Even as an endoscopic approach to malignant sinonasal tumors appears to be increasingly popular, this treatment is stirring debate within the medical community due to the lack of long-term study data showing that the technology is as effective as open surgery.
Explore This Issue
May 2009Open cranial facial resection has been the workhorse for sinonasal tumors for more than 50 years, said Pete Batra, MD, Assistant Professor of Surgery at the Head and Neck Institute and Section Head of Nasal and Sinus Disorders at the Cleveland Clinic Foundation. However, this paradigm shifted about 20 years ago with the introduction of endoscopy to the field of otolaryngology-head and neck surgery.
Over the past decade, endoscopes have been used for orbital and pituitary surgery and the removal of benign tumors such as angiofibromas, osteomas, and inverted papillomas, explained Dr. Batra. This experience has culminated in an endoscopic approach to malignant sinonasal tumors, including those that extend to the anterior skull base, he said.
Although endoscopy has been successful in removing benign tumors, using this approach to treat malignant tumors is still very controversial, said Carl Snyderman, MD, Professor of Otolaryngology and Neurological Surgery and Co-Director of the Center for Cranial Base Surgery at the University of Pittsburgh School of Medicine. There are still a lot of skeptics.
John Osguthorpe, MD, Professor in the Department of Otolaryngology-Head and Neck Surgery at the Medical University of South Carolina in Charleston, cautions that the treatment of benign and malignant sinonasal tumors should not be lumped together. There’s a big division between what has been documented as effective by larger series with long-term follow-ups for benign paranasal tumors and what has been [documented] for malignant tumors, he said.
Sinonasal malignancies are sporadic and their treatment should not be the same as that of benign tumors, agreed Dennis Kraus, MD, Attending Surgeon in the Head and Neck Service at Memorial Sloan-Kettering Cancer Center and Professor of Otorhinolaryngology at Cornell University Medical Center in New York.
 There’s a big division between what has been documented as effective by larger series with long-term follow-ups for benign paranasal tumors and what has been [documented] for malignant tumors.
There’s a big division between what has been documented as effective by larger series with long-term follow-ups for benign paranasal tumors and what has been [documented] for malignant tumors.
-John Osguthorpe, MD
Using endoscopy on the pituitary is a lot different than endoscopic sinonasal surgery for a malignancy, he said. However, the role of endoscopy in the treatment of sinonasal malignancies is increasing as a new generation of physicians enters head and neck surgery, he noted.
The Controversy
Most of the limited experience with endoscopic treatment of malignancies centers on lower-grade lesions, principally esthesioneuroblastomas at the Kadish A/B stage, said Dr. Osguthorpe. Very little information exists, aside from what is technically feasible, on longer-term control of endoscopically resected higher-grade lesions, and as with any topic where there’s inconclusive information yet major interest, it’s controversial, he said.
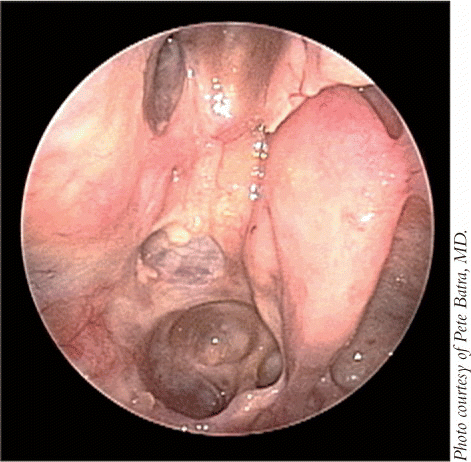
During the 1980s, the optimal treatment of esthesioneuroblastoma was a source of debate not among surgeons, but between surgeons and radiation oncologists, because the tumor is relatively sensitive to radiation. Today, most physicians favor surgery for esthesioneuroblastomas, with or without radiation, depending on tumor stage, said Dr. Osguthorpe. If a tumor is early-stage, confined to the nasal cavity, or with modest adjacent sinus involvement, a transnasal endoscopic approach supplemented by external beam radiation to the anterior fossa floor, primarily the olfactory bulb region, may be appropriate, he said (citing Unger et al. Minim Invasive Neurosurg 2001;44: 79-84).
Radiation is expected to control minor disease spread through the cribriform plate, a finding Dr. Osguthorpe encountered in a patient who presented with a 2-cm solely intranasal esthesioneuroblastoma on MRI, yet had microscopic disease in the ipsilateral olfactory bulb.
