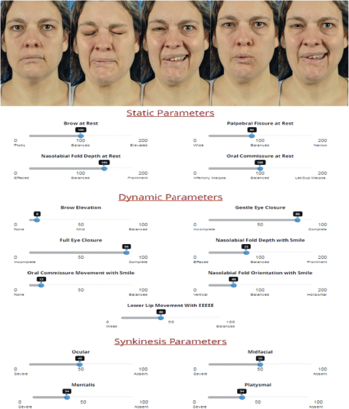
Facial grading using the electronic clinician-graded facial function (eFACE) scale in a patient with postparalysis facial palsy secondary to pregnancy-associated Bell’s palsy.
© The American Laryngological, Rhinological and Otological Society, Inc
Is pregnancy a risk factor for worse outcomes in Bell’s palsy (BP), and are these outcomes the result of factors intrinsic to pregnancy or the tendency to withhold medical therapy?
Bottom line
BP onset in late-term pregnancy and the immediate puerperium is a risk factor for worse long-term facial function outcomes than in nonpregnancy-related BP. Although there exists a strong tendency for medical therapy to be withheld in pregnancy-associated cases of BP, factors intrinsic to pregnancy appear principally responsible for the worse prognosis. Avoidance of systemic corticosteroids in the first trimester of pregnancy is prudent; however, use of corticosteroid and antiviral therapy in the late phase of pregnancy appears safe and should be discussed with patients presenting with pregnancy-associated BP (PABP).
Explore This Issue
December 2017Background: The incidence of Bell’s palsy (BP) is elevated in the late phases of pregnancy. A diagnosis of exclusion, BP is characterized by the rapid development of facial weakness involving all branches of the facial nerve, with ensuing recovery of function within six months. Although full recovery of facial function occurs in approximately 70% of cases, 30% of patients will develop postparalysis facial palsy. Controversy exists as to whether pregnancy is a risk factor for worse outcomes in BP, and whether such outcomes are the result of factors intrinsic to pregnancy or the tendency to withhold corticosteroid therapy in this cohort.
Study design. Retrospective analysis.
Setting: Department of Otolaryngology, Massachusetts Eye and Ear, Boston.
Synopsis: Long-term facial function outcomes in cases of PABP were compared against outcomes in cases affecting nonpregnant adult women of child-bearing age by a blinded expert using the electronic clinician-graded facial function (eFACE) scale facial grading system. Fifty-one pregnancy-associated cases and 58 non-pregnancy-associated cases were included. Among patients who received early corticosteroid therapy, significantly worse static, synkinesis, and composite facial function eFACE scores were demonstrated among cases of PABP compared with nonpregnancy-associated cases (static median = 86 vs. 92.5; synkinesis median = 79 vs. 86; composite median = 78 vs. 84). Among those not treated with corticosteroids, significantly worse dynamic and composite facial function eFACE scores were demonstrated in cases of PABP compared with those for nonpregnancy-associated cases (dynamic median = 74 vs. 92.5; composite median = 73 vs. 86.5). A trend toward improved outcomes was demonstrated within both groups for those treated with corticosteroids compared with those who were not.