Kristen B. Pytynia, MD, MPH, is Assistant Professor in the Department of Otolaryngology, Head and Neck Surgery at The University of Illinois-Chicago. E-mail: pytynia@uic.edu.
Explore This Issue
February 2008Oral screening exams are inexpensive, are easy to perform, and have the potential to reduce the annual global mortality for oral cancer by tens of thousands of people. So why isn’t screening for oral cancer as effective as screening at other sites, such as breast, colon, or prostate? Are we evaluating the wrong people, performing the screening incorrectly, or just not screening at all? What are the factors influencing our lack of success at early detection of oral cancers via screening? And with the rise in HPV-associated oropharyngeal cancers, can screening help early detection of tonsil or base-of-tongue disease?
More than 40,000 new cases of squamous cell carcinoma of the head and neck are diagnosed annually in the United States. New strategies are needed for reducing the morbidity and mortality of head and neck cancer, particularly since multiple treatment advances have not significantly changed the prognosis of oral cancer in the past three decades. Perhaps efforts to decrease oral cancer mortality should be aimed at disease prevention and improving early detection.
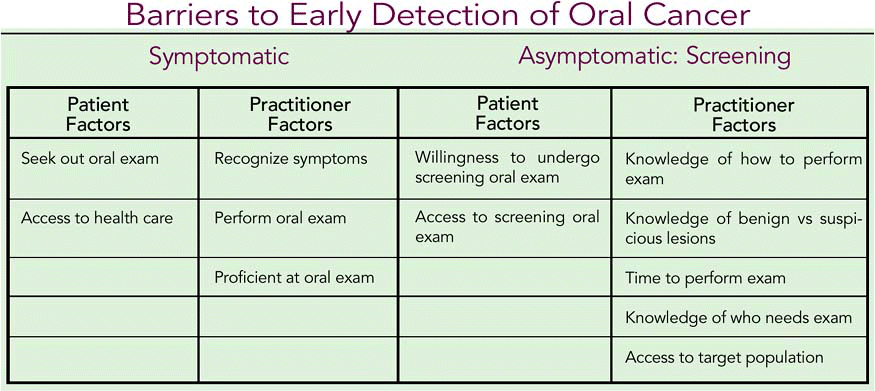
Early detection has two arms. The first arm is directed toward increasing both patient and practitioner knowledge of the signs and symptoms of head and neck cancer to allow the diagnosis to be made at an early stage. The other arm is focused on improving screening for oral cancer in asymptomatic patients. However, there are significant barriers to oral screening, the sum of which make the implementation of screening seem to be an unachievable dream (see table, next page).
The Innate Difficulty of Screening
Screening is, by definition, for asymptomatic patients. The goal of screening is to find patients with cancer prior to the development of symptoms. Therefore, in the strictest definition of screening, patients who come in complaining of the principal symptoms of head and neck cancer-such as otalgia, neck mass, hoarseness, dysphagia, odynophagia, or unintentional weight loss-should undergo a complete exam directed toward finding the origin of their symptoms, and consequently this should not be considered a screening exam.
Therein lies some of the difficulty of screening. How do we get an asymptomatic patient to have a screening? Colon, breast, and prostate screenings have been beneficial only after an enormous amount of resources was aimed at improving patient knowledge about the benefit of screening. The patients at highest risk for oral and oropharyngeal cancer are heavy smokers and drinkers. Charles LeHew, PhD, has been involved in screening more than 2000 patients for head and neck cancer through his work at the University of Illinois at Chicago. The biggest challenge is reaching those people at greatest risk, particularly men with histories of tobacco and alcohol use, he said. These are the people least likely to receive routine medical and dental care and are also the least likely to avail themselves of free screening opportunities. Many of these men simply don’t want health care unless disability drives them to it.

Leave a Reply