Alternatively, the surgeon can resect the olfactory region via an endoscopy alone, but challenges associated with defect closure and maintaining the safety of adjacent intracranial structures may arise, said Dr. Osguthorpe, adding that few physicians currently have the expertise to use this approach. For larger tumors with obvious skull base or anterior fossa involvement, a formal craniotomy, endoscopically assisted on the transnasal portion of the procedure, may be prudent, and is usually combined with postoperative irradiation, he said.
Generally, radiation needs to be employed after both endoscopic resection and open craniofacial surgery, said Dr. Kraus. However, the goal of either procedure is to completely resect the entire tumor, he added.
Overall, an endorsement of endoscopic resection of aggressive or advanced malignancies should be withheld until long-term data are available to support its use, said Dr. Osguthorpe, noting that this view was also expressed by Paul Levine, MD, at the Ogura Lecture given at the at the Triological Society 111th Annual Meeting in Orlando, FL, last spring (Laryngoscope 2009;119:3-7; ENT Today 2008(7); 3:8-9).
Moreover, endoscopic treatment of these tumors should occur only in a clinical trial setting with long-term follow-up, so physicians can learn from the experience, added Dr. Osguthorpe.
Dr. Snyderman noted that many surgeons who are doubtful of using endoscopy for sinonasal malignancies support en bloc surgery, which involves working around the periphery of the malignancy and taking out the entire tumor with a margin of disease-free tissue around it.
However, in skull base surgery, small spaces and proximity of nerves and vessels to the tumor make en bloc surgery challenging, said Dr. Snyderman. The optic nerve, carotid artery and brain make achieving margins technically difficult, he explained.
Increasing evidence indicates that en bloc procedures aren’t necessary and that tumors can be removed a little bit at a time, said Dr. Snyderman. For example, during supraglottic laryngectomy, surgeons can remove cancers at the top of the voice box in a piecemeal fashion through the mouth, using a laser. Results are as good as in open procedures, he said.
There are no published data suggesting that taking tumors out in a piecemeal manner is better than taking the entire tumor out at once for either endoscopic or open surgery, with the stated goal of complete tumor resection, noted Dr. Kraus.
Physicians can also treat esthesioneuroblastomas, including advanced-stage tumors or Kadish stage C, with endoscopy by debulking the intranasal portion of the tumor to provide visualization of the margins and to assess the extent of disease, said Dr. Snyderman. The area of skull base involvement (dura and olfactory tracts) can then be removed in an en bloc fashion. This approach can be successful if the surgeon achieves clear margins and adheres to oncologic principals for removing the malignancy, he said.
The ability to achieve widely negative margins is fairly limited for both endoscopic and open craniofacial resection due to the presence of the orbits, optic nerves, dura, and brain, said Dr. Kraus. Complete tumor resection allows for narrow microscopically negative margins with radiation being employed in a majority of patients to address the risk of microscopic residual disease, he added.
 The treatment needs to be individualized to the patient and, candidly, to the ability of the surgeon.
The treatment needs to be individualized to the patient and, candidly, to the ability of the surgeon.
-Dennis Kraus, MD
More Research Needed
Although endoscopy holds promise, more data are needed to support the contention that its oncologic results, morbidity, and mortality are as good as those for open surgery, said Dr. Kraus. Most studies are in small groups of patients, and long-term follow-up data comparing it with open surgery are not yet available, he said.
Most otolaryngologists-head and neck surgeons want to see the efficacy of endoscopy proven via cure rates rather than what might be technically feasible, noted Dr. Osguthorpe. So far, sufficient data do not exist to resolve the controversy surrounding the treatment of malignant sinonasal tumors, he said.
Additionally, one major caveat to keep in mind when evaluating available data is that many studies of endoscopic procedures are performed in conjunction with open surgery or radiation, said Dr. Osguthorpe, so separating endoscopic-alone from endoscopically-assisted is critical. The titles of some publications do not make this distinction, he added.
 Pete Batra, MD, said that not every tumor is best managed by an only an endoscopic or an open approach. Surgeons may opt to combine the two techniques to remove tumors.
Pete Batra, MD, said that not every tumor is best managed by an only an endoscopic or an open approach. Surgeons may opt to combine the two techniques to remove tumors.In one small study (Am J Rhinol 2005; 19(5):521-8), Dr. Batra and his colleagues found no significant differences in operative time, estimated blood loss, or hospital stay between a group of nine patients managed with a minimally invasive endoscopic resection of anterior skull base tumors and a group of 16 patients treated with traditional craniofacial resection.
