Patient Nonattendance

© hxdbzxy / shutterstock.com
How many patients are no-shows for their appointments at rhinology clinics? According to a review by Benjamin Hunter, MD, of Southern Illinois School of Medicine in Springfield, Ill., the answer is 8%. That’s significantly lower than studies that have shown no-show rates between 24% and 28% in adult clinics.
Explore This Issue
June 2018But little work has been done in otolaryngology to quantify patient attendance in rhinology clinics. Dr. Hunter said just a half-dozen reviews have been conducted. Four of those were outside the U.S., all of them were single-institution studies, and no adult subspecialty comparisons have been made. That’s despite the issues that no-shows cause, including workflow disruption, suboptimal resource utilization, and delays for scheduled procedures.
Dr. Hunter and colleagues used a retrospective review of two academic centers to establish the profile of patients who do not attend their appointments. Insurance status and age were among the most notable factors in nonattendance. Some 19% of Medicaid patients did not show up for appointments, compared with 5% each for patients with private insurance or Medicare. While 11% of patients aged 50 or younger did not attend appointments, the number for those older than 50 was 5%.
Future research could help determine whether interventions targeting both patient profiles could help improve attendance.
Inequality in Otolaryngology Residency Interview Invitations

© Photographee.eu / shutterstock.com
When it comes to early-career physicians interviewing for otolaryngology residency slots, it’s a story of haves and have-nots.
Third-year resident Andrew Lee, MD, of Johns Hopkins Medicine in Baltimore, reported that 19% of applicants took up 38% of available interviews. Just 26% of all otolaryngology applicants took up half of all interviews. Out of all the specialties reviewed, otolaryngology had the highest percentage of applicants taking up 50% of all interviews.
The review was based on the Gini coefficient, a scale of 0–1 that is more typically used to describe income disparity within countries. The higher the coefficient, the more unequal the distribution.
The research found that otolaryngology is less unequal than all of the other reviewed specialties, but largely because so many applicants “hoard” interviews. In fact, the Gini coefficient among otolaryngology applicants was 0.43, compared to 0.72 for internal medicine and 0.84 for family medicine. Traditionally, factors like the expense and effort of multiple meetings limit the number of interviews applicants can hoard.
But the specialty’s perceived competitiveness mitigates those factors, essentially encouraging more people to take as many interviews as they can. Residency programs, however, can use conflicting dates to try to make applicants interview only for those programs in which they’re most interested.
New Nasal Valve Obstruction Treatment
© Karan Bunjean / shutterstock.com
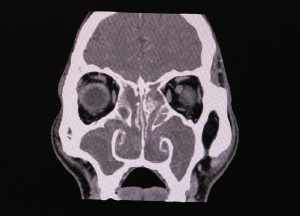
Ofer Jacobowitz, MD, PhD, of ENT Allergy & Associates in New York City, presented his study on the efficacy of a “novel in-office bipolar radiofrequency (RF) treatment” to relieve obstruction in the nasal valve area. The study, funded by Aerin Medical for FDA 510k clearance for its VIVAER nasal remodeling device, looked at its safety and effectiveness in heating and remodeling tissues in the nasal valve area to alleviate nasal obstruction.
The procedure is done under a local anesthetic with a specially designed probe, as compared with invasive nasal surgery in an operating room. Fifty patients with a Nasal Obstruction Symptom Evaluation (NOSE) scale score of at least 60 were selected for the study. Patients received a single treatment, and follow-up lasted for 26 weeks.
No serious adverse events were reported. The mean NOSE score fell from 79.9 at baseline (SD 10.8, range 60-100) to 24.7 at 26 weeks (SD 20.4, p<0.0001), results similar to those of nasal surgery, Dr. Jacobowitz said. He acknowledged that a limitation of the study was its small population and that follow-up extended for only about six months. But he added that a European pilot study found that the efficacy of similar treatment maintained positive results at a mean follow-up of two years.
Dr. Jacobowitz is working on a clinical trial to extend his follow-up information.
Early Swallow and Hearing Outcomes in Infants with Zika Exposure

© Surapol Usanakul / shutterstock.com
Si Chen, MD, of the House Ear Clinic in Los Angeles, presented a first-of-its-kind review of infants who were exposed to the Zika virus (ZIKV) in the year after the February 2016 public health emergency declaration by the World Health Organization (WHO). The report sought to quantify early swallow and hearing outcomes for those exposed in utero but born without microcephaly or imaging evidence of neurologic malformation.
The retrospective chart review tallied 89 ZIKV-exposed (ZIKVE) infants and 15 controls, based on pregnancies occurring between January 2016 and May 2017. Weight, length, and head circumference showed no major differences between the groups.
Ten ZIKVE infants demonstrated dysphagia and four ZIKVE infants failed newborn hearing screening. However, neither of those results was reported as statistically significant. The report also showed that the three infants who tested positive for Zika had brain abnormalities and swallowing issues. Dr. Chen says more follow-up will be done via a three-year Florida Department of Health grant that runs through 2020.
Future work will seek to correlate the severity of brain malformation with severity of dysphagia, as well as look at the prevalence and progression of hearing loss in both symptomatic and asymptomatic ZIKV infants.
Program-Specific Paragraph in the Otolaryngology Residency Application

© jannoon028 / shutterstock.com
Call it otolaryngology’s version of unintended consequences. The mandatory program–specified paragraph (PSP) within a residency applicant’s personal statement, introduced in the 2015-2016 application cycle, aimed to help program directors hone in on which applicants truly wanted to join an institution. But the PSP became controversial during the otolaryngology match process, because some saw it as imposing a required standard into one of the “only truly customizable elements” of an application, said Katelyn Stepan, MD, of Icahn School of Medicine at Mount Sinai in New York.
A retrospective cohort analysis undertaken by Dr. Stepan and her colleagues sought to assess the degree of variability among PSPs by looking at 181 applications to Icahn School of Medicine and the Massachusetts Eye and Ear Infirmary in Boston. The results suggest that applicants customize PSPs. Using a five-point scale and Levenshtein distance function, the researchers found the applications to be “mildly similar.” Each contained at least three unique points about the institution to which it had been submitted.
Dr. Stepan noted that, in recent years, there are more applications per otolaryngology applicant (and fewer overall applicants), because people perceive the specialty as competitive. The value of the PSP could be further studied to see what role it plays in that trend.
Richard Quinn is a freelance medical writer based in New Jersey.