What is the effect on glottic gap and voice quality of medialization laryngoplasty (ML) alone versus ML with arytenoid adduction (AA) in unilateral vocal fold paralysis (UVFP) patients?
Bottom line
ML with AA, but not ML alone resulted in statistically significant improvement in PG UVFP, meaning that patients undergoing ML may benefit from AA when a large posterior glottic gap is present.
Explore This Issue
November 2017Background: Three procedures are commonly performed to permanently treat UVFP: laryngeal reinnervation, ML, and AA. There are no widely accepted indications for AA, and the need for it preoperatively or intraoperatively is determined in different ways at different institutions. There is also a debate over whether the addition of AA to ML truly improves clinical outcomes, as well as concern that adding AA increases complication rates.
Study design: Retrospective case series of UVFP patients treated with ML alone (47) and ML with AA (27) between 2011 and 2016.
Setting: University of California San Francisco Voice and Swallowing Center.
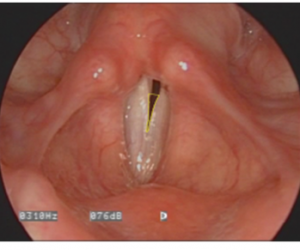
Calculation of anterior glottic gap area in pixels using Image J software. Anterior gap is traced out in yellow and pixels within the lines are calculated. Normalized gap is then calculated by dividing anterior gap by the square of vocal fold length times 100.
© The American Laryngological, Rhinological and Otological Society, Inc
Synopsis: There were no statistically significant differences between groups in gender, age, UVFP laterality, prior laryngeal procedures, or subsequent revision laryngeal surgery. There were, however, statistically significant differences in UVFP etiology between groups, including iatrogenic vagus or recurrent laryngeal nerve (46% of ML patients versus 74% of ML-AA patients) and cancer (20% ML versus 0% ML-AA). Of the six voice parameters measured, overall severity and roughness had acceptable intrarater and interrater reliability between all three graders. Overall severity, roughness, and strain were not statistically different between the two treatment groups both preoperatively and postoperatively. In the ML group, normalized anterior gap (AG) was visualized in 41 preoperative and 39 postoperative recordings; normalized posterior gap (PG) was visualized in 22 preoperative and 21 postoperative recordings. AG improved in both groups (ML group: 4.4 to 0.8; ML-AA group: 3.3 to 0.6), while PG improved in the ML-AA group from 1.8 to 0.5. Limitations included the study’s retrospective nature, selection bias in forming treatment groups, relatively small sample size, inability to visualize AG and PG in all recordings, and relatively less experienced speech language pathologist graders.