Smaller incisions, fewer complications, and a speedy return home are a few of the advantages otolaryngologists can offer by managing their patients on an outpatient basis or using minimally invasive surgical techniques. These new options are appropriate for selected thyroidectomy or parathyroidectomy patients, according to investigators who presented their findings at the American Academy of Otolaryngology-Head and Neck Surgery Foundation Annual Meeting in Toronto last September.
Outpatient Thyroidectomy
For thyroid patients, minimally invasive surgery can often be managed on an outpatient basis, avoiding overnight hospitalization. We found that it is nicer for patients to convalesce in their own home environment, eating their own foods, and surrounded by their family, said David J. Terris, MD, lead investigator of a study that examined the feasibility of outpatient thyroid surgery. Other advantages include minimizing exposure to hospital-acquired infections, reduced potential for iatrogenic complications, and lower costs.
Dr. Terris led a group from the Departments of Otolaryngology-Head and Neck Surgery and Medicine of the Medical College of Georgia in Augusta in examining the safety of efficacy of outpatient versus inpatient thyroid surgery. In a prospective, nonrandomized study of 91 consecutive patients who underwent thyroid surgery between December 2004 and October 2005, 57% of patients (n = 52) had the procedure on an outpatient basis. Twenty-nine percent (n = 25) underwent 23-hour observation with an overnight stay and were considered inpatients. An additional 14% (n = 13) were admitted to the hospital, for a mean of 3.4 ± days. The outpatient and inpatient groups did not differ significantly by age (44.8 ± 13.3 years vs 48.5 ± 16.3 years) or gender (85% female vs 82% female).
Dr. Terris, who is the Porubsky Distinguished Professor and Chairman of the Department of Otolaryngology at the Medical College of Georgia, performed all surgeries. He used a number of surgical techniques, including Kocher incision, minimally invasive thyroid surgery with access to the thyroid compartment, and endoscopic thyroidectomy. Laryngeal nerve monitoring was used as required, and vocal cord mobility was checked preoperatively and again in the postanesthesia care unit or on the ward using flexible fiberoptic laryngoscopy. In the outpatient group, patients were assessed postoperatively and discharged once they became ambulatory, could tolerate food, and could use oral medications to manage pain. All patients returned within one to two weeks for follow-up assessment, and were requested to return after that if needed.
Forty-two patients underwent hemithyroidectomies, 38 underwent total thyroidectomies, and 11 had completion thyroidectomies. Hemithyroidectomies were usually done on an outpatient basis, while patients were admitted to the hospital for total thyroidectomies. Outcome measures included estimated blood loss, duration of surgery, pathology, admission or readmission to the hospital, and hospital charges.
Our outpatients did very well, commented Dr. Terris. Complication rates were low and comparable for both groups (2 vs 1, p = 1.0). Mean estimated blood loss was lower for outpatients than for inpatients (17.8 ± 14.0 cc vs 29.4 ± 22.1 cc, p = 0.02). No patients suffered permanent recurrent laryngeal injury.
Historically, one of the reasons surgeons have been reluctant to perform thyroid and parathyroid surgery on an outpatient basis is the concern for bleeding, which necessitates the placement of a surgical drain. Use of the Harmonic ACE™, a device that utilizes frictional energy rather than electrical energy, in conjunction with a small incision, has virtually eliminated this worry. We now use the Harmonic ACE exclusively to control blood supply to the gland. It is very hemostatic, and when we’re done, there’s a very dry field, said Dr. Terris. By using the Harmonic ACE and minimal access, we can avoid need for the drain. This eliminates a potential source of postoperative infection. Dr. Terris has given lectures sponsored by the manufacturer of the Harmonic ACE, but has no stock or financial stake in the outcome of the company.
The Harmonic ACE also helps shave operative time by about 20 to 30%. Savings in time by using the harmonic device are offset, in part, by the increased time needed when using a minimally invasive approach.
Another potential drawback to outpatient thyroid surgery is the fear of life-threatening hypocalcemia. To avoid this problem, in a novel approach, patients in this study were placed on a prophylactic calcium supplementation regimen consisting of a 3-week taper of oral calcium carbonate (600 mg TID for the first week, 600 BID for the second week, and 600 every day for the third week), and ionized calcium levels were monitored postoperatively. Even if parathyroid hormone levels were low because of dissection, it didn’t matter because we maintained the calcium level by supplementation, said Dr. Terris.
The typical patient profile for minimally invasive thyroidectomy is the young woman with thyroid nodules of unclear malignant potential or a very low-risk cancer. These patients typically do not have very enlarged glands, says Dr. Terris.
But outpatient thyroid surgery is not for all patients. Inpatient stays are still warranted for medically infirm patients with significant coexisting conditions, patients who have undergone concomitant procedures requiring admission, and patients who may prefer hospitalization. Open incisions are usually necessary for patients with giant goiters.
In practice, Dr. Terris estimates that about 70% of patients who are eligible for ambulatory surgery do go home shortly after surgery. Most, but not all, of these patients have undergone minimally invasive surgery, either endoscopic (3/4″ incision) or minimal access (1-1½″ incision). Even some patients with open surgery are discharged the same day, as long as they are fit, healthy, and do not need a drain.
Minimally Invasive Parathyroidectomy
At the George Washington University Medical Center, otolaryngologist Nader Sadeghi, MD, and colleagues compared minimally invasive parathyroidectomy with conventional open surgical access. These investigators reported that minimally invasive parathyroidectomy, when used for selected patients, is an effective treatment of primary hyperparathyroidism, with distinct advantages for both the patient and surgeon.