Major complications were encountered in 22% and 44% of the patients in the endoscopic and open surgery groups, respectively. Thirty-three percent of patients who had undergone endoscopy and 36% of those in the open surgery group experienced disease recurrence. Mortality rates were 0% and 27% in the endoscopic and open groups, respectively.
Additionally, Dr. Snyderman and his colleagues have published data on endoscopic resection of esthesioneuroblastoma (Am J Rhinol 2009;23:91-4). The problem is we don’t have long follow-up, so no one can say it’s better than traditional surgery yet, but early data are encouraging, he observed.
In this study, 19 patients underwent primary endoscopic endonasal anterior skull base resection. Complete resection and negative intraoperative resection margins were achieved endoscopically in 17 individuals. Of the two other cases, one patient required a craniotomy to complete the resection of a positive lateral dual margin, and the other patient had positive margins at the orbital apex. All patients tolerated the endoscopic procedure, and there were four cerebrospinal fluid (CSF) leaks. All cases were disease-free at the most recent available follow-up.
Open surgery to treat esthesioneuroblastomas has already been shown to have an impressive disease-free survival, noted Dr. Osguthorpe. Specifically, in a study by Levine et al (Arch Otolaryngol Head Neck Surg 2006;132:134-8), 50 patients with esthesioneuroblastoma were treated with a standardized protocol during a 28-year period. Patients with Kadish A or B disease underwent preoperative radiotherapy followed by craniofacial resection. Those with stage C disease received preoperative sequential chemotherapy and radiotherapy followed by a craniofacial resection. The disease-free survival was 86.5% at five years and 82.6% at 15 years.
During the recent Ogura lecture, Dr. Levine noted that 60 patients have now been treated, and that the 20-year disease specific survival is 81.2%.
In other recent research supporting the use of endoscopy, a 10-year retrospective analysis (Nicolai P et al. Am J Rhinol 2008; 22:308-16) evaluated 184 patients with nasoethmoidal malignancies possibly involving the adjacent skull base. Of these, 134 were treated with an exclusive endoscopic approach (EEA) and 50 were treated with a cranioendoscopic approach (CEA).
Researchers found that the five-year disease-specific survival was 91.4% for the EEA group and 58.8% for CEA patients, respectively, indicating that endoscopic surgery, when properly planned and in expert hands, may be a valid alternative to standard surgical approaches for the management of malignancies of the sinonasal tract.
Additionally, in a prospective cohort study (Lund V et al. Am J Rhinol 2007;21: 89-94), 49 patients underwent an endoscopic resection as an alternative to craniofacial resection for pathologies including adenocarcinoma, malignant melanomas, and olfactory neuroblastomas. Thirty-seven patients received radiotherapy and 14 received adjuvant chemotherapy.
The overall survival of patients was 88% at five years. Mean hospital stay was five days, with no significant postoperative complications. Thirty-six patients were alive and well at follow-up (a mean of 36 months), seven had residual disease, and six patients had died. Three patients were converted to craniofacial resection. Researchers concluded that endoscopic resection may provide an alternative to craniofacial resection in selected cases of sinonasal malignancy.
Benefits of Endoscopy
Despite the debate surrounding endoscopy and the lack of long-term research, most physicians can agree that the technology has a number of potential benefits.
An endoscopic approach results in less morbidity for the patient, less manipulation of the brain tissue, and faster and easier recovery compared with open surgery, said Dr. Snyderman.
Additionally, patients may have better cosmetic results because endoscopy avoids facial incisions, said Dr. Batra. However, even though endoscopic surgery can facilitate a quicker recovery and reduce complications, it shouldn’t be viewed as a panacea, he said.
The benefits of endoscopy, or any other approach, open surgical or otherwise, are irrelevant if the tumor isn’t fully controlled, cautioned Dr. Osguthorpe.
Risks of Endoscopy
One of the biggest challenges that exists with endoscopic resection is the ability to reconstruct the dura in patients undergoing resection intracranial extension, including involvement of the dura and the brain, said Dr. Kraus.
With tissue flap repair, the risk of CSF leaks during endoscopic surgery is now comparable to traditional techniques, noted Dr. Snyderman. In a consecutive series of 150 patients undergoing endoscopic skull base surgery with septal mucosal flap reconstruction, the incidence of a postoperative CSF leak was 4%, he said, citing unpublished data.
