Although eustachian tuboplasty is in its infancy and specific criteria and indications for its use have not yet been established, researchers hope that it might provide a viable alternative to using pressure equalization tubes or tympanostomy for chronic eustachian tube dysfunction.
Eustachian tube surgery is also being offered to patients with patulous disease (see sidebar).
Chronic Eustachian Tube Obstruction
Eustachian tuboplasty is very much in its infancy, and whether the procedure is effective over time for chronic eustachian tube obstruction remains to be seen, said Ralph Metson, MD, a rhinologist and Clinical Professor of Otology and Laryngology at Harvard Medical School in Boston.
We are hoping that as we gather more and more evidence, eustachian tuboplasty will prove to be a long-term solution to chronic ear disease, said Elias Michaelides, MD, Assistant Professor of Surgery- Otolaryngology at the Yale School of Medicine in New Haven, CT. However, the outcomes of the procedure for chronic eustachian tube obstruction might take years for researchers to observe, he noted.
 Just as with surgery for chronic sinusitis, you’ve got to treat underlying problems, such as allergies.
Just as with surgery for chronic sinusitis, you’ve got to treat underlying problems, such as allergies.
-Dennis S. Poe, MD
Eustachian tube dysfunction is a relatively common problem, noted Dr. Metson. Many otolaryngologists have patients who say their ears are blocked but show no severe pathology on examination, which often leads to a diagnosis of intermittent eustachian tube obstruction.
This condition can wear down the eardrum, causing scarring or rupture. This in turn, may cause patients to experience hearing loss or cholesteatoma, said Dr. Michaelides.
Standard of Care
There aren’t a lot of good treatments for these patients, said Dr. Metson, adding that tympanostomy remains the gold standard for treating eustachian tube obstruction.
Clinical guidelines from the American Academy of Pediatrics, American Academy of Family Physicians, and American Academy of Otolaryngology-Head and Neck Surgery state that in children with otitis media with effusion who are candidates for surgery, tympanostomy tube insertion is the preferred initial procedure.
Adults with chronic or recurrent otitis media with effusion or tympanic membrane atelectasis are also candidates for tympanostomy tube insertion, said Dennis S. Poe, MD, Associate Professor of Otology and Laryngology at Harvard Medical School and Children’s Hospital in Boston.
Although they are the gold standard for treating eustachian tube obstruction, pressure equalization tubes can damage the eardrum, may cause infection, and can come out with time, noted Dr. Michaelides. They also prevent patients from swimming, he said.
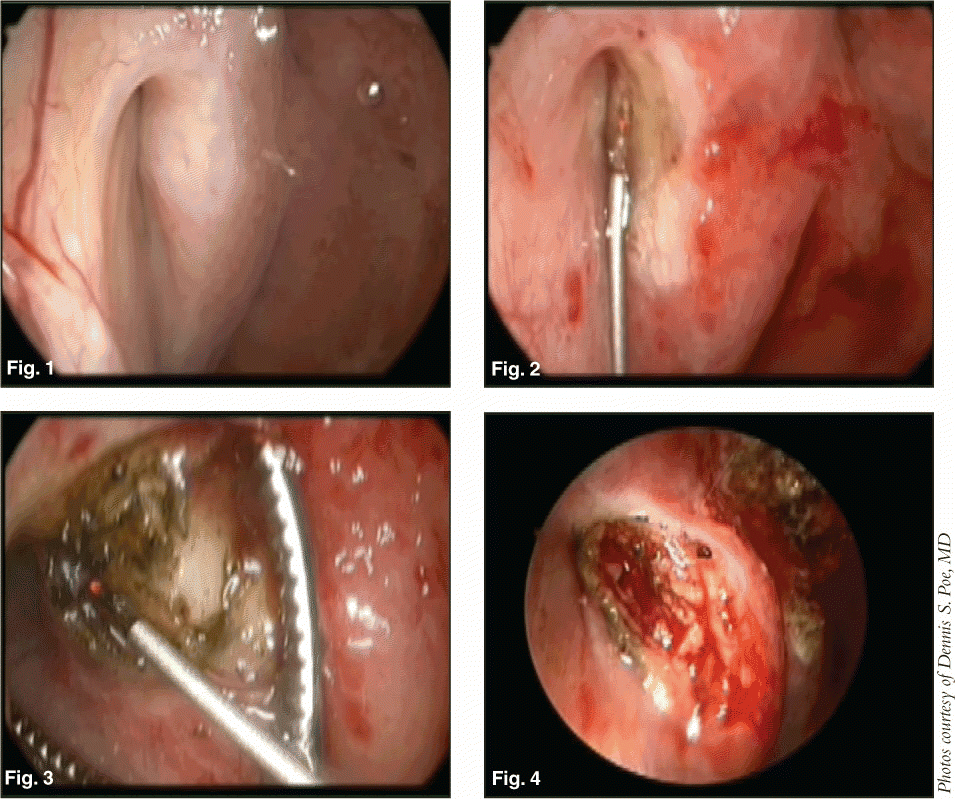
Eustachian Tuboplasty
Although it is too early to tell with certainty, researchers are hoping eustachian tuboplasty will reduce the need for tympanostomy, said Dr. Michaelides.
