Sialendoscopy has changed my entire approach to salivary obstructive disease, said Barry M. Schaitkin, MD, Associate Professor in the Department of Otolaryngology at the University of Pittsburgh School of Medicine. I think it will take over completely the approach to treating salivary gland stones.
Indeed, the minimally invasive procedure has been proving to be effective for both diagnosis and management of obstructive salivary gland disorders. After 10 years of expansion in Europe,1-4 the technique is now gaining purchase in the United States.5 In properly trained hands, say otolaryngologists and head and neck surgeons, sialendoscopy can be used to effectively manage obstructive salivary gland disorders (especially calculi).
However, cautioned Dr. Schaitkin and two other noted otolaryngologists-one of them a developer of a widely used system-the technique is not a panacea for diagnosing and treating all disorders of the salivary gland, such as salivary tumors. Proper training and careful selection of patients are key to successful outcomes.
Development of the Procedure
Miniaturization of endoscopes and progress in fiberoptic technology enabled several researchers in the 1990s to expand the uses of endoscopy for management of obstructive salivary gland diseases. Francis Marchal, MD, PhD, Associate Professor in the Department of Otolaryngology-Head and Neck Surgery at Geneva University Hospital in Switzerland, was one of those innovators. In the early 1990s, he recalled, endoscopy was being used (notably, by Gundlach and Hopf6) in conjunction with intracorporeal lithotripsy to fragment salivary gland stones. Technical problems (caused by instruments that were too long and fragile) seemed to impede the spread of the technique.
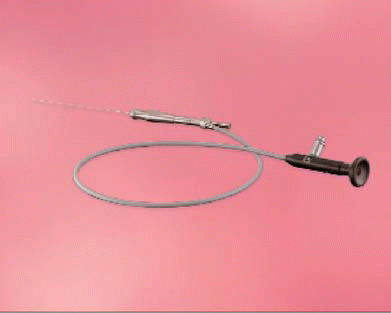
In partnership with the Federal Polytechnic School of Lausanne, Dr. Marchal began to experiment with small-sized flexible endoscopes to see whether it would be possible to have adequate vision of the ductal system, and then to treat people with submandibular obstructions without removing the gland. With these initial forays, visualization into collapsed ducts was very poor. Dr. Marchal tried a 1.5-mm flexible scope with a rinsing system, and found that flushing the gland with saline solution was the key to greater visibility. Finally, he began collaborating with the Karl Storz Company, which had a semi-rigid 1-mm diameter scope. This scope was modified, and various outer sheath systems were designed and customized (tip, curve, etc.) in order to facilitate access to the ducts. A specific surgical technique using various dilators, and specific baskets for stone retrieval, also designed by Dr. Marchal, were set up. The Storz system (the main company manufacturing these scopes) contains a rinsing channel and a working channel with an external diameter ranging from 0.89 mm to 2.2 mm, according to different models of scopes.
Diagnostic sialendoscopy at Geneva University Hospital is usually performed using local anesthesia, whereas interventional sialendoscopy, requiring some degree of sedation, is often performed with an anesthetic standby. After lavage, it is possible to view primary, secondary, and even tertiary ducts to allow for diagnosis of stones and ductal stenosis. Stones up to 3 mm in the parotid and 4 mm in the submandibular glands can be extracted using a metallic wire basket. If stones are larger, intracorporeal laser lithotripsy is employed to fragment the stones, and the fragments can then be removed.
There are many advantages of this procedure over sialadenectomy, noted Dr. Schaitkin: no scar; elimination of facial nerve paralysis of the marginal mandibular branch; and lower morbidity, especially for older patients with co-occurring disorders. (Because sialendoscopy is performed on an outpatient basis, older patients can be maintained on their anticoagulant therapies.) Since the use of sialendoscopy began in Geneva 12 years ago, the submandibular resection rate has dropped by 80%, Dr. Marchal reported.
Learning Curve
Sources interviewed for this article emphasized that training basics should include a formal course. It would be a great mistake to buy an endoscope and start, said Dr. Marchal. I can cite many examples of people having done that, and then having problems. It’s not that it’s so complicated, but there are so many little tricks.
At the European Sialendoscopy Training Centre (ESTC) in Geneva, where 480 physicians from 43 countries have been trained since 2002, surgeons first practice the technique on fresh pigs’ heads to master the instrumentation and navigation in the duct. (For more information, go to www.sialendoscopy.net/.)
David W. Eisele, MD, Professor and Chairman of the Department of Otolaryngology-Head and Neck Surgery at the University of California, San Francisco, whose primary practice is in head and neck cancer, has achieved good results since adding sialendoscopy to his armamentarium following the course in Geneva.5 At UCSF (www.ucsf.edu ), Dr. Eisele performs sialendoscopy under general anesthesia in the operating room. He believes that once surgeons master the technique in a course setting, it’s pretty easy to translate those skills into the operating room. However, he said, when you’re in the operating room, you must be prepared to deploy other options-for instance, in some patients, it may be too difficult to dilate the opening to insert the scope. A sialodochotomy may be required for insertion of the scope. (Dr. Marchal has also published descriptions of his combined endoscopic and external approach for extracting large stones.7)
Dr. Schaitkin agreed that the most difficult part of the learning curve is inserting the scope. (Other authors have described some new technical tricks.8) The papillae of the ducts are so very small. Even though the scopes you are inserting are 1.3 to 1.6 mm-and that sounds tiny-you still have to dilate the opening to be able to accept that instrument. The first 20 cases are difficult, and it gets easier after that.
