TORONTO – When it comes to performing surgery for obstructive sleep apnea (OSA), there are a variety of procedures that can be done, but otolaryngologists sometimes have personal preferences, and preferences can affect everything from how diagnoses are made to the type of surgery performed, often with similar end results. At the same time, some of the options available are limiting and better treatments need to be found.
These were among the issues discussed at the panel Clinical Insights in Sleep Surgery at the annual meeting of the American Academy of Otolaryngology-Head and Neck Surgery Foundation here.
Generally there is much to be learned about OSA and its causes, according to B. Tucker Woodson, MD, Professor and Chief of Sleep Medicine at the University of Wisconsin, who served as session moderator.
In all of sleep medicine our results in the way that our outcomes are, are really poor, he said during his introductory remarks. It’s not from lack of skill of surgeons, but rather the fact that many available therapies just aren’t perfect. Indeed, one study in the literature reported only a 50% success rate for palatal obstruction surgery.
The good news is developments in the field promise to improve and even revolutionize the approach to OSA, Dr. Woodson said.
When it comes to using continuous positive airway pressure (CPAP) in patients, data on its effectiveness are sometimes misleading. CPAP is effective only when you use it. But when you apply it to a large cohort and you include the people who aren’t using it but who are supposed to use it, then it’s not nearly so effective, he said.
Proper Evaluation Is Key
Panelists addressed the best way to evaluate patients with OSA, and agreed that the history and how patients report they feel is key. The actual exam is brief, but includes height, weight, and body mass index (BMI). Also determining if there are skeletal malformations, doing a nasal exam, and asking about dental extractions-which can affect the relative size of the mandible and maxilla-should all be done.
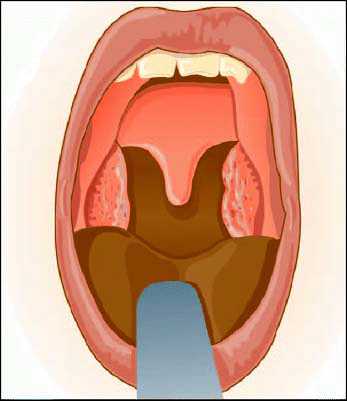
Probably the most important part of my exam is to have patients open their mouth. I do a Friedman classification, said Samuel Mickelson, MD, from Advanced Ear, Nose & Throat Associates, in Atlanta. But counting the teeth and looking for premolars and wisdom teeth tells a lot. In my own practice, between 15 and 20 percent of patients referred to me have micrognathia, and typically have four missing premolar teeth that were extracted at about age 13, he said. Pharyngeal mirror exams are done, and a fiberoptic exam is performed with the patient in a supine position.
Children with apnea who have teeth removed because of crowding might eventually need some expansion procedures, Dr. Woodson said.
The fiberoptic exam is not always needed if a patient is a surgical candidate, depending on the surgery, said Edward Weaver, MD, Associate Professor of Otolaryngology at the University of Washington. A significant portion of my practice is correcting the nasal airway to facilitate CPAP. I don’t do any fiberoptic exam on [these patients], he said.
Since so much attention is rightfully paid to the palate and tongue base, the nose is often an underappreciated part of the exam in potential sleep apnea surgical patients, said Tod Huntley, MD, from Head and Neck Surgery Associates in Indianapolis. In fact, the most common surgical procedures that most of us do for such patient is on the nose, particularly to improve CPAP tolerance and compliance, he said.
As for the nasal exam, the nasal valve is key to look at, since it can be where much of the resistance occurs, said Dr. Woodson. Problems might occur in one part or several.
Indeed, patients may have multiple abnormalities in the nose, but I don’t necessarily correct them all. I do it on as ‘as needed’ basis, said Dr. Weaver. A patient may have a narrow pyriform aperture that doesn’t bother him or her, for example, but can be worth repairing to help the patient’s apnea. On the other hand, I’ll treat a normal-looking turbinate if I think that will buy me room to facilitate CPAP, he said.
Dr. Mickelson stated he finds it worth being aggressive in treating the nose and that some of his patients aren’t even aware their nasal obstruction is problematic.
Dr. Huntley concurred, and said he is increasingly aggressive about treating the external nasal valves surgically for such patients. Yet we are all aware that numerous studies have shown that nasal surgery alone is rarely sufficient to control OSA. But appropriate nasal surgery is an important adjunct for complete surgical treatment of such patients, he said.
When Should Surgery Be Done?
When it comes to large tonsils, panelists were united in saying they’re certainly worth removing.