Eustachian tuboplasty may be used in patients with chronic eustachian tube dysfunction with tympanic membrane atelectasis or middle ear effusion and who have undergone tympanostomy only to have grommets fall out on multiple occasions while symptoms persist, said Dr. Poe.
The procedure is also used in people who experience recurrent episodes of ear discomfort with changes in altitude-for example, those that can occur on an airplane flight or while scuba diving. Eustachian tuboplasty is not yet being performed in children, he added.
Although Dr. Michaelides recommends this type of surgery to patients who are frustrated with chronic eustachian tube dysfunction that has required multiple sets of tubes or ear surgeries, he tells patients that he cannot guarantee long-term outcomes because we do not have long-term results, he said.
As a rhinologist, Dr. Metson generally offers the procedure to patients with sinusitis who are planning on having sinus surgery and have had a tympanogram that shows eustachian tube dysfunction.
The Procedure
Eustachian tuboplasty is a nasal or transoral endoscopic outpatient procedure requiring general anesthesia. To date, it has been used only in adults, said Dr. Poe. A laser or microdebrider is used to strip away hypertrophic mucosa and cartilage on the posterior eustachian tube cushion and into an area called the valve to clear obstruction.
According to a recent paper describing microdebridement in 20 patients (Otolaryngol Head Neck Surg 2007;136:422-7), Dr. Poe and Dr. Metson describe the valve as a 0.5-cm-long region where mucosal surfaces from the anterior and posterior cushions are seen to appose during tubal closure and dilate to the open position with normal tubal function.
During surgery, physicians take special care to steer clear of injury to the mucosa on the anterior cushion to avoid postoperative scarring and stenosis of the eustachian tube orifice.
According to the paper, prior surgical attempts to treat the condition focused on the enlargement of the bony eustachian tube isthmus, but drilling techniques and stents failed to restore eustachian tube function. Moreover, concerns about injury to adjacent structures, such as the carotid artery, caused surgeons to abandon this approach, wrote the authors.
During eustachian tuboplasty, whether surgeons remove both mucosa and cartilage depends on how aggressive they want to be, said Dr. Metson, who removes hypertrophic mucosa but generally does not remove cartilage unless the case of eustachian tube obstruction is severe.
As a rhinologist, Dr. Metson performs the procedure entirely through the nose, using a microdebrider in conjunction with sinus surgery. Many of his patients have eustachian tube obstruction in association with chronic sinus disease, he explained. Patients with sinusitis, for example, experience postnasal drip that flows over the eustachian tube orifices, leading to blockage.
 We are hoping that as we gather more and more evidence, eustachian tuboplasty will prove to be a long-term solution to chronic ear disease.
