In a short period of time, the criteria for appropriate selection for FESS has really shifted from a focus pathway to more of a quality of life focus pathway. —Adam Zanation, MD
Explore This Issue
April 2019
Invasive Fungal Rhinosinusitis
Stilianos Kountakis, MD, PhD, chairman of the otolaryngology department and director of neurorhinology-advanced sinus surgery fellowship at the Medical College of Georgia-Augusta University, underscored the continued essential role of surgery in the treatment of invasive fungal rhinosinusitis (FRS) which, when acute in immunocompromised patients, has a high mortality rate.
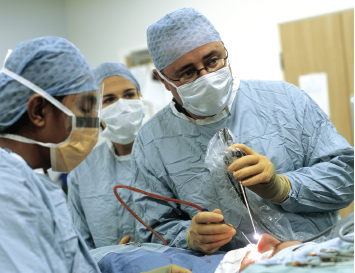
Sinus surgery is still an essential part of patient care, and some data support an expanded role for boosting quality of life.
© Mark Thomas / Science Source
In these patients, identified by edema, ulcerations, and necrosis on endoscopy; sinus ossification and bone necrosis on CT; and fungal particles invading the mucosa with thrombosis, ischemia, and necrosis on biopsy, there is an urgent need for surgical debridement, Dr. Kountakis said. “It’s a question of minutes sometimes, and hours, instead of days,” he said. “All the necrotic debris and tissue has to be removed until we encounter bleeding tissue. Once we do that, the patients may have a chance.” Then, patients should receive anti-fungals to fight the disease, he said.
For the allergic version of FRS, a subclass accounting for approximately 10% of the surgical cases in the U.S. and usually involving young, immunocompetent people with a fungal atopy, endoscopic sinus surgery provides a definitive diagnosis, he said. Key to resolving the symptoms is removing all of the fungal and eosinophilic debris, followed by medical management to control the underlying disease.
Endoscopic Sinus Surgery
Adam Zanation, MD, professor of otolaryngology at the University of North Carolina, said that recent findings suggest that the role of endoscopic sinus surgery is likely to expand for certain patients.
A 2019 study published in The Laryngoscope proposed that criteria for appropriateness for surgery in the management of uncomplicated adult chronic rhinosinusitis should be minimum prior therapy; a Sino-Nasal Outcome Test (SNOT-22) score of 20 or higher; and a CT Lund-Mackay score of 1 or higher (Laryngoscope. 2019;12:37–44). “Several years ago, a CT Lund of 1 would likely not have meant surgery,” he said. “We’ve opened ourselves up to a broader range of patients we can help from a quality-of-life perspective.”
Studies have found that baseline CT scores don’t necessarily correlate with quality-of-life outcomes after FESS, he said. “In a short period of time, the criteria for appropriate selection for FESS [functional endoscopic sinus surgery] has really shifted from a focus pathway to more of a quality-of-life focus pathway,” he said.
But questions remain as to which type and what extent of FESS is best, he said. Data from a study of 311 patients with CRS suggests similar benefits for a complete versus a targeted approach, done according to physician discretion (Int Forum Allergy Rhinol. 2015;5:691-700). Those undergoing the complete procedure had a higher prevalence of asthma, aspirin sensitivity, nasal polyps, and history of prior surgery. While the overall SNOT score was higher for those undergoing a complete procedure, there was no difference in the number of patients showing improvement between the two groups, Dr. Zanation noted.
“Both FESS and extended endoscopic endonasal surgery have had and will continue to have expanding roles,” he said. “Research and innovation and outcomes and value studies will be key to protecting this growth.”