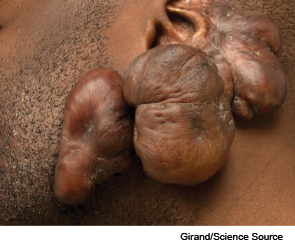
Keloids are incredibly common in some patient populations. These abnormal scars, which grow well beyond the border of the original injury site, are typically unsightly, inconvenient, and often uncomfortable. Keloids cause pain, pruritis, and even hyperesthesia, as well as social discomfort and embarrassment.
Until recently, very little was known about the etiology of keloids, and even less was known about how to effectively treat and manage these growths. Surgical excision is frequently inadequate, because many, if not most, keloids recur after excision. Other treatment measures, including corticosteroid injection and the use of pressure dressings, were based on medical intuition and anecdotal evidence more than on scientific research.
Not surprisingly, keloids remain a challenge for patients and practitioners alike. Fortunately, new research is beginning to reveal more about the etiology of keloids. Innovative treatments continue to hit the market, with more anticipated in the future. Experts predict that biologic therapies may eventually be used to treat—and even prevent—keloids. There’s even hope that an increasing understanding of keloid formation and treatment will lead to innovations within the field of plastic surgery.
“When you look at facial plastics, our nemesis is scar formation,” said Lamont R. Jones, MD, vice chair of the department of otolaryngology–head and neck surgery at Henry Ford Hospital in Detroit. “What is exciting about studying keloids is that if we understand what’s going on in keloids, we can exploit that knowledge for other uses in facial plastics.”
Epigenetic Link
Because keloids are most commonly seen in people of African, Hispanic, and Asian descent, researchers have long suspected a genetic component to keloid formation. The observation that more than half of all patients with keloids report a family history of keloid scarring has strengthened that suspicion (Mol Med. 2011;17:113-125).
By 2008, researchers had identified at least one autosomal dominant inheritance pattern of keloids and some genes (most notably HLA-DRB1*15 and DQB1*0503) associated with an increased risk of keloid scarring (Mol Med. 2011;17:113-125). But keloids have also been associated with immune response and blood type, leading researchers to believe that keloid formation is much more complex than the presence, absence, or mutation of any one gene.
“Most disease conditions are complex. A lot of times, there is not just one gene that’s involved but a pathway. There may be multiple genes that come together to help produce whatever the end result may be,” Dr. Jones said. “So, identifying a gene and pathways may key you into the bigger picture of what’s going on with that process, and identifying that gives you the opportunity to look at other relationships, which may be more important than a particular gene alone.”
Dr. Jones and colleagues recently used advanced genetic sequencing technology to profile the genomes of six keloids and six normal skin samples; that profiling revealed 152 keloid specific genes. Those genes were uploaded into Ingenuity Pathway Analysis software, which led to the discovery of 10 genes that are part of biological pathways known to be important to the process of keloid development. Dr. Jones presented his findings at the International Symposium of Facial Plastic Surgery in May 2014.
“Some of the genes we identified are unique; they haven’t yet been reported in keloids,” Dr. Jones said. “This research allows us to look at the genes identified in this study in a different light and from the standpoint of their biological significance. These genes are part of pathways, and we can study them at different points along the pathways to identify opportunities to intervene therapeutically.”
 What is exciting about studying keloids is that if we understand what’s going on in keloids, we can exploit that knowledge for other uses in facial plastics.
What is exciting about studying keloids is that if we understand what’s going on in keloids, we can exploit that knowledge for other uses in facial plastics.—Lamont R. Jones, MD
Current Treatment
Fortunately, many of the most common facial plastic surgery procedures are unlikely to result in keloid formation. “The places that keloids are most likely to occur are the earlobes, the shoulders, the sternum, the preauricular areas, and the neck. Within the head and neck region, the earlobes and neck are the two most common areas of keloid scarring,” said Anthony Brissett, MD, associate professor of otolaryngology–head and neck surgery and director of the Baylor Facial Plastic Surgery Center in Houston, Texas.
The middle of the face is unlikely to develop keloids, so facial plastic surgeons can feel comfortable performing rhinoplasty and blepharoplasty, said Dr. Brissett. Procedures such as otoplasty and rhytidectomy are more likely to result in keloids in at-risk patients, due to the locations of incisions.
Of course, many patients seek assistance for keloids that developed as a result of previous procedures, such as ear piercing. The most common treatments for keloids include silicone gel sheeting, intralesional corticosteroid injections, laser and light-based therapy, cryotherapy (both topical and intralesional), radiotherapy, fluorouracil (5-FU), interferon, bleomycin, imiquimod 5% cream, botulinum toxin A, and surgical excision, but none of these treatments have been found to be universally useful or effective (Burns [published online ahead of print April 22, 2014]. doi:10.1016/j.burns.2014.02.011). As a result, physicians often combine treatments for the most effective results.
