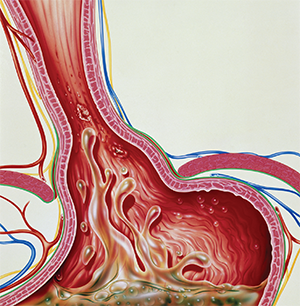
Gastroesophageal reflux.
© John Bavosi / Science Source
Despite the huge number of people who suffer from its effects, evaluation and treatment of laryngopharyngeal reflux (LPR) can vary widely, and the tools are far from perfect. Experts discussed their approach to LPR, shedding some light on many of the issues otolaryngologists face.
Explore This Issue
March 2017Moderator Seth Dailey, MD, chief of laryngology and voice surgery at the University of Wisconsin School of Medicine and Public Health in Madison, said that gastroesophageal reflux disease (GERD) affects approximately 40% of the population, with cost estimates ranging from $9 to $12 billion a year. Proton-pump inhibitors (PPIs) are the most costly prescribed medication in the U.S., he said. What’s more, the yearly cost of direct care for patients with LPR, including tests and medications, is five times what it is for patients with GERD, he said. (Am J Gastroenterol. 2013;108:905-911.)
When it comes to evaluation and treatment by otolaryngologists, he said, reflux manifests itself in many forms, and a diagnosis can be difficult to nail down. Overdiagnosis is likely common, and there can be harmful side effects from treatment.
Some of the tools otolaryngologists use have been called into question, he noted. The rigor with which the nine-question reflux symptoms index (RSI) was tested came under scrutiny in a paper published in December 2016 (Otolaryngol Head Neck Surg. 2016;155:923-935). And the reflux finding score, used to grade findings on office laryngoscopy, was found in a 2014 study to offer poor inter-rater reliability and no correlation with reflux in healthy, untreated volunteers (Laryngoscope. 2014;124:2345-51).
Dr. Dailey suggested that the field may even need to come up with a more reliable language to describe reflux. When talking about LPR, he said, “Is it disease? Is it symptoms? I’m not sure. So should we be moving toward a more common nomenclature? And where do we draw the line between what are classically described as GERD or esophageal symptoms … versus LPR symptoms?”
He and panelists also made these points as they discussed their approach to handling reflux patients.
PH Impedance Testing
Gaelyn Garrett, MD, professor of otolaryngology and senior executive medical director of the Vanderbilt Voice Center in Nashville, cautioned against otolaryngologists bringing a bias to these cases that favors a reflux diagnosis from the start. “You can’t take the next step until you evaluate other potential causes,” such as allergy or sinus, she said. “I do think reflux is a contributor in a lot of what we see, but I hate to jump directly to say, ‘How are we going to evaluate this person for their reflux symptoms?’”