We are hoping that as we gather more and more evidence, eustachian tuboplasty will prove to be a long-term solution to chronic ear disease.
-Elias Michaelides, MD
Dr. Metson noted that eustachian tube obstruction in patients with sinusitis resolves after the combined procedure. I can never be sure if the blockage goes away because of the sinus surgery or eustachian tube surgery, or both, he said.
Patients who undergo eustachian tuboplasty generally experience very few significant complications, said Dr. Poe, adding that he and his colleagues have treated about 40 individuals with the procedure. However, inflammation at the surgical site that is asymptomatic may occur, he noted.
Overall, the eustachian tuboplasty is low-risk, said Dr. Michaelides. Patients experience very little pain postsurgery, he said, adding that he recommends that patients use nasal rinses or saline sprays to assist in the healing process. Patients can return to normal to activities the following day.
Treating Inflammation
Before considering eustachian tube surgery, physicians should treat patients for any nasal allergies or reflux symptoms that may be contributing to chronic disease and the swelling of the eustachian tube mucosa, said Dr. Michaelides.
Just as with surgery for chronic sinusitis, you’ve got to treat underlying problems, such as allergies, noted Dr. Poe.
Controlling the underlying cause of inflammation can help to increase the success rate of Eustachian tuboplasty for chronic eustachian tube dysfunction, which is only about 50% to 55%, said Dr. Poe. Patient preoperative and postoperative compliance with treatment for inflammation is also important, he added.
Recent Data
To date, research has shown that eustachian tuboplasty for the treatment of eustachian tube dysfunction is safe in conjunction with sinus surgery.
In the prospective study of 20 patients mentioned above, for instance, researchers evaluated microdebrider eustachian tuboplasty via a solely transnasal approach in patients with eustachian tube dysfunction. All patients also had sinonasal disease and received endoscopic sinus surgery at the same time as the eustachian tuboplasty.
After a mean follow-up of 13 months, 70% of patients reported improvements in symptoms of ear blockage. Mean pure tone average improved by 6 decibels, and abnormal tympanogram improved in 65%. Patients did not experience any surgical complications.
Although there has not been a direct head-to-head comparison, Dr. Metson noted that laser surgery appears to be just as effective as microdebridement for eustachian tuboplasty.
For example, in a prospective surgical trial (Otol Neurotol 2004;25:1-8), Dr. Poe and his colleague, Oskar Kujawski, MD, of the Eustachian Tube Institute in Geneva, Switzerland, evaluated outcomes in 108 eustachian tubes in 56 patients who underwent laser eustachian tuboplasty under general anesthesia through a combined endoscopic nasal and transoral approach. Patients had intractable eustachian tube dysfunction with either middle ear effusion or tympanic membrane atelectasis.
Dr. Kujawski used laser vaporization of mucosa and cartilage from the luminal posterior wall until he achieved adequate dilation. He also performed a laser myringotomy to provide middle ear aeration while packing the eustachian tube.
About 65% of ears had normal middle ear aeration at three years or longer. Patients did not experience any intraoperative complications. Postoperative complications included minimal peritubal synechia in about 8% of tubes and epistaxis in nearly 1% of tubes. About 6.5% of ears did not respond to treatment and required tympanostomy.
Another small prospective study (Laryngoscope 2003;113:583-91), of which Dr. Poe, Dr. Metson, and Dr. Kujawski were authors, found that laser eustachian tuboplasty was safe and efficacious in the treatment of intractable eustachian tube dysfunction.
The researchers studied 10 patients with chronic intractable otitis media with effusion, who were treated with unilateral laser eustachian tuboplasty. These patients had already undergone repeated tympanostomy procedures, which had failed.
The surgeons combined transnasal and transoral approaches and used a laser to vaporize mucosa and cartilage on the posterior wall of the tubal lumen. Patients received general anesthesia, and surgery was on a outpatient basis.
After six months, seven of the 10 patients were free of effusion. There were no intraoperative complications; postoperative complications were minimal peritubal adhesions and one intranasal synechia.