According to a 2014 review, combining intralesional corticosteroid injection, a common first-line treatment, with surgery, pulsed-dye laser treatment, 5-flurouracil, and silicone gel sheeting may be a more effective first-line treatment than corticosteroid injection alone, which carries a high risk of recurrence. Keloids that don’t respond to that regimen can be treated with cryotherapy or irradiation via brachytherapy and electron beam radiation (Burns [published online ahead of print April 22, 2014]. doi:10.1016/j.burns.2014.02.011).
Recent Advances
A 2012 study of three patients suggests combining silicone gel sheeting with negative pressure. The small study examined the use of an all-in-one negative pressure/silicone dressing device; patients used the device for one month, and two patients demonstrated an improvement in keloid appearance, itching, and thickness at one month, with further improvement in thickness two months after the discontinuation of treatment. The third patient, a juvenile, dropped out of the study after one week. (Int Wound J. 2013;10:340-344).
Intralesional cryotherapy is beginning to emerge as an alternative to external cryotherapy. “The problem with freezing keloids with a traditional cryogun is that you freeze the surface of the lesion and not necessarily the inside of the lesion,” said Gary Goldenberg, MD, assistant professor of dermatology and pathology at the Mount Sinai School of Medicine in New York City. A new, specially designed needle probe allows clinicians to freeze keloids from the inside out, a procedure that has been shown to be safe, well-tolerated, and efficacious (J Clin Aesthet Dermatol. 2013;6:23-26).
“This procedure works best for exophy-tic keloids,” Dr. Goldenberg said. “The lesion has to be thick enough so you can stick the probe through the keloids. If it’s really thin and flattish, it won’t work because the needle won’t get all the way through and you’ll end up freezing normal, healthy tissue.”
Larger keloids may require more than one cryotherapy session. Results vary, but most patients experience notable improvement. “Every patient does differently, but I have to tell you, from my experience, for a single treatment, it is by far the best treatment that I’ve used,” Dr. Goldenberg said.
Stem cells also show promise in the treatment of keloids. “A group in Britain looked at keloids and stem cells and found that keloids have an increased number of stem cells,” said Marc Jeschke, MD, PhD, a professor in the departments of surgery and immunology at the University of Toronto. Researchers have examined the effect of human Wharton’s jelly stem cells on keloid tissue and found that exposure inhibits keloid cell proliferation in culture (J Cell Biochem. 2014;115:826-838; Stem Cells Transl Med. 2014;3:299-307).
Dr. Jeschke is also currently investigating the utility of stem cells derived from human adipose tissue. He uses liposuction to gain adipose tissue, then isolates and harvests the stem cells, which are injected beneath a keloid scar. “The effect of those stem cells is that they dampen the inflammatory response and, in a lot of cases, cause regression of the keloids,” Dr. Jeschke said. “Effectiveness varies. We’ve had everything from fantastic results to it didn’t really work that well, and it’s hard to predict who will respond or not. But for some patients, it was incredible. The keloids were gone. They melted away.”
Will New Research Translate to Effective Treatments?
Otolaryngologists, dermatologists, and plastic surgeons are watching the advances in keloid research and treatment with interest. “I do think that the new genetic studies are going to help us understand how to prevent keloids better,” Dr. Goldenberg said. “The Holy Grail is preventing keloids as opposed to waiting for them to occur and then treating them.”
Clinicians and researchers also hope that new research will help clinicians tailor treatment. “We’re actively researching a pathway that we think may be highly predictive for those patients who may or may not respond to the most common keloids treatment, which is steroid injection plus a minor surgical excision,” Dr. Jones said. “The important thing is that if we can identify the people who are less likely to respond to this treatment, we can better determine who will benefit from other treatments.”
That insight would be most helpful, as right now there is no way, other than trial and error, for clinicians to know which treatment modality will be most effective for any particular keloid or patient. Yet it will likely be years until the current research yields actionable insights for keloid management.
“Unfortunately, although we have a better understanding of keloids in terms of the pathways involved in scarring and wound healing, we still have some difficulty in terms of translating that to medical management and improved outcomes,” Dr. Brissett said.
Unraveling the science of keloids, though, may ultimately revolutionize the field of facial plastics, because understanding keloids may provide insights into a process common to all human beings. “Part of what happens with the aging process is that we lose support tissue like collagen,” Dr. Jones said. “Keloids have an abundance of collagen and support tissue. Figuring out how to treat keloids, and why keloids do what they do, has the potential for identifying a way of combating aging as a result of the loss of collagen and structure.”
Jennifer L.W. Fink is a freelance medical writer based in Wisconsin.
Leave a Reply