TRIO How I Do It articles are reviews from The Laryngoscope designed to provide guidance on clinical and surgical techniques and practice issues from experts in the field.
Introduction
Cerebrospinal fluid (CSF) rhinorrhea is a consequence of a breakdown of the layers of the arachnoid membrane, dura matter, the bony skull base and periosteum, and the nasalmucosa (Neurosurgery. 2006;58:246–257). In the past few years, several endoscopic techniques have been described to close ventral skull base CSF leaks. These include local pedicled flaps (e.g., nasoseptal flap [Laryngoscope. 2006;116:1882–1886], turbinates [Laryngoscope. 2009;119:2094–2098]), regional pedicled flaps (e.g., pericranium [Laryngoscope. 2016;126:1736–1738], fascia temporalis [J Neurosurg. 2016;125:419–430]), free grafts (e.g., abdominal fat [Otolaryngol Head Neck Surg. 2016;154:540–546], fascia lata [Otolaryngol Clin North Am. 1984;17:591–599]), microanastomosed free flaps (Am J Rhinol Allergy. 2017;31:122–126), as well as synthetic grafts (ibid). Nowadays, most authors use multiple-layer reconstruction by combining these techniques to improve the success rate of endoscopic skull base reconstruction.
The choice of skull base reconstruction technique depends on the location and the size of the defect, as well as intracranial pressure. The graft can be placed in the extracranial or extradural spaces that are often used, or in the intradural space, which is technically more demanding.
In cases of small-size CSF leaks, we propose a new surgical technique with a good success rate that allows centering the intradural graft adequately on the defect. This “parachute” placement can be used with both autologous free grafts and synthetic materials.
Method
A retrospective chart review was performed to identify patients who had undergone endoscopic-guided transnasal duraplasty for small low-flow CSF leaks (<2 cm) of the ventral skull base at the Lariboisière University Hospital in Paris, France. Leaks that were reconstructed with other techniques were excluded. We report on the surgical technique, graft materials, and outcomes. All patients were imaged preoperatively with skull base computed tomography and magnetic resonance imaging.
The procedure is done under general anesthesia. The patient is positioned supine, with the patient’s head in a neutral position. An anterior and posterior ethmoidectomy is performed, associated most often with a middle turbinate removal. Then, the CSF leak site is identified endoscopically and measured. Site preparation begins by removal of the overlying mucosa. Abrasion of the adjacent and involved bone is generally advocated to stimulate osteoneogenesis. If needed, the bone defect is enlarged to see the limits of the dura defect. Then, an intradural and extradural circular dissection is performed with angled elevators to allow an underlay and overlay placement of the graft.
This “parachute” placement can be used with both autologous free grafts and synthetic materials.
The parachute technique allows the use of both fascia lata and synthetic materials. We present here a skull base reconstruction of a 1.5-cm defect of the planum sphenoidale.
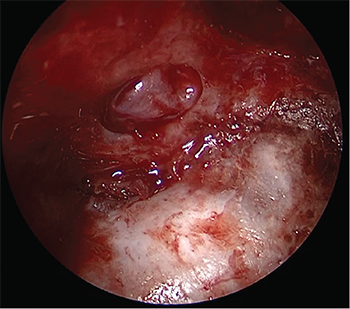
Final view of the two-layer reconstruction using the “parachute” technique.
A Biodesign duraplasty graft (Cook Biotech, West Lafayette, Ind.) in a size that was approximatively 30% larger was designed. A nonabsorbable polypropylene suture (3/0) is passed through the graft near the center in a U shape. The two strands must be long enough to easily exit the nose. Then, the graft is placed in the subdural space using classic microsurgical instruments (angled endonasal blunt hook and seeker, spoon curettes, blunt angled elevators). A slight tension on the strands allows centering the graft on the defect, and then it is applied against the dura without any pucker—hence the name “parachute technique.” It should be noted that the role of the suture is not to anchor the graft but to center it on the defect. The graft is then covered with fibrin glue to seal the reconstruction and the suture is removed, with back pressure being maintained on the graft with a blunt instrument to avoid displacement. Fibrin glue sealing should be used sparingly between the two reconstruction layers to avoid dead space during resorption.
Then, a second graft designed like the first graft is placed in the extradural space, as a “sandwich” to maintain the dura between two graft layers. At the end of the procedure, fibrin glue sealant is applied. With this parachute closure technique, it is possible to associate a multilayer reconstruction using a mucosal graft or mucosal flaps to cover the graft and surrounding bone. We did not use any nasal packing or postoperative antibiotics.
Patients must follow common postoperative advice such as avoiding straining and Valsalva-like maneuvers. Acetazolamide was prescribed only in case of suspicion of intracranial hypertension. We did not use any lumbar drain.
Results
Sixteen patients were included in the study from 2005 to the present. All patients were operated on by the same surgeon.
Iatrogenic CSF leaks were addressed by other centers and then closed during another surgical procedure. The mean postoperative follow-up was 24 months (range = 1–101 months). We did not notice any leak recurrence.