Patients’ consent forms include the possibility of gland removal should the surgeon be unable to access the gland endoscopically, said Dr. Schaitkin, who also learned sialendoscopy at the ESTC. Dr. Schaitkin and Ricardo L. Carrau, MD, Professor of Otolaryngology at the University of Pittsburgh School of Medicine, have, with Dr. Marchal’s assistance, established an American Sialendoscopy Training Center (ASTC), that aims to train-as did the ESTC-American physicians interested in learning the technique. The next American course will be held November 9, 2008, in Pittsburgh (https://ccehs.upmc.edu/formalCourses.jsp ). The next European course will be held October 9-11, 2008, in Geneva (www.sialendoscopy.com ).
Good for Which Patients?
Patients with suspected sialolithiasis comprise the major population for whom sialendoscopy is indicated. Dr. Marchal has now published a series on treating children with obstructive salivary gland swelling, and has shown that the technique has greater diagnostic sensitivity than conventional radiology, ultrasound, and MRI.9 Although larger series with longer-term follow-up are needed to confirm these results, Dr. Marchal believes that the future for this procedure is bright.
In addition, those with stenotic disease, inflammatory conditions (such as Sjögren’s syndrome or recurrent parotitis of childhood), or radioiodine-induced sialadenitis may also be candidates for diagnostic sialendoscopy. Dr. Eisele has observed a therapeutic benefit of doing sialendoscopy in the last group of patients. Dr. Schaitkin reported that at his center, patients with inflammatory conditions are treated primarily with lavage and intraglandular deposition of steroids for localized control of the inflammation.
Dr. Marchal said he exercises extreme caution in cases of infection of the duct. I’ve always said this is a contraindication, because the ductal walls are more fragile when they are inflamed and can be perforated more easily. It’s always delicate to push fluid into an area where there is already an infection; it may push and spread the infection further. In good hands, if you have good experience, this may be all right, but trying to introduce this as standard therapy might be dangerous.
If You Offer It, Will They Come?
Dr. Eisele doubts that sialendoscopy will be hugely applicable in every general otolaryngology practice. The equipment is expensive and, he said, there are relatively small numbers of eligible patients in the United States compared with those in series reported from Europe. The results of 77 patients who underwent sialendoscopy between 2004 and 2007 at UCSF Medical Center were recently reported.5 Dr. Eisele and colleague Amol M. Bhatki, MD, reported a 73% success rate of stone removal, with minimal complications. They have now completed 106 procedures in 85 patients since they began to do the procedure in the fall of 2004. I am doing perhaps 30 to 40 procedures a year at this point in time, he said. I think the prevalence of the disorder that is the primary indication for this procedure-sialolithiasis-is less in the United States compared to Europe.
However, Dr. Marchal-who sees more than five new cases a week at his center-believes that there is a reservoir of patients in the United States as well as in Europe, and that the use of the technique here could follow a similar trajectory to the one he has observed in Switzerland. The larger numbers of cases in Europe are more a function of the procedure’s longer track record and greater availability than to a greater incidence of salivary stones, he believes. Epidemiological analyses done by his center and other researchers have not established causative links between diet and/or water hardness and incidence of sialolithiasis. For instance, he said, We could not find any difference in calcium absorption-due to ingestion of dairy products in Switzerland-and people having stones.
Dr. Marchal has concluded that the success of sialendoscopy in Europe is due to concerted and ongoing reporting of studies as well as education-of his colleagues, the general public, and referring physicians. This pathology is widely underestimated, because the reservoir of patients is kept by the GP, he said. It is those physicians, he said, who warn their patients against surgery because of the history of complications following the older treatments of gland excision.
The real truth is that when you start showing people there is a treatment for something for which there was no noninvasive treatment, patients start to appear, he asserted.
Whether or not the European experience will be duplicated here, Dr. Eisele said that its minimally invasive nature means that sialendoscopy will increasingly offer real benefits to patients. It does require a little more sophisticated equipment-and time-but I think it’s well worth it, he said. Dr. Schaitkin agreed: There’s no doubt in my mind that for stones it’s amazing-for stones, it’s a home run!
References
- Marchal F, Dulguerov P, Lehmann W. Interventional sialendoscopy. N Engl J Med 1999;341:1242-3.
- Marchal F, Dulguerov P, Becker M, Lehmann W. How I do it: interventional sialendoscopy. Laryngoscope 2000;110(2 Pt 1):318-20.
- Marchal F, Dulguerov P. Sialolithiasis management: the state of the art. Arch Otolaryngol Head Neck Surg 2003;129:951-6.
- Becker M, Marchal F, Becker C, Dulguerov P, Georgeakopoulos G, Lehmann W, Terrier F. Sialolithiasis and salivary ductal stenosis: diagnostic accuracy of MR sialography with a three-dimensional extended-phase conjugate-symmetry rapid spin-echo sequence. Radiology 2000;217(2):347-58.
- Bhatki AM, Eisele DW. Diagnostic and therapeutic sialoendoscopy [sic] in the treatment of obstructive salivary gland disorders. Presentation, Western Section, Triological Society annual meeting, 2007.
- Gundlach P, Hopf J, Linnarz M. Introduction of a new diagnostic procedure: salivary duct endoscopy (sialendoscopy) clinical evaluation of sialendoscopy, sialography, and X-ray imaging. Endosc Surg Allied Technol 1994;2(6):294-6.
- Marchal F. A combined endoscopic and external approach for extraction of large stones with preservation of parotid and submandibular glands. Laryngoscope 2007;117 (2):373-7.
- Chossegros C, Guyot L, Richard O, Barki G, Marchal F. A technical improvement in sialendoscopy to enter the salivary ducts. Laryngoscope 2006;116(5):842-4. (IF:1.51).
- Faure F, Froehlich P, Marchal F. Paediatric sialendoscopy. Curr Opin Otolaryngol Head Neck Surg 2008;16(1):60-3.
©2008 The Triological Society

Leave a Reply