Dizzy patients are among the most challenging, time-consuming cases that are seen in otolaryngologists’ offices. The cause of the vertigo is often difficult to establish, and effective treatment is often elusive. Therefore, it can be helpful to know which vestibular tests can be effectively conducted in the general otolaryngology clinic and which ones are typically performed in a referral clinic specializing in balance disorders.
In several phone interviews, several vestibular disorder experts discussed some basic in-office techniques as well as novel testing modalities that are typically available in referral clinics or hospitals.
Patients who present with vestibular complaints typically will involve more time than the usual patient with sinusitis or middle ear fluid or any number of other pathologies that the general otolaryngologist encounters, said James Soileau, MD, the senior partner of the Ear and Balance Institute in Baton Rouge, La.
Often it’s difficult to get a clear history because the dizziness has been ongoing for some time. Therefore, the most important consideration is to be able to allocate some extra bit of time to get a very good history. The clinical exam should include extra diagnostic tests to get a good clinical picture on the first visit.
Those tests should be accompanied with good counseling from the physician regarding the tests’ potential benefits, said John Epley, MD, Director of the Portland Otologic Clinic (Ore). The major problem with most vestibular testing is patients’ over-expectations regarding what benefits they will get from the test, said Dr. Epley. They are not aware of the limitations of the tests commonly performed in clinics.
We need to heighten the awareness of migraine and superior canal dehiscence to stop these cases from falling through the cracks, – Dr. Goebel said.
Other problems include out-of-date standards and reimbursement difficulties, he said. All of these barriers can result in inadequate testing of vestibular patients.
A Poorly Understood Urgency
Vestibular testing is currently poorly covered, with reimbursement often not available or sharply discounted. The reason for this is that the urgency of dizziness is poorly understood, Dr. Epley said. People can die from falling, but dizziness is not seen as something that can kill you, he said. It’s taken a long time for people to understand that dizziness originates in the ear in 95% of cases.
The otologic origin of dizziness is still poorly recognized, he said, noting, I frequently see patients who have been sent to psychiatrists for vertigo. Dizziness increases in prevalence with age, he said. Approximately 9% or 10% of elderly have BPPV [benign paroxysmal positional vertigo], but they’re dizzy and don’t know why, he said. The lifetime chance of developing vertigo must be 25% to 50%.
Kamran Barin, PhD, Assistant Professor of Otolaryngology at Ohio State University in Columbus, agreed with Dr. Epley regarding the frequency of dizziness. The general otolaryngologist is the one who sees dizzy patients, he said. It’s important to realize what kind of vestibular testing is available, when patients should be referred and for which tests, and which in-office tests can be done to see what is the most appropriate route for managing the condition.
In-Office Tests
All available vestibular function tests are quite limited, said Joel Goebel, MD, Professor of Otolaryngology and Head and Neck Surgery at Washington University in St. Louis, Mo., where he is the Director of the Dizziness and Balance Center.
The ultimate test would one that evoked potential, he said. Can you do a stimulus and evoke a potential to show which part of the inner ear is involved and the degree of involvement? We don’t have a perfect evoked potential.

The lack of direct access to the vestibular system is a key factor in the limitations of vestibular function testing, he added. We don’t have a direct access to the vestibular system, so we have to look at proxies, he said. These include eye movements and postural movements. Because we don’t have direct access and use proxies, our tests are not that specific.
However, several tests that can be performed in the otolaryngology clinic are quite useful. Two tests that can help the general otolaryngologist establish the cause of the vertigo are the Tullio response test and the pressure response test, he said.
Tullio and Pressure Tests
The Tullio test involves putting a tuning fork to the ear of a standing patient. With the pressure test, the clinician applies a squeeze bulb to the patient’s ear and watches the eyes for the onset of nystagmus. These tests can identify which ear is implicated in the balance problem, Dr. Epley said. He added that he is working on a device that will give a quantified amount of sound and pressure in the ear so that the results are standardized.
Dr. Soileau stressed that the exam should include a careful examination of the patient’s cranial nerves and hearing, either with tuning forks or by an audiometric study.
Dix-Halpike Maneuver
Next, consider a Dix-Halpike maneuver, Dr. Soileau said. This maneuver involves bringing the patient from a lying to a sitting position with the head in one position and allows the physician to assess for nystagmus or dizziness symptoms.
One problem with BPPV is that the symptom complex can wax and wane, he said. Even if you don’t see it the first time, you’re obligated to look for it again. Just because it was in remission or symptoms were weak on one occasion doesn’t mean the patient doesn’t have it. If the history is compatible with BPPV, you’re obligated to look for it.
Head Shaking Tests
In addition to these tests, there are three other tests people should do in the office, said Dr. Goebel. Those are the head impulse test, the head shake test, and dynamic visual acuity.