One important element to preventing CSF leaks during minimally invasive resection is separating the intracranial and sinonasal components with multilayered skull base reconstruction, said Dr. Batra.
Pedicled nasoseptal flap based on the posterior septal artery has been described (Hadad G et al. Laryngoscope 2006;116: 1882-6) as an alternative to the traditional multilayered reconstruction, noted Dr. Batra.
In research of Dr. Batra’s that has not yet been published, he and his colleagues observed a CSF leak rate of 6.5% with the multilayered approach in patients with anterior skull base tumors. These two persistent leaks resolved with lumbar drainage without need for additional surgery.
The decision of lumbar drain placement for CSF leak management is done on a case-by-case basis, explained Dr. Batra. In his series of patients, only 25% required lumbar drains, helping the remaining 75% avoid drains and their associated morbidity.
In addition to CSF leaks, the risks of endoscopy are similar to those of open surgery and include bleeding and damage to vision or the brain, said Dr. Osguthorpe, but such risks tend to diminish with endoscopic approaches to early-stage lesions, as fewer soft tissues are disrupted with the approach.
Spilling tumor cells that could potentially implant in sinonasal tissue is a theoretical concern of endoscopic procedures that remove malignancies a little at a time, noted Dr. Snyderman.
However, most tumors hang down into the nasal cavity, so physicians are rarely at risk of violating healthy tissue when they remove the malignancy, he said.
In more than 10 years of performing endoscopic resections of sinonasal malignancies, Dr. Snyderman hasn’t seen any cancer implants attributable to endoscopic techniques.
Necessary Expertise
To avoid associated risks, minimally invasive endoscopic resection of sinonasal malignancies needs to be performed by physicians with endoscopy training as well as a background in head and neck surgery, noted Dr. Snyderman. They need to be able to get all the cancer out and not rely on other therapies such as radiation to mop up afterward, he said.
Endoscopic surgeons performing resection of sinonasal tumors require formal training in head and neck oncology and supporting disciplines, said Dr. Kraus. Working with a neurosurgeon who is experienced with an endoscope is also beneficial, he added.
Moreover, having pathologists on staff who understand the variety of sinonasal tumors so an exact diagnosis can be made is critical, said Dr. Batra. Endoscopy and CT scan of the sinuses are paramount to delineate the extent of the tumor. Many cases require an MRI because of its ability to delineate soft tissue involvement at the skull base and orbital interfaces, he said. PET scan allows for detection of regional and distant disease, he said.
Weighing the Options
Certainly, in some circumstances, an open operation will make more sense than endoscopy, said Dr. Snyderman, adding that specific areas of the head and neck are difficult to access endoscopically. Coming up the front of the skull is especially hard to visualize with an endoscope inserted through the nose, he said. Additionally, if a malignancy is big and growing into superficial tissues or is invading the eye, an open approach may be more practical, he said.
However, tumor size rarely makes a difference as to whether the surgeon needs to use an open or endoscopic approach, said Dr. Snyderman.
Tumor size is not a contraindication to an endoscopic approach, agreed Dr. Batra. Tumors can be bulky and still be removed via endoscopy, he said.
However, patients with extensive dural or brain involvement or involvement over the lateral orbit will likely require a bifrontal or subfrontal craniotomy to clear the superior margin, said Dr. Batra. Additionally, patients with involvement of the facial soft tissues, extensive lacrimal pathway infiltration, or anterior table of frontal sinus may be better served by the open approach, he said.
Not every tumor is best managed by an only an endoscopic or an open approach, said Dr. Batra. Surgeons may opt to combine the two techniques to remove tumors, he said. Some surgeons will also perform an open procedure then put the endoscope in to look at the results or to biopsy residual tissue, he added.
Additionally, to avoid facial incisions, surgeons may choose to use endoscopy to resect the intranasal portion of the tumor and perform a craniotomy if the cancer has spread to the intracranial region, noted Dr. Kraus.
Individualized Treatment the Bottom Line
Because all patients, surgeons, and tumors are different, treatment ultimately needs to be individualized, said Dr. Batra.
Dr. Batra and his colleagues present their cases of malignant sinonasal tumors to a tumor board consisting of endoscopic and traditional head and neck surgeons, radiation oncologists, and medical oncologists to best formulate a treatment plan.
Overall, the treatment needs to be individualized to the patient and, candidly, to the ability of the surgeon, concluded Dr. Kraus.
©2009 The Triological Society
Leave a Reply