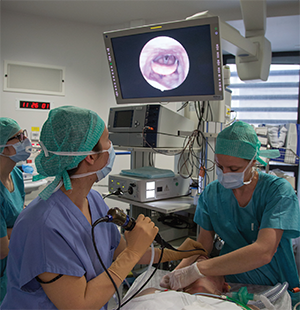
Patient undergoing sleep endoscopy.
© Voisin / Phanie / Science Source.com
Deciding how to evaluate and treat hypopharyngeal obstructive sleep apnea (OSA) is often not a straightforward proposition, but many options exist for getting the best results for patients, according to a panel of experts who convened at the annual meeting of the American Academy of Otolaryngology-Head and Neck Surgery.
Explore This Issue
November 2016The wide-ranging panel covered the need for better ways to identify airway obstruction sites, radiofrequency tongue reduction, transoral robotic surgery, a system for grading lingual tonsil hypertrophy, endoscopic coblator open tongue base resection, epiglottic collapse and laryngomalacia, and the role of skeletal surgery.
Identifying the Obstruction Site
Eric Kezirian, MD, MPH, professor of sleep medicine in the department of otolaryngology-head and neck surgery at the University of Southern California in Los Angeles, stressed the importance of identifying the site or sites of obstruction. Several studies have cited the need for better ways to do this (Cochrane Database Syst Rev. 2000;(2):CD001004; 2005;(4):CD001004).
“Although sleep apnea is not entirely related to anatomy, when it comes to surgery, we are treating the anatomy. We want to make the most accurate determination of the anatomical issues and treat patients individually,” he said.
OSA severity as a sign of site obstruction—the idea that mild-to-moderate OSA is likely a result of collapse at the palate level and that moderate-to-severe sleep apnea likely includes some component of hypopharyngeal collapse—is inaccurate and is not supported by the evidence. Also, the Friedman system, which involves considering relative tongue size, tonsil size, and body mass index, is not sufficient for guiding surgical decisions by itself in the majority of patients, he added.
Drug-induced sleep endoscopy (DISE), designed to visualize the pattern of obstruction by reproducing the patterns seen on a sleep study, is becoming more commonly used; however, it is not a simple procedure and does require some time in the operating room or procedure suite. Dr. Kezirian is leading an international collaborative study to better tease out how DISE findings are associated with outcomes of sleep apnea surgery.
By improving the assessment, he said, “we may be able to develop targeted, more effective treatment of sleep apnea with surgery, and probably oral appliances as well.
Radiofrequency Tongue Reduction
Edward Weaver, MD, MPH, chief of sleep surgery at the University of Washington and co-director of the UW Medicine Sleep Center in Seattle, said radiofrequency surgery under local anesthesia over a series of sessions to reduce tongue size can be a good, minimally invasive option for some patients. But, it’s important for patients to have realistic expectations, and those with severe problems, such as a very high apnea-hypopnea index (AHI), a huge tongue, and a floppy palate—wouldn’t be good candidates.