With the head impulse test, the patient shakes the head side to side and the doctor asks the patient to view a target to test whether the patient can keep his or her vision aligned on the target. The head impulse test detects damage to the vestibular system; if the gaze slips on both sides, both ears could be involved, Dr. Goebel said.
With the head shake test, the patient closes his or her eyes or puts on Fresnel lenses and shakes his or her head for 20 seconds, after which the clinician looks for nystagmus. This test can identify peripheral vestibular lesions, he said, noting that the eye will beat toward the better ear.
The dynamic visual acuity test (DVAT) involves the patient reading an eye chart. Then, with the patient reading the lowest line of best corrected vision with the head still, you shake the patient’s head and ask them to read, he said. They should still be able to read within three lines. If not, the vestibular system is not well timed, he said.
Dr. Goebel agreed with Dr. Soileau that these tests should be done along with the Dix-Halpike test. An update of this, the computerized DVAT, is in development, Dr. Goebel said.
Nystagmography
The electronystagmography (ENG) and the videonystagmography (VNG) which document various changes in position and oculomotor tests, are considered the gold standard for assessing dizziness, yet I see patients who have had these tests but nothing has been found, Dr. Epley said. That’s because they only test a limited amount of pathology.
He added that the positions used may not be the triggering positions, and that clinicians need to be exhaustive in their use of positions in order to determine whether the patient has BPPV.
Dr. Soileau added that using VNG or Fresnel lenses enhances the physicians ability to observe the patient’s eye movements while doing this maneuver. Oftentimes this is relegated to the audiologist or physical therapist, and unfortunately, many neurootologist relegate this important part of the clinical exam to other assistants, he said.
However, it is probably one of the most important clinical exams that should be included in the evaluation of every patient with complaints of vertigo. Far and away, the most common cause of vertigo is BPPV. If you don’t look for it, you won’t find it.
Types of Vestibular Function Tests
Tests that can be performed in the general otolaryngology clinic
- Tullio response test
- Pressure response test
- Dix-Halpike maneuver
- Head impulse test
- Head shake test
- Dynamic visual acuity test
- Electronystagmography (ENG)
- Videonystagmography (VNG)
- Fresnel lens test
- Gait test
- Step test
- Caloric test
Tests that are typically performed in referral clinics
- Rotary chair test
- Epley Omniax chair
- Posturography
- Vestibular evoked myogenic potential (VEMP)
- Subjective visual vertical test (SVVT)
Other Office-Based Tests
Several other tests involve technique but not technology, Dr. Soileau said. These include the gait test and the step test. The gait test involves the patient standing initially with feet together and eyes closed. The clinician then observes the patient walking down the hall and making turns to see whether the patient is more coordinated when turning to the right or left.
With the step test, the patient walks in place with eyes closed and the clinician watches to see whether there is any drift to one side or the other, which would indicate a unilateral reduction of vestibular function.
The caloric test, which involves putting hot and cold fluid sequentially in each ear, helps the clinician to localize the ear that is implicated in the patient’s balance problems. It only tests the lateral canal, Dr. Goebel said. When highly positive, with very different results for one ear versus the other, it’s very useful. A colder stimulus should be used if the change is the same on each side with cold water. If the study is with cold water, the patient should be referred for a rotary chair test.
Limitations
Dr. Goebel noted that conventional vestibular tests miss two types of dizzy people. Those include migraine-related dizziness, who have normal test results but whose dizziness is triggered by photophobia, and those whose dizziness is triggered by loud sounds. However, with astute testing, these diagnoses can be teased out, he said.
With VNG, if the patient is sound-sensitive, you can use a loud sound and look for eye movement, he said. If you get that, you can send them to get an x-ray or high-resolution computed tomography [CT]. Tell the radiologist that you suspect superior canal dehiscence and ask for a thin-cut CT with bone windows and ask the radiologist to reconstruct in the plane of the superior canal because you’re looking for a hole.
He added that otolaryngologists should suspect this underlying cause for the dizziness if the patient complains of dizziness, is sensitive to sound, and the CT shows that there is no bone in the area.
Identifying this cause can spare such patients unnecessary surgery for suspected fistulae, he said. Migraine-related dizziness can be identified with questions regarding light sensitivity.
Specialty Clinic Tests
Because of the costs of the equipment, all of the experts interviewed agreed that some of the more advanced tests, such as the rotary chair test, are most appropriately performed at referral clinics.
It’s a select group of people that need the rotary chair test, Dr. Goebel said. That group includes those who don’t have caloric responses and those with a unilateral vestibular function loss. Another group would those with a unilateral loss, but with an unknown amount of central nervous system compensation.
Rotary Chair Tests
The rotary chair test involves the patient sitting in a chair, head affixed to a head holder and using video goggles as with VNG. The testing system uses software to lock on the pupil for a tracing of the eye movement and calculates how well the patient’s system is making eye movements when moving to the right or left.
