Bone-anchored hearing aids (BAHA) provide many patients who can’t use standard hearing aids-for example, those with ear malformations or chronic infections-the potential to restore their hearing.
Explore This Issue
October 2007Patients should understand that good auditory function is possible with the BAHA, said Darius Kohan, MD, Clinical Associate Professor in the Department of Otolaryngology at New York University School of Medicine. Patients who get a BAHA are usually ecstatic, he said. They hear much better.
If the patient’s cochlear function is good, then they can have very good expectations about being able to hear with a BAHA, agreed Anders Tjellström, MD, PhD, Professor in the Implant Unit of Department of Otolaryngology at Sahlgrenska University Hospital in Göteborg, Sweden, and one of the original developers of the BAHA technology, first used in 1977.
One of the BAHA’s newer indications is for patients with unilateral hearing loss. While it is definitely beneficial in many patients, they should know the device won’t give them true bilateral hearing, noted John House, MD, President of the House Ear Institute.
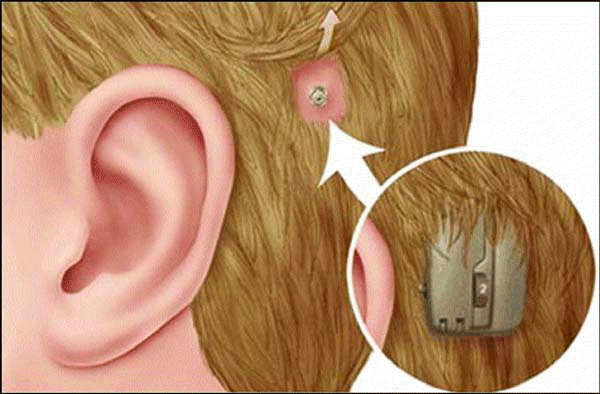
How BAHA Works
The BAHA is not really a hearing aid, said Dr. House. It works on a totally different principle and is meant for people who do not use or benefit from a standard hearing aid.
The BAHA consists of a sound processor attached to an external abutment, which is held in place by a titanium screw implanted into the skull behind the ear. The bone carries vibrations that bypass the external and middle ear and travel directly to the cochlear nerve.
The beauty of the device is you can’t tell the difference between whether the sound comes through the ear canal or bone, and the patient has quite natural hearing, explained Dr. Tjellström.
Who Benefits from BAHA
BAHA is used in patients with chronic ear infections that cause conductive or mixed hearing loss and for whom a hearing aid would aggravate the infection, said Dr. House.
About 70% of BAHA patients have chronic ear disease or a perforation in the eardrum, said Dr. Tjellström, adding that a conventional hearing aid may not be feasible in these patients because of drainage through the ear canal.
BAHA is also indicated for people who do not have an ear canal or who have aural atresia and cannot wear a conventional hearing aid, said Dr. House.
Physicians have started performing more BAHA surgery in children with aural atresia, said Sam Marzo, MD, Associate Professor in the Department of Otolaryngology and Head and Neck Surgery at Loyola University Health System in Maywood, IL, and a consultant for Cochlear Corporation.
These patients can wear a tight headband with a bone-conducting hearing aid attached to it, but they are frequently noncompliant because they get headaches, making surgery the better option, he explained.
Another BAHA indication, approved in 2002 by the US Food and Drug Administration, is for patients with unilateral sensorineural hearing loss. These individuals wear the BAHA in the ear in which they cannot hear, and the device conducts sound through the skull to the opposite ear’s existing cochlear nerve, explained Dr. House.
In a recent study presented in April at the Combined Otolaryngology Spring Meeting (COSM) in San Diego, Dr. House and his colleagues evaluated questionnaires about hearing completed by 59 patients with BAHA implants and 54 patients without the implants. All individuals had severe to profound unilateral hearing loss.
The researchers found that patients experienced improvements in background noise, ease of communication and reverberation of 16.1%, 11.4%, and 5.4%, respectively. However, localization of sound was difficult for patients with unilateral deafness even with a BAHA, the researchers found.
Another option for this type of hearing loss is the contralateral routing of signals (CROS) hearing aid. However, this device uses a wire to conduct sound to the opposite ear, which can be cumbersome for patients, explained Dr. House.
A transcranial hearing aid in the deaf ear also transmits sound to the opposite side by bone conduction, added Dr. Kohan. However, the tight fit of the ear mold deeply into the canal is often painful, he said.
Surgical Implantation
Regardless of the indication, implanting the BAHA requires making an incision behind and above the ear and undermining an area of skin and soft tissue that is about 2 cm in diameter, explained Dr. House. The reason we undermine the skin is so the implant is flush with the bone and the skin does not grow over the abutment, he explained.
Then a small hole about 1 to 2 mm wide and 3 to 4 mm deep is drilled into the bone and the titanium implant is placed in the skull. An abutment is attached to the implant, and three months later a sound processor is connected to this abutment.
Adults can usually undergo the implant surgery while under local anesthetic or sedation, said Dr. Marzo. It is generally an outpatient procedure that takes 30 to 45 minutes, he added.
In children, the surgery is performed with general anesthetic and often in two stages because pediatric patients have thinner tissue and bones, said Dr. Kohan. The first stage involves placing the titanium implant. The second stage of exposing the implant and attaching the abutment and processor occurs three to six months later, after osseointegration occurs, he explained.
Lately, we’ve been doing the procedure in one stage, said Dr. Kohan. He and his colleagues documented the safety of the one-stage procedure in a retrospective review of 27 children who underwent BAHA in 30 ears between 2002 and 2006. These data were also presented at COSM.
Complications
Skin overgrowth of the abutment and infection are the most common complications associated with having a BAHA implant, said Dr. Tjellström.
However, careful cleaning of the implant area can help to prevent these events. The first patient to receive a BAHA in 1977 has not had a single episode of an adverse skin reaction, said Dr. Tjellström.
Although complications are often preventable, sometimes revision surgery is necessary, said Dr. Marzo. He and his colleagues recently conducted a retrospective review, presented at COSM, of BAHA procedures performed at his institution between September 2003 and September 2006 to see how many required revision.
Ninety-two BAHA implantations were performed on 80 adult patients for unilateral conductive, mixed, or sensorineural hearing losses. Of these individuals, 10 underwent 11 revision procedures, with one patient requiring two reimplantations.
Four patients experienced loss of their skin grafts probably because of increased scalp soft tissue thickness, they reported. The remaining six patients experienced skin overgrowth, which physicians addressed with longer abutments and good wound care.
Another possible complication that did not occur in the study is device extrusion, noted Dr. Marzo. However, this is also preventable with good surgical technique and follow-up wound care.
Also of note is that the abutment can break due to trauma from games or sports, although wearing a helmet can prevent this from happening, added Dr. Kohan. Additionally, osseointegration fails to occur in about 5% of patients, he said.
Room for Improvement
While BAHA can successfully provide patients with good hearing, there is room for improvement, said the experts interviewed for this article.
Digital technology and omnidirectional microphones may one day provide better hearing to people with more significant hearing loss, said Dr. House.
In addition, researchers need to work on better integration of the fixture into the bone to ensure osseointegration, said Dr. Kohan. We need to find ways to attach the device and maintain it so it is more secure, he said.
Eventually, the metal pin and processor may be combined, or the processor may be attached with a magnet, added Dr. Kohan. Placing BAHAs under the skin may also be possible because increasingly smaller devices are becoming implantable. There’s a lot of room for growth and improvement, he concluded. This is a growing technology.
©2007 The Triological Society


Leave a Reply