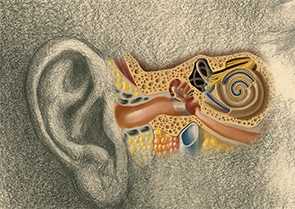
Image Credit: Spencer Sutton / Science Source
Konstantina Stankovic, MD, PhD, associate professor of otology and laryngology at Harvard Medical School and associate surgeon at the Massachusetts Eye and Ear Infirmary, finds it astounding that we don’t know more about what happens inside the inner ear.
Explore This Issue
December 2015Globally, hearing loss is the most common sensory loss, with 600 million people affected worldwide. And it is the most common congenital anomaly, with one in 500 newborns affected. Most sensorineural hearing loss starts in the inner ear.
“Given the magnitude of the problem, it’s mind-boggling that today, in the 21st century, we cannot biopsy the inner ear and we cannot see cells inside it to establish diagnosis,” said Dr. Stankovic, delivering the Howard P. House, MD Memorial Lecture for Advances in Otology during the Annual Meeting of the American Academy of Otolaryngology-Head and Neck Surgery, held in September in Dallas. She and colleagues at her laboratory are working to demonstrate what is possible when neuroscience and biotechnology are used imaginatively to tackle real-world clinical problems.
Advances from her lab include a new use of optical tools to better assess the condition of the inner ear to help with diagnosis and treatment, development of a completely implantable cochlear implant, the use of electric potential in the inner ear to power very small devices, a deeper understanding of vestibular schwannoma’s effects on hearing loss and potential treatments, and an understanding of the role of osteoprotegerin in the inner ear, which may have implications for hearing loss therapy.
Despite the inner ear being located deep in the base of the skull and very tiny, Dr. Stankovic and her colleagues have made it a mission to overcome this and other hurdles in order to expand research and advances in the inner ear.
New Imaging of the Inner Ear
Some research on mice using optical imaging based on laser light has found damage to hair cells after exposure to a sound at the volume of a snowblower. Dr. Stankovic and her colleagues are developing an endoscope that can be used to establish what is happening in the inner ear in any given patient.
“This strongly motivates the need to develop tools that would allow us to see inside the ear and establish cellular-level diagnosis,” she said. “The workhorse of hearing testing today, an audiogram, is notoriously insensitive.” She envisions a tool that could be wheeled around and used during outpatient procedures and would “literally take a few minutes” to image through the inner ear canal to give a picture of what’s going on. “This could be important not only to establish diagnosis but to guide therapy.”
Fully Implantable Cochlear Implant
Dr. Stankovic has also developed a prototype for a fully implantable cochlear implant, which would help overcome limitations of current versions that have external and internal components. With the prototype, the pattern of speech input matched the pattern of the speech output.
The device would need a power source, and researchers have found that it’s possible to draw a small amount of electricity from a source in the inner ear, the endocochlear potential. In a proof-of-principle study using a chip that can fit on the tip of your index finger, researchers powered a radio transmitter entirely with power from a guinea pig’s inner ear, although the chip was located outside the body and connected with electrodes. This was done without any damage to hearing. “This is the first demonstration that you can use an electrochemical gradient from the body to power an electronic device,” Dr. Stankovic said.
She emphasized that this involves only nanowatts of power, and cochlear implants use tens of milliwatts. But the location of the inner ear, which is millimeters from the temporal bone and the facial nerve, could be an important advantage, she said. “We envision that down the line this energy from the inner ear may be used to power various sensors in the inner ear and its vicinity.”
New Treatments for Vestibular Schwannomas
Through a series of discoveries beginning with an examination of all the genes that have ever been reported to be differentially regulated in vestibular schwannomas, Dr. Stankovic’s laboratory could be getting closer to addressing an unmet medical need to develop well-tolerated pharmacologic therapies for these tumors, she said. The genes have been pointing researchers in the direction of inflammation, and the researchers have submitted a grant proposal that suggests research on whether aspirin has a role in their treatment.
Down another avenue, the researchers, noting that tumor compression itself can’t be the cause for hearing loss because tumor size does not correlate with hearing loss, have turned to tumor secretions instead. They now believe that tumor necrosis factor (TNF)-alpha could be a molecule that is toxic to the inner ear and is being secreted by the tumors. “Is it possible that we could use TNF-alpha inhibitors such as the ones that are already in clinical practice … to try to prevent hearing loss in these patients?” Dr. Stankovic asked.
A Possible Role for Bisphosphonates
When researchers performed a mass spectrometry analysis of the human perilymph to study the fluids of the inner ear, doubling what is known about the protein content of the perilymph, they were intrigued by the large amount of osteoprotegerin, a protector of bone remodeling. They now believe that the bisphosphonate zoledronate, which can reverse the effects of osteoprotegerin deficiency, could have a neuroregenerative role in the inner ear, and have received a grant from the Department of Defense to study this possibility.
Dr. Stankovic said that all of these discoveries are evidence of what can happen when advanced science is brought to bear on real human medical problems. “Our approach overall is that we start with problems in clinical medicine—clinical otology, neurotology,” she added, “and then we use tools of biotechnology and neuroscience to ultimately help patients.”
Thomas Collins is a freelance medical writer based in Florida.
Take-Home Points
- Dr. Stankovic and her colleagues are developing an endoscope that can be used to establish what is happening in the inner ear.
- She and her team have developed a prototype for a fully implantable cochlear implant.
- The researchers could be getting closer to addressing an unmet medical need to develop well-tolerated pharmacologic therapies for vestibular schwannomas.