Computational modeling (CM) is the use of computers to build a model of a plan or procedure to find ways to improve outcomes. Early research indicates that studying this type of modeling may have a large impact on otolaryngology surgery at all stages.
Explore This Issue
May 2017The hope is that CM will eventually be able to guide surgeons to help prevent potential errors, increase patient safety, and predict outcomes. The information would be based on known scientific evidence indicating that, if a procedure is performed a certain way, the physician can expect certain types of outcomes, said Grace C.Y. Peng, PhD, a program director in the division of discovery science and technology at the National Institute for Biomedical Imaging and Bioengineering (NIBIB) in Bethesda, Md. “The idea is to eventually develop models to be more predictive and more proactive to get the best possible outcome on the first try,” she added.
Surgery is a common treatment for nasal airway obstruction (NAO); however, its failure rate is high. “Currently, between 25% and 50% of surgeries to correct NAO fail to completely resolve the patient’s symptoms,” said Dennis O. Frank-Ito, PhD, an assistant professor of surgery in the division of head and neck surgery and communication sciences at Duke University Medical Center in Durham, N.C. “This implies that as many as one out of every two surgeries will not produce the desired outcome,” he added. For this reason, he and his colleagues became interested in determining how they could apply computational technologies to aid surgical planning for NAO treatment, potentially improving outcomes.
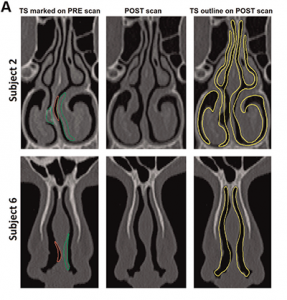
Figure 1. 3D transcribed-surgery models. Left: Digitally created airspace (green) and closed airspace (red). Right: Transcribed-surgery (yellow) superimposed on postsurgery.
© marcinswiostek / shutterstock.com
As an early proof-of-concept study, Dr. Frank-Ito and his team prospectively constructed nasal models from computerized tomography (CT) scans of 10 patients undergoing surgical treatment for NOA (see Figure 1, and Figure 2). The scans were taken prior to surgery, and five and eight months following surgery. To create the transcribed-surgery and post surgery models, the surgeon digitally hand-edited the preoperative scans to represent the physical changes that were expected from the surgery. Steady-state, laminar, and inspiratory inflow were simulated in each model. The results were not as robust as they had hoped, largely related to software limitations (Otolaryngol Head Neck Surg. 2014;151:751-759).
“We hope that, eventually, this will become a way for the surgeon to meld radiologic and other studies into a platform that lets them virtually plan and even practice long before they enter the nose,” said Dr. Frank-Ito. “The pre-surgery platform would allow surgeons to ‘try out’ different procedures virtually before deciding the best procedure to perform on a given patient.”