Previously, parathyroidectomy required exploration of all four parathyroid glands to identify the abnormal gland and remove it. At least one normal-looking gland had to be biopsied to be sure the patient had only single-gland adenoma, explained Dr. Sadeghi, who is Director of Head and Neck Surgery at GWU. We know that out of all patients with primary hyperparathyroidism, about 85 to 90 percent have single-gland adenoma and only 10 to 15 percent have four-gland hyperplasia as the primary diagnosis. So, for that 85 percent, if you can localize the single abnormal gland, the patient can have only a directed, minimally invasive parathyroidectomy.
In this prospective, noncontrolled study, 100 patients with primary hyperparathyroidism underwent a sestamibi scan and ultrasonography preoperatively to localize the affected parathyroid gland. With a sestamibi scan, an adenomatous parathyroid gland retains the radiolabeled agent, which allows its localization in a great majority of cases. In this study, the sestamibi parathyroid scan had a sensitivity of 90%, a positive predictive value of 97%, and a negative predictive value of 36%. Ultrasound was helpful not only to corroborate the sestamibi images in localizing the parathyroid adenoma, but it also helped to rule out otherwise nonpalpable thyroid nodules that may potentially lead to false positive sestamibi results.
Patients then underwent selective parathyroidectomy using a minimally invasive approach. The average incision for minimally invasive surgery is about 4 cm, compared with an 8 cm average in the standard open approach. More important, far less deep dissection is required to find and excise the abnormal gland.
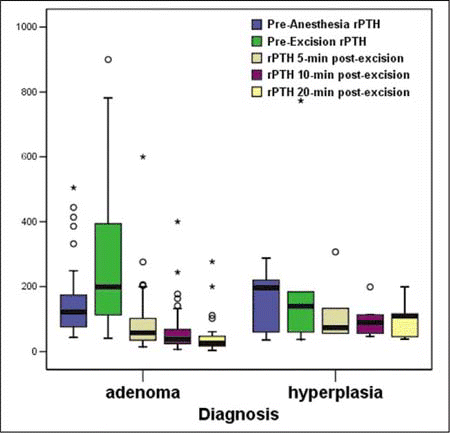
To ensure that the diseased gland was successfully excised, levels of parathyroid hormone (PTH) were assayed preoperatively and intraoperatively. With this measure, elevated PTH levels reflective of hyperparathyroidism would be expected to fall precipitously once the diseased gland is removed; if PTH levels remain high following excision of one abnormally enlarged gland, it suggests that another gland is affected (see graph), or more likely the patient has parathyroid hyperplasia. In this study, postoperative serum calcium levels with a mean follow-up of 11 months and minimum of 6 months were normalized in more than 97% of the patients, confirming the efficacy of the approach. Indeed, 100% of the patients who were managed with single-gland excision with unilateral directed exploration became normocalcemic and remained so.
Dr. Sadeghi reported that 90% of the patients who were diagnosed with single-gland adenoma required only minimally invasive, single-gland exploration. Ten percent of patients having eventually confirmed diagnosis of single-gland disease needed bilateral exploration for nonlocalizing adenoma or false negative imaging.
Minimally invasive parathyroidectomy has made a big difference, said Dr. Sadeghi. It has been shown by numerous studies, including our own, that it has a 97% or more success rate and that we are not compromising success rates as compared to traditional surgery. He said that recurrence rates for both approaches hover around 2 to 3%.
The overall risk of minimally invasive parathyroidectomy is below 1%, compared with 2% or less for standard surgery, said Dr. Sadeghi. Smaller incisions with less dissection mean that patients recover faster, return to work faster, and have better cosmetic outcome. The surgery is performed on an outpatient basis. It reduces the risk of postoperative hypocalcemia, except in few cases of very large adenomas where the other three normal glands are functionally suppressed and the patient may suffer transient hypocalcemia. Calcium supplementation similar to a post-thyroidectomy strategy eliminates this risk. This approach leads to fewer major complications, such as bleeding and hematoma formation.
Minimally invasive surgery also reduces the risk of residual injury to the recurrent laryngeal nerve-a danger of any thyroid or parathyroid surgery. None of the patients in this study suffered any of these complications. Because there is less disturbance of the remainder of the neck and the thyroid bed, and the contralateral side is not dissected at all, it also allows for easier and safer re-exploration in the few cases with persistent or recurrent disease.
Minimally invasive parathyroidectomy also carries no risk of postoperative permanent hypoparathyroidism, or adynamic bone disease. This advantage is due to the improved preoperative localization with imaging, allowing identification and removal of the single adenoma, leaving the other three normal parathyroid glands nondisturbed, intact and functioning.
Outpatient thyroidectomy and minimally invasive parathyroidectomy also carry an additional benefit: cost savings. In Dr. Terris’s study, costs were significantly lower for outpatients ($7,974) than for inpatients ($9,578, p = 0.0006). Although reduced costs are not a compelling reason for surgeons to consider alternatives to traditional patient management, the comparable efficacy findings, improved safety outcomes, and desirable patient benefits demonstrated by these two studies should encourage surgeons to consider minimally invasive and/or outpatient surgery for selected patients with thyroid and parathyroid disease.
©2007 The Triological Society

Leave a Reply