A variation of this, eccentric rotation, utilizes asymmetric stimulation of the inner ear, particularly the utricle. This test may be the first to give an idea of utricular function, Dr. Goebel said.
Noting that the standard rotary chair has limitations regarding speed, Dr. Epley pointed out that he has developed the Epley Omniax chair, which is manufactured by Vesticon, to address these limitations and to allow for a fuller positional test. Since patients with cupolalithiasis have vertigo in some positions but not in others, the Omniax chair puts patients in all of the positions, he said. The chair is still being reviewed by the Food and Drug Administration.
Because rotary chairs can be costly, in the neighborhood of $100,000, others are using a less costly device: a computerized headband that can measure acceleration of eye and head movement in horizontal and vertical planes.
Patients are asked to watch a target on the wall while moving their heads back and forth with varying frequencies. The headband records head motion and acceleration and eye movement, and then the software calculates whether the vestibular ocular reflex system is working.
Other Specialty Tests
Posturography, which involves placing the patient on a platform in various positions with eyes open and closed, can enhance ENG and VNG by narrowing down the causes of dizziness. For example, the test could identify whether the nystagmus is sound-evoked, which would involve a disorder in the semicircular canal.
One new test, the vestibular evoked myogenic potential (VEMP), consists of electrically transmitting a sound into the ear. If the receptors of balance are damaged, the patient will then report the sensation of the room spinning. This test would be the closest version of an evoked potential, Dr. Goebel said.
One test in development is the subjective visual vertical test (SVVT). With the SVVT, the patient is asked take a light bar and place it in a vertical plane in complete darkness. Patients with vestibular problems tend to shift the bar to one side, Dr. Goebel said. It’s not ready for routine clinical testing, but it’s emerging as an easy way to examine the vestibular system, he said.
Treatment
The experts interviewed agreed that testing should not only be for diagnosis, but also to help clinicians identify treatment. Testing can help us identify unusual problems that may be the cause, such as acoustic neuroma, Dr. Goebel said.
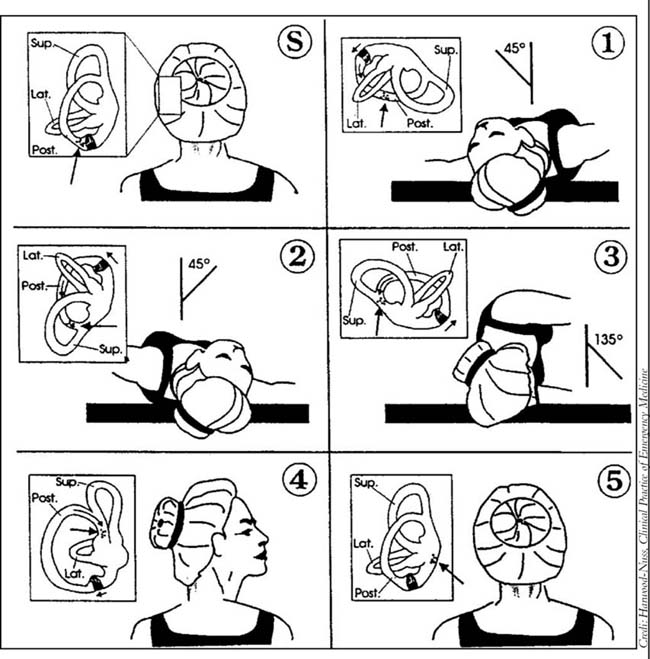
If a patient has BPPV and if the affected canal has been identified, the proper treatment is the Epley maneuver, Dr. Soileau said. The maneuver involves moving the head in a way that encourages the misplaced otoliths to move out of the affected canal and back into the chamber that is their proper residence.
The Epley maneuver is an easy, gentle, and highly effective way to resolve BPPV, Dr. Soileau said. The more vigorous Semont maneuver involves turning the patient’s head and rapidly moving the patient from a sitting to a reclining position on one side and then on the other side.
A Conjunction of Exam and History
Otolaryngologists need to understand the limitations of vestibular tests and communicate those limitations to patients in order to use the tests effectively, Dr. Barin said.
If physicians are sending patients for vestibular testing and patients are expecting the test to tell exactly what disease is causing the dizziness, the patients will be very disappointed, he said. This is where otolaryngologists need to help patients see that the glass is half full. These tests provide such information for half of patients.
The tests are more helpful if they are viewed in the context of the overall evaluation, Dr. Barin continued. Vestibular tests cannot be useful without complete history, he said. Once the physician understands that, the testing can be a great adjunct to the diagnosis.
Dr. Goebel echoed this emphasis on the exam and the history. If you’re thorough, you can identify the cause in 85% of cases, and testing will identify another 10% to 15%, he said. Among these you can identify the causes by the history in 70% of cases. Listen for expressions of vertigo; BPPV patients will tell you that the world is in motion.
©2006 The Triological Society

Leave a Reply