When you have big tonsils it tends to hold the palate forward. When you remove them you can see the palate settle back. You don’t appreciate that in your office exam because the scope is obscured by the tonsil, said Dr. Weaver.
At the same time, how much surgery is performed on the palate in the young, thin, otherwise normal adult with big tonsils depends on the severity of the apnea, he added. Big tonsils can lower the pressure in CPAP.
Some patients with moderate or severe apnea should undergo uvulopalatopharyngoplasty (UPPP) along with the tonsillectomy, though mild disease could benefit from tonsillectomy alone, panellists said.
At the same time there is some risk that UPPP can lead to mouth leak in CPAP, especially at higher pressures, Dr. Mickelson said. Yet patients undergoing this are intolerant of CPAP in the first place. Realistically the goal of therapy is to improve patient survival. If they are not getting symptomatic relief from CPAP, then the only other alternative may be surgical. Sometimes the surgery is nasal alone, and not palatal.
Much of this depends on the goals of surgery, said Dr. Huntley. Usually my goal is to completely take care of OSA, to shoot for improvement in the sleep study parameters to the level obtained by CPAP. Sometimes this can be attained only with extensive stage surgery, which is sometimes not possible with some patients, or is more than what a patient will tolerate.
Dr. Weaver concurred, stating there is benefit if the surgery did not eliminate the OSA but allowed for more CPAP compliance, or resulted in lower, more comfortable pressures. The goals of surgery should be carefully discussed with patients preoperatively.
Determining the area of obstruction is far from an exact science, said Dr. Mickelson. But UPPP outcomes can be improved if it’s known whether the obstruction in a patient is in the palatal opening, palatal-tongue, or tongue only-all are worth testing for.
Panelists agreed that if multilevel surgery to the nose, palate, and tongue base is being considered, it is important to decide how to stage such surgeries. Sometimes it’s smartest to perform the nasal surgery first, letting it heal and seeing whether the patient can benefit from CPAP before considering further surgery. But which surgery comes first depends on patient characteristics and whether the goal is to help CPAP or do an airway correction.
Then there’s risk. Published data show that the more levels of surgery of the airway operated on at one setting, the higher the complication rate. Decisions as to how much to do at one setting must be made on a case-by-case basis.
You have to use your own critical judgement. You can defend either approach, but keep in mind why you are doing it, Dr. Weaver said.
There is also evidence suggesting that UPPP makes CPAP worse in isolated incidences, and this must be communicated to the patient preoperatively.
Another related issue is the anesthesia. There are some noticeable advantages if patients are put under only a light sedation so they don’t require intubation, Dr. Woodson said. However, the preference by anesthesiologists for doing this can vary between centers.
Panelists addressed different approaches to surgery in patients with narrow or slit nostrils. Options for approaches include stabilizing the nasal valve with sutures via intraorbital or transconjunctival incisions, using a microdebrider to resect bone in the area, resecting the turbinates at the bone, or approaching the pyriform aperture sublabially.
Tailor UPPP to Patient’s Anatomy
When performing UPPP, the technique varies according to what’s appropriate for an individual patient’s anatomy, said Dr. Woodson. But panelists agreed that whatever the approach, a goal is to leave as much of the mucosal tissue as possible. Saving as much of the uvula as possible is desirable too. In some patients where UPPP is not viable, other, newer variations on the UPPP theme, such as the Z-palatoplasty, transpalatal advancement pharyngoplasty, or expansion pharyngoplasty, should be considered.
Surgeons should not limit themselves to one approach to the palate. When there are multiple such choices available, there is no one best choice for all patients, said Dr. Huntley. Panelists said their choice of palatal surgery varies from case to case, and that the patient’s presenting anatomy should be the guide.
In cases in which the uvula is not salvageable, a traditional UPPP with little or no resection of the soft palate might be the way to go. But stenosis can occur in this type of patient, presenting a whole other challenge.
Treatment of palatal and nasopharyngeal stenosis from tonsillectomy and UPPP surgery was also addressed. Panelists concurred that cases with stenosis are difficult, and reported varying success in using Z-plasty and other techniques. However, success is not always guaranteed and some degree of restenosis often is seen.
Again, saving as much mucosa as possible may help, Dr. Woodson said. On another note, Dr. Weaver cautioned against using lasers because it can make the problem worse.
Contact the Editor
ENToday welcomes your feedback about our publication! Contact us using the information below:
ENToday@wolterskluwer.com
©2006 The Triological Society


Leave a Reply