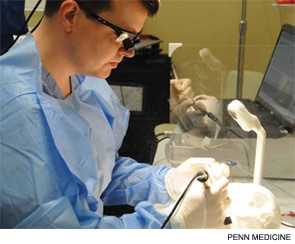
In May, Marcelo Antunes, MD, chief resident of otorhinolaryngology-head and neck surgery at the University of Pennsylvania, was able to practice bilobed flaps on pig’s feet at an ORL Rising Chief Boot Camp held at Penn Medicine Clinical Simulation Center in Philadelphia. While he had previously experienced medical simulation during his otolaryngology residency, the boot camp put the methodology in proper context for Dr. Antunes, who is particularly interested in facial plastics.
"When you think about local skin flaps, such as the rhomboid or the bilobed, they’re very easy in theory," he explained. "You measure the defect, cut here, cut there and rotate the skin in. But there is a big difference when you’re actually doing it, like when we did it on the pig’s feet. You appreciate so much more the little nuances involved in it. You realize how much undermining of the skin is needed, and if we didn’t shape the flap just right, placing the incision over the relaxed skin tension lines, it was not going to look good. That was something you would only appreciate after you do it."
Otolaryngologists say the use of simulators, from the boot camp’s animal models to the most advanced mannequins and attached laboratories that can cost hundreds of thousands of dollars, has grown in academic otolaryngology programs in recent years. And now the simulation programs may be poised to grow even faster, thanks to the new work-hour rules from the Accreditation Council for Graduate Medical Education (ACGME). The new rules maintain the established cap on overall hours at 80 per week, averaged over four weeks. However, first-year post-graduates, as of July 1, are now limited to 16 hours a day, a rule that, in effect, forces a rest period.
While the new rules are aimed at reducing medical errors and adverse events caused by sleep-deprived residents, some worry that reducing a first-year’s available hours will also reduce the student’s level of preparedness. And that’s where simulation comes in.
"I think it’s going to be a hugely useful tool to help manage the limitations of the ACGME rules," said Ellen Deutsch, MD, FACS, FAAP, director of surgical and perioperative simulation at the Center for Simulation, Advanced Education, and Innovation at the Children’s Hospital of Philadelphia. She was one of several otolaryngologists to organize this spring’s boot camp, which drew 14 fourth-year residents. In July, 31 second-year residents attended the Second Annual ORL Emergencies Boot Camp.
Leave a Reply