The first balloon catheter was approved by the Food and Drug Administration (FDA) for intranasal use in 2005. Since then, at least four other medical devices have received FDA approval for balloon sinus ostial dilation, and balloon sinuplasty rates have increased dramatically. In 2011, the first year a distinct Current Procedural Terminology (CPT) code was available for balloon dilation, stand-alone balloon sinuplasty accounted for 5% of sinus procedures performed on patients with chronic rhinosinusitis. By 2014, that number had risen to 22.5% (Int Forum Allerg Rhinol. 2017;7:600–608). Nationally, the use of balloon dilation increased greater than five-fold, while the use of endo-scopic sinus surgery only increased by 5.9% (Laryngoscope. Published October 8, 2017;doi:10.1002/lary.26941).
The fact that balloon sinuplasty rates increased so dramatically while sinus surgery rates remained stable led to speculation about inappropriate usage. “When you look at balloon dilation usage data, you can see that there are certain hotspots in the country that are doing a vast number of these,” said Nadim Bikhazi, MD, an otolaryngologist in private practice in Ogden, Utah. “One of the concerns has been, is it really being used for the right indications in the right fashion?”
The first-ever clinical consensus statement on balloon dilation of the sinuses aims to ensure patient safety and proper utilization. The document was approved by the American Academy of Otolaryngology–Head and Neck Surgery Foundation (AAO–HNSF) board of directors and published in February 2018 (Otolaryngol Head Neck Surg. 2018;158:203–214). The statement examines 58 clinical statements regarding patient criteria, perioperative considerations, and outcomes.
“Balloon dilation of the sinuses is an evolving technology that has been shown to have benefit in a number of circumstances,” said James C. Denneny III, MD, executive vice president/CEO of the American Academy of Otolaryngology–Head and Neck Surgery. “As with most evolving technologies in the field of medicine, it’s important to have a blueprint to objectively look at things. Everyone’s end goal is to have a very safe, effective treatment for patients.”
Expected Impact
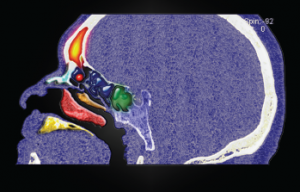
Sinus osteoma.
© Living Art Enterprises / Science Source
According to the consensus statement, balloon dilation is an appropriate treatment for patients who have sinonasal symptoms and positive findings on a CT scan. It can also be used as an adjunct to functional endoscopic sinus surgery (FESS) and may be used in patients who have persistent sinus disease despite previous sinus surgery. There is also a role for balloon sinus dilation in managing patients with recurrent acute sinusitis.
There is already evidence that the clinical consensus statement may lead to improved health insurance coverage for balloon sinuplasty. Shortly after the statement’s release, Anthem changed their classification of balloon sinus ostial dilation from “investigational” to “medically necessary” for patients who meet the criteria outlined in the consensus statement.
Expanded health insurance coverage of balloon dilation is a “win-win-win scenario,” Dr. Bikhazi said. It’s a win for patients, because appropriate candidates can undergo an in-office procedure at a lower cost and with decreased risk of complications. It’s a win for physicians because they can receive reimbursement while treating patients in accordance with best practices; insurers win because patients can be treated in the lowest-cost setting.
Previously, patients who could not afford to pay out of pocket for balloon sinuplasty often opted for insurance-covered sinus surgery. “Having to take them to the operating room when I did not need to is just ridiculous,” Karen Stierman, MD, an otolaryngologist with the ENT & Allergy Center of Austin. “Now that more insurances cover in-office balloon procedures, people who have sinusitis without polyps can be considered for an office-based balloon procedure and avoid general anesthesia.”
According to the consensus statement, however, balloon sinuplasty is not appropriate for the management of sleep apnea or headache in patients who do not otherwise meet the criteria of chronic sinusitis or recurrent acute sinusitis. That news may be disappointing to patients interested in balloon dilation for those indications.
“I have people come to my office and say, ‘Can I have a balloon dilation to fix my breathing? Or to fix my sleep apnea?’ because that’s how it’s being marketed in some places,” Dr. Stierman said.
The lack of inclusion of these indications in the consensus statement “does not say that balloon dilation has no potential value or does not work in individual cases,” for barotrauma and headaches, Dr. Denneny said. Rather, “at this time, this is not a substantial body of scientific evidence that rose to the level of consensus for these other disease processes as it did for chronic rhinosinusitis,” he said.
Balloon dilation of the sinuses is an evolving technology that has been shown to have benefit in a number of circumstances. As with most evolving technologies in the field of medicine, it’s important to have a blueprint to objectively look at things. Everyone’s end goal is to have a very safe, effective treatment for patients. —James C. Denneny, III, MD
Additional Research Is Necessary
The consensus statement will be updated at least every three years to reflect new knowledge. For instance, although otolaryngologists have been using balloon technology to dilate the frontal, maxillary, and ethmoid sinuses for years, the only location-specific outcome statement that reached consensus is, “Balloon dilation can be effective in front sinusitis.” Dr. Bikhazi said that may be because there’s not yet evidence to suggest that balloon dilation is a superior choice for maxillary sinus disease, as compared with sinus surgery. However, based on his experience with the REMODEL study, which showed that stand-alone balloon dilation is as effective as FESS in the treatment for CRS in patients with maxillary sinus disease, Dr. Bikhazi said, “I think maxillary sinus will follow the front sinus recommendation in the future” (Am J Rhinol Allergy. 2014;28:323–329. Laryngoscope. 2016;126:44–50).
This clinical consensus statement “provides a foundation that patients, providers, and insurers can lean on to cover an important problem that is fairly prevalent in our society,” Dr. Denneny said. “It will be adjusted as further research and clinical experience warrant.”
Jennifer Fink is a freelance medical writer based in Wisconsin.
Key Points
- The FDA approved the first balloon catheter for intranasal use in 2005.
- This is the first clinical consensus statement on balloon dilation of the sinuses, and it indicates that the procedure is appropriate for patients with sinonasal symptoms and positive findings on CT scan. It can also be used as an adjunct to FESS.
2018 Clinical Consensus Statement: Balloon Dilation of the Sinuses
1. Balloon dilation is not appropriate for:
- patients who are without both sinonasal symptoms and positive findings on CT;
- the management of headache in patients who do not otherwise meet the criteria of CRS or recurrent acute sinusitis;
- the management of sleep apnea in patients who do not otherwise meet the criteria of CRS or recurrent acute sinusitis; or
- patients with sinonasal symptoms and a CT that does not show evidence of sinonasal disease.
2. CT scanning of the sinuses is a requirement before balloon dilation can be performed.
3. Balloon dilation can be appropriate as an adjunct procedure to FESS in patients with chronic sinusitis without nasal polyps.
4. There can be a role for balloon dilation:
- in patients with persistent sinus disease who have had previous sinus surgery; and
- in managing patients with recurrent acute sinusitis as defined in the AAO-HNSF guidelines based on symptoms and CT evidence of ostial occlusions and mucosal thickening.
5. Balloon dilation can:
- be performed under any setting as long as proper precautions are taken and appropriate monitoring is performed;
- be performed under local anesthesia with or without sedation;
- improve short-term quality-of-life outcomes in patients with limited CRS without polyposis; and
- be effective in frontal sinusitis.
6. Surgeons who consider reusing devices intended for dilation of the sinuses should understand the regulations set forth by the FDA for reprocessing such devices and ensure that they are followed.
Source: Otolaryngol Head Neck Surg. 2018;158:203–214