 We’re trying to be careful and to work scientifically with academically rigorous publications, and we don’t want to make any false claims.
We’re trying to be careful and to work scientifically with academically rigorous publications, and we don’t want to make any false claims.
-Ralph Metson, MD
Future Research
Researchers agree that further studies are needed to determine the long-term outcomes of eustachian tuboplasty for chronic obstruction. We think that the procedure has promise, although long-term studies are needed, said Dr. Poe.
It may be years before any problems recur to indicate that the eustachian tube surgery was not effective, explained Dr. Michaelides.
Because the surgery is still new, we’re trying to be careful and to work scientifically with academically rigorous publications, and we don’t want to make any false claims, said Dr. Metson.
Investigators also need to explore whether the eustachian tuboplasty is more effective in conjunction with sinus surgery, noted Dr. Metson.
Additionally, Dr. Poe and his colleagues are looking at the origin of eustachian tube inflammation in children and adults, said Dr. Poe. We’re looking for eustachian tube and middle ear biofilms, inflammation markers, proteins, and gene expressions, he said. They are also researching whether the procedure should be used in children.
In addition to conducting ongoing basic science research, investigators want to improve the efficacy of the procedure and possibly expand its indications, said Dr. Poe.
In Practice
While research is ongoing, eustachian tuboplasty remains a simple technique that general otolaryngologists can perform, noted Dr. Poe. However, the procedure should be applied cautiously in clinical practice, and practitioners should preferably take a course to learn the surgery and the anatomy involved, he said.
The experience of general otolaryngologists performing the surgery in their patients will determine whether the procedure becomes widely accepted and is effective in the long term, added Dr. Metson. They are the ones who will end up deciding the value of eustachian tube surgery and not the academics, he said.
Eustachian tuboplasty is still in the early stages of being implemented in patients, but it continues to show promise, concluded Dr. Poe.
Patulous Eustachian Disease
Eustachian tuboplasty may also be used to treat patulous disease, a condition in which the eustachian tube channel opens abnormally, said Dr. Michaelides.
The patulous eustachian tube is due to a defect in the normally convex anterior-lateral wall that can be due to loss of volume with the mucosa, submucosa, Ostmann’s fat pad, cartilage, or tensor veli palatini muscle, explained Dr. Poe.
The main complaint associated with the condition is autophony, said Dr. Michaelides. Other symptoms may include subtle hearing loss and respiratory tinnitus.
Traditional treatments for patulous disease include medical therapies such as nasal sprays to induce irritation of the eustachian tube mucus membranes, causing them to become more bulky and narrowing the passageway. Weight gain in patients who have recently lost weight and developed patulous symptoms may also help, said Dr. Michaelides, who offers eustachian tuboplasty to patients in whom these therapies aren’t effective.
For patulous disease, surgeons augment the eustachian tubal walls, narrowing the passageway, using autograft cartilage, he said.
The lumen may also be narrowed with diathermy or silver nitrate cautery, according to the Eustachian Tube Institute (www.eustachian-tube.net/SOLUTIONS.html ). Extrinsic compression by paraffin, Teflon, gelatin, sponge or collagen injection are other options. The surgery usually requires general anesthesia and is an outpatient procedure.
So far, patients have not had any significant complications from undergoing eustachian tuboplasty for patulous disease, and they generally experience little to no pain, said Dr. Michalides. As with eustachian tuboplasty for chronic obstruction, he recommends that patients use nasal rinses or saline sprays to assist in the healing process.
If the surgery is successful, autophony will be eliminated immediately, said Dr. Michaelides, adding that unlike chronic obstructive disease, researchers do not have to wait for long-term outcomes to determine whether the treatment is effective. The outcomes of surgery for patulous symptoms are much more clear for patients than for those with chronic eustachian tube obstruction, he explained.
Research data on treating patulous eustachian tubes are in the process of being collected, noted Dr. Michaelides.
©2009 The Triological Society
Leave a Reply