Other complications reported included the following:
Explore This Issue
August 2016- Parotidectomy wound dehiscence occurred in six cases (6%); all of these patients responded to conservative management.
- Fat transfer graft debulking was required in three patients with persistent overcorrection beyond six months postoperatively. According to Dr. Gourin, one patient lost a great deal of weight, and two patients did not have the absorption rate originally predicted. No patients demonstrated undercorrection or further FAT resorption beyond six months.
- There were no significant differences between the FAT and control groups with respect to postoperative drain output, duration of drainage, and facial nerve function.
- Although Frey’s syndrome can also occur, no patients in this study reported the condition or required Botox injections for it.
Contraindications
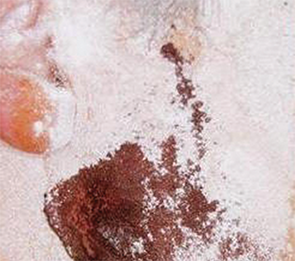
Gustatory sweating during starch-iodine test following parotidectomy.
U.S. National Library of Medicine
Dr. Gourin noted that, based on her experience since her last study on the FAT graft technique in 2008, she has found some contraindications for its use (Laryngoscope. 2008;118:1186-1190). “If you’re excising skin along with the parotid gland, then the closure is under increased tension and the FAT graft will further increase that tension. In that case, I wouldn’t consider doing one.”
Although the FAT procedure is a technically simple reconstructive option when performing parotidectomy, it isn’t as commonly used as SMC flaps. “Only perhaps half of parotid surgeons perform it, and I think its use depends to some extent on the age of the surgeon and where he or she trained,” said Dr. Gourin. “It wasn’t something I learned to do in my training; many of us just weren’t exposed to techniques for parotid defect reconstruction.
“It also depends on whether you view a parotid defect as a cosmetic problem and how much you discuss it pre-surgery with patients,” she added. “Many patients don’t ask about reconstruction because they don’t expect a defect. I offer it during consultation because after a parotidectomy and the shock of the tumor wears off, other concerns like appearance often come to the front. It isn’t vanity—it’s returning to the state they were in before the operation. I’d love to see this technique in greater use. If I ever had a parotid tumor, I would want this done.”
Amy E. Hamaker is a freelance medical writer based in California.
Key Points
- There are a number of surgical techniques for reconstructing this parotidectomy defect, including bipedicled sternocleidomastoid muscle flaps, AlloDerm biomaterial, free tissue transfer, and free abdominal fat transfer.
- Autologous fat grafts have long been used in the reconstruction of facial defects, and the advantages of utilizing fat include its abundant availability, biocompatibility, and ease of harvest.
- The main criticism of fat grafting has been reabsorption and longevity of the material.
Preventing Frey’s Syndrome
Frey’s syndrome, or gustatory sweating, is a known complication of parotid gland surgery. Placing a barrier between the overlying skin flap and the parotid bed during repair can often prevent the syndrome. A recent study published in The Laryngoscope examined how effective FAT grafts are for preventing Frey’s syndrome (Laryngoscope. 2016;126:815-819).