Kristen B. Pytynia, MD, MPH, is Assistant Professor in the Department of Otolaryngology, Head and Neck Surgery at The University of Illinois-Chicago. E-mail: pytynia@uic.edu.
Oral screening exams are inexpensive, are easy to perform, and have the potential to reduce the annual global mortality for oral cancer by tens of thousands of people. So why isn’t screening for oral cancer as effective as screening at other sites, such as breast, colon, or prostate? Are we evaluating the wrong people, performing the screening incorrectly, or just not screening at all? What are the factors influencing our lack of success at early detection of oral cancers via screening? And with the rise in HPV-associated oropharyngeal cancers, can screening help early detection of tonsil or base-of-tongue disease?
More than 40,000 new cases of squamous cell carcinoma of the head and neck are diagnosed annually in the United States. New strategies are needed for reducing the morbidity and mortality of head and neck cancer, particularly since multiple treatment advances have not significantly changed the prognosis of oral cancer in the past three decades. Perhaps efforts to decrease oral cancer mortality should be aimed at disease prevention and improving early detection.
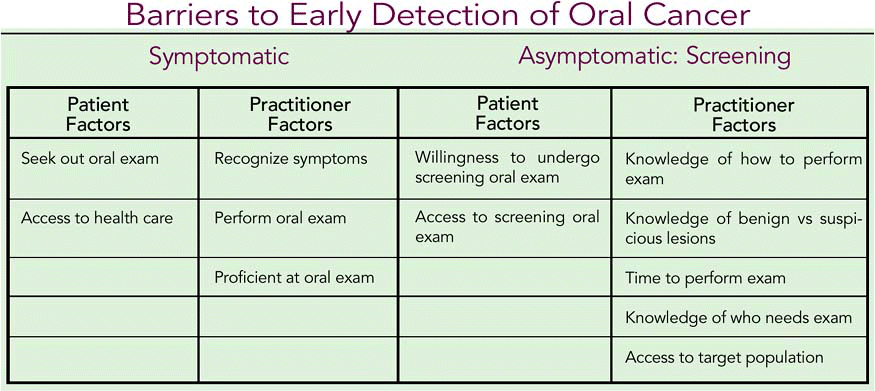
Early detection has two arms. The first arm is directed toward increasing both patient and practitioner knowledge of the signs and symptoms of head and neck cancer to allow the diagnosis to be made at an early stage. The other arm is focused on improving screening for oral cancer in asymptomatic patients. However, there are significant barriers to oral screening, the sum of which make the implementation of screening seem to be an unachievable dream (see table, next page).
The Innate Difficulty of Screening
Screening is, by definition, for asymptomatic patients. The goal of screening is to find patients with cancer prior to the development of symptoms. Therefore, in the strictest definition of screening, patients who come in complaining of the principal symptoms of head and neck cancer-such as otalgia, neck mass, hoarseness, dysphagia, odynophagia, or unintentional weight loss-should undergo a complete exam directed toward finding the origin of their symptoms, and consequently this should not be considered a screening exam.
Therein lies some of the difficulty of screening. How do we get an asymptomatic patient to have a screening? Colon, breast, and prostate screenings have been beneficial only after an enormous amount of resources was aimed at improving patient knowledge about the benefit of screening. The patients at highest risk for oral and oropharyngeal cancer are heavy smokers and drinkers. Charles LeHew, PhD, has been involved in screening more than 2000 patients for head and neck cancer through his work at the University of Illinois at Chicago. The biggest challenge is reaching those people at greatest risk, particularly men with histories of tobacco and alcohol use, he said. These are the people least likely to receive routine medical and dental care and are also the least likely to avail themselves of free screening opportunities. Many of these men simply don’t want health care unless disability drives them to it.
Oral screenings are easier to perform than prostate, colon, or even breast exams. Colonoscopies and mammograms are only performed by specialists, but the oral cavity is accessible to anyone. As 40% of head and neck cancers diagnosed in the United States are in the oral cavity, and 40% of those are on the lateral tongue, the oral cavity is a prime area for screening. Any physician, dentist, or physician extender should not only be able to perform the oral exam, but should also be able to detect the overwhelming majority of oral cavity-incident cancers. Yet up to 40% of some medical practitioners feel that they lack the skill to recognize a potentially malignant lesion. And even though a quick oral exam can take less than a minute, increasingly overstretched physicians do not feel that they have the time to perform an oral exam, especially in a health care setting that is increasingly demanding more office visits in less time with less compensation. In other words, being a thorough physician just doesn’t pay.
There has been some debate among head and neck cancer clinicians regarding the use of adjuvant tests for oral screening, such as dyes or cytological brushing specimens. Although these may be useful for the experienced examiner, they are not appropriate for the primary care provider. We need to first ensure that primary care providers and dentists are actually performing the screening and have the proper training to recognize lesions. The state of oral screening among primary care providers has not advanced enough to utilize adjuvant testing.
Components of an Effective Screening Program
What are the components of effective screening programs? First, the screening test must be easy, reliable, and cost-effective. The oral cavity exam is easy and inexpensive, but is it reliable? It is only as reliable as the strength of the training of the practitioner.
Second, intervention must be able to reduce the morbidity and mortality of the disease. Early stage disease can have as high as a 90% five-year survival with proper treatment.
Finally, the incidence of disease must be high enough that it is likely that a random sampling of the target population will identify patients with early asymptomatic (or minimally symptomatic) disease. This final criterion poses a difficulty for screening programs directed at oral and oropharyngeal cancer detection. The incidence of disease, while increasing in some populations, is not necessarily high enough to make oral and oropharyngeal cancer a common disease, at least in the United States.
Oral cavity cancer is actually the number-one cancer in India, with buccal mucosa being the most common site, likely due to the widespread use of chewing tobacco mixed with the carcinogenic betel nut. One of the few studies examining the effect of oral cancer screenings was completed recently in India by Sankaranarayanan et al. (Sankaranarayanan R et al., for the Trivandrum Oral Cancer Screening Study Group. Effect of screening on oral cancer mortality in Kerala, India: a cluster-randomised controlled trial. Lancet 2005;365:1927-33). Tobacco users in the intervention group who had undergone screening had a reduced mortality from oral cancer compared with the control group. But can we apply these findings to the United States? The incidence of oral cavity cancer in India is four to six times higher than in the United States, making a screening program in India more likely to detect a patient with a lesion. There are other factors that may have led to the success of Dr. Sankaranarayanan’s intervention. This study involved recruiting patients by going door to door. How would we get these patients to present for screening? Furthermore, the breakdown analysis found that only high-risk patients (with a history of tobacco use and drinking) should be screened. If we try to apply that in this country, we will be missing the 10% to 20% of patients with oral cavity cancer and perhaps a higher percentage of patients who have oropharyngeal cancer without a smoking or drinking history. And with the increasing prevalence of HPV-associated disease, particularly with oropharyngeal disease, this may lead to a significant number of people who are at risk but not screened due to lack of tobacco use.
The Importance of Screening
At the University of Illinois at Chicago, 76% of our patients have advanced-stage disease, well over the Surveillance, Epidemiology, and End Results (SEER) database average for all sites. Some may consider this to be university bias. Regardless, I consider this to be unacceptable. During my first few months as an attending physician, I noticed that patients were coming in with bulky disease that perhaps might have been visible earlier, and some of these patients were followed by other doctors for their comorbid conditions. In fact, the vast majority of patients with advanced stage disease have seen a doctor for some other complaint in the past year.
With this in mind, I have started a more systematic teaching of medical students about the oral examination and how to do an oral screening. I emphasize performing a complete oral exam, but the real take-home point (at least in is country) is to learn to examine the lateral tongue. The lateral tongue is the most common place for Americans to develop oral cancer, yet it is rarely examined in a general exam. I emphasize in my lecture and in clinic that adding the command, Stick out your tongue, move it to one side, move it to the other side will allow examination of the lateral tongue in less than 15 seconds and will likely result in improved early detection. Because of the increase in HPV-associated oropharyngeal cancers, I have recently started emphasizing visual inspection of the tonsils as well as palpation of the base of tongue and tonsils. I also teach self-exam to my patients who have cancer or are high risk due to smoking or drinking.
Great strides are needed in order for screening for oral cancer to be successful in the United States. On a practitioner level, we need to improve the knowledge and techniques of oral cancer screening, as well as make practitioners recognize the importance and ease of screening. In particular, we need primary care providers to participate in oral screening, and we must continue to encourage dentists to do the same. The increase in HPV-associated oropharyngeal disease should be a call to action for providers to examine the tonsils and base of tongue. Patients also need to recognize the importance of oral screening, present themselves for screening, and learn to perform a self-exam. With concerted efforts, I believe that oral screening can be a successful part of early detection, and can significantly decrease the morbidity associated with oral and oropharyngeal cancers.
©2008 The Triological Society

Leave a Reply