
In 1978, Richard T. Miyamoto, MD, received a phone call from his former mentor, William F. House, MD. Dr. Miyamoto had just completed his fellowship in neurotology and had moved to Indiana University’s Riley Hospital for Children as an assistant professor. Dr. House was calling to ask his former trainee to join a new multi-center clinical trial of cochlear implants. Dr. Miyamoto immediately agreed to join the study and traveled with his first patient to House Ear Institute (HEI) to complete the surgery. “I was the youngest co-investigator in that group,” Dr. Miyamoto said. “Most of the experts in hearing science were very down on implants in those early days. They felt that success was unobtainable. But there wasn’t any treatment for sensorineural deafness at the time and, during my fellowship at House Ear Institute, I had seen that this technology was life changing for patients.”
The results of that trial, concluding that CIs were beneficial to patients, helped dispel some of the controversy sparked in the scientific community. By 1984, the U.S. Food and Drug Administration had approved the 3M/House single-channel cochlear implant. Many, including Dr. Miyamoto and John W. House, MD, president of House Research Institute and clinical professor in the department of otolaryngology at the University of Southern California, credit the late William House as the father of neurotology and as instrumental in the development and acceptance of cochlear implants. Dr. House died on December 7, 2012, at the age of 89 at his home in Aurora, Ore. “We are all grateful for his pioneering work, and he will be missed,” said Dr. John House, who is also Dr. William House’s nephew.
Since 1984, cochlear implant technology has followed a fairly rapid trajectory, fed by advancements from investigators around the world. By 2010, according to the FDA, more than 219,000 patients worldwide had received cochlear implants. In the U.S., where Advanced Bionics, Cochlear Americas and MED-EL devices are FDA approved, that figure stands at 42,600—28,400 of these implanted in children.

“Like Boiling Soup”
The roots of cochlear implant technology go back more than 200 years, said Dr. John House. In the 1790s, Alessandro Volta, who developed the electric battery, placed metal probes into his own ears and connected them to a 50-volt circuit. Upon switching on the flow of current, he experienced a jolt but, more importantly for auditory science, he also heard a noise, which he noted was akin to the sound of boiling soup.
Others also experimented with stimulation of the cochlea. In 1865, Duchenne de Boulogne reported a buzzing and ringing sensation, achieved by using alternating current. Much later, in the 1930s, Ernest Glen Wever, a Princeton University psychology professor, worked with Charles Bray during an otological research fellowship at Johns Hopkins Medical Center in Baltimