless outpatient procedure.
He and his team perform about 150 to 200 thyroid procedures a year, he said, and about one-third of these operations are done with the endoscope, safely removing lesions in low-risk patients with barely a discernible scar after a short healing period.
In the previous articles in this series for ENT Today, Dr. Terris and his panel reported on work in four areas of surgery where minimally invasive procedures were changing the playing field in a variety of treatments. Researchers discussed endoscopic skull base surgery and use of sentinel node biopsy that may prove useful in sparing patients of the need for neck dissection.
We are witnessing a very rapid change in how thyroid surgery is done, Dr. Terris said. Many of these advances have been technologically driven. Whether it is in new devices or in image guidance, the operation of thyroidectomy has been effectively transformed. In addition, parathyroid surgery bears very little resemblance to the way I was trained to do that operation just 15 years ago.
When doctors find a patient who is ideal for the endoscopic approach to thyroid surgery, the patient will undergo an incision of about three-quarters of an inch, and the operation can be managed through this small access point without damaging major blood vessels or impinging on critical nerves.
We don’t use drains on these patients at all, Dr. Terris said. We don’t use sutures for the skin. It is almost always outpatient surgery, even in total thyroidectomy patients. It can be done under local anesthesia in carefully selected patients.
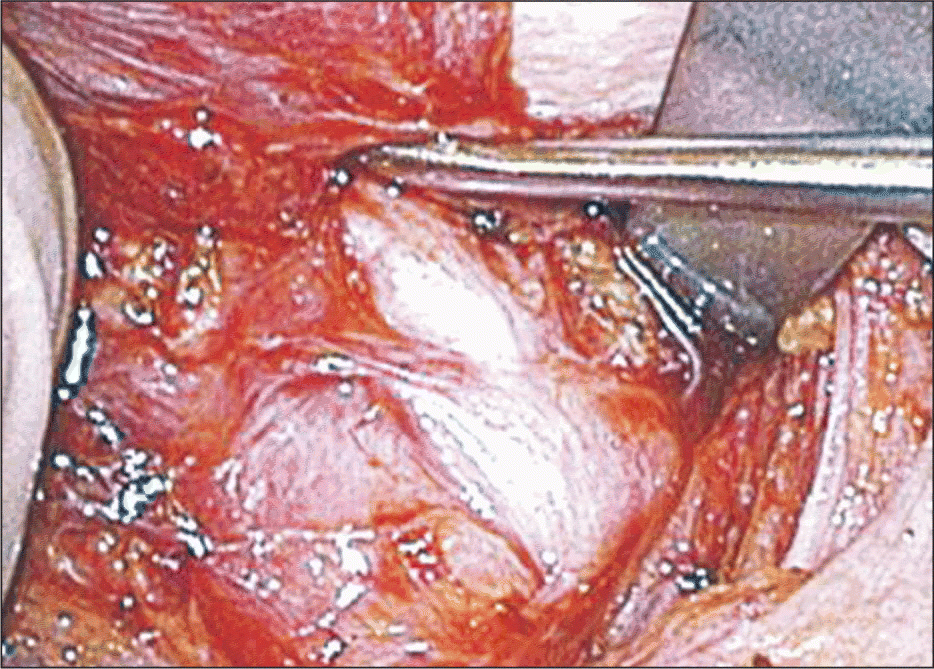
In his presentation, Dr. Terris showed several film clips of actual procedures to give a sense of what a doctor is looking at when performing endoscopic surgery. He described the removal of a left-sided lesion, pointing out the ease of identifying nerves with endoscopic magnification. He also narrated the ligation of the superior thyroid artery using ultrasound-based devices.
In a matter of five or six seconds, the vessel is completely and reliably ligated. The device generates a little bit of steam that can be evacuated, he said. We then look to secure the thyroid vein in exactly the same way. We can get to within one or two millimeters to the nerve with temperatures that are reached that are so much lower than with electric cautery. The nerve dissection is done off the monitor.
We use blunt elevators and-in a significant departure from the way I was trained-we dissect perpendicular to the direction of the nerve. I was trained to dissect parallel to the nerve, he said. The use of the blunt elevators allow for the thyroid to be retracted medially.
It is far easier and gentler on the nerve to identify it that way, Dr. Terris said. Once the gland is exteriorized, we follow it all the way to the junction with the larynx to make sure the nerve is not injured.
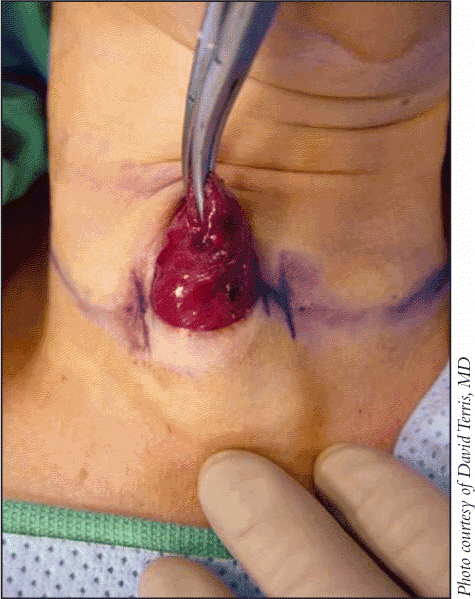
He showed before-and-after pictures of one patient-a pediatric nurse in his institution who underwent the surgery. The evidence of the operation was virtually undetectable. Obviously, these surgeries heal quite well, he said. He made the incision low in the neck-about 20 mm in length-and was able to safely remove the thyroid gland.
Technology Advances Enable Change
What has allowed us to accomplish these beautiful access techniques has been changes in technology, Dr. Terris said. Advanced energy devices, whether it be a laser device or an ultrasonic device, have certain advantages. The ultrasonic devices reach temperatures of 70 to 100 degrees Celsius, which is enough to ligate blood vessels but not as high as you get with electrocautery. That’s the safety factor. Another advantage is that it is very efficient. It lets you ligate and cut in a single step rather than with the suture technique. In addition to ligating and cutting, now you can actually dissect with this instrument. That has increased our efficiency, which has cut down our time in surgery. It is nearly bloodless surgery. If we lose more than 5 cc of blood on a case, it is unusual. I like the fact that there is nothing left in the wounds. There are no clips, there are no silk ties. Because of the confidence in hemostasis, we are able to get away from using drains; we are now doing about 70 percent of our cases on an outpatient basis.
Dr. Terris said that changes in imaging technology-particularly, advances in ultrasound visualization-in the mid-1990s have allowed us to use a targeted approach to parathyroid surgery, and this gives us the confidence of having performed a complete resection.
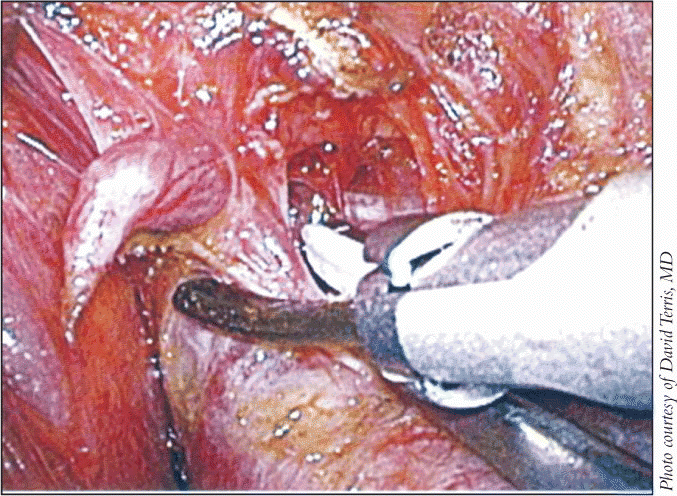
In the surgery procedure itself, he illustrated how the use of blunt elevators allows doctors to perform an atraumatic dissection in the region where the site of the adenoma is anticipated. We are really looking for a color change associated with an adenoma, he said. It’s kind of a purplish hue. Once the adenoma is identified, then it is a matter of gently dissecting around the gland. The gland really wants to come out. You just have to help it a little bit.
 We are witnessing a very rapid change in how thyroid surgery is done. Many of these advances have been technologically driven. Whether it is in new devices or in image guidance, the operation of thyroidectomy has been effectively transformed.
We are witnessing a very rapid change in how thyroid surgery is done. Many of these advances have been technologically driven. Whether it is in new devices or in image guidance, the operation of thyroidectomy has been effectively transformed.
-David J. Terris, MD
In the case he described, the large adenoma made it necessary for the surgeon to deal with the major nerve in the area. To make sure that nerve is not injured, we identify it, trace it out, and dissect it away from the adenoma, so we can retract the adenoma laterally in this case, Dr. Terris explained. It is a process of gentle blunt dissection to mobilize that nerve away from the adenoma.
We usually find the end artery of the adenoma. We could use the harmonic device, but we usually find that there is just one blood vessel that we are ligating for this entire operation, so I think it is hard to justify a $300 handpiece just for that. So we use an endoscopic clip. We fire three clips-two on the patient side and one on the adenoma side-and we divide the artery between these clips. Once that is done, the adenoma is devascularized.
The surgery can be performed in such a manner that the patients recover rapidly, and almost all of them are discharged the day of the operation. I think we are enjoying the benefits of technology in that there is a high rate of cure even in less-experienced hands, Dr. Terris said. In the old days, it was more important to have an experienced parathyroid surgeon. Now I think that even in less experienced hands, we are finding quite good results.
The next article in this series will provide tips to practitioners of endoscopic surgery.
©2009 The Triological Society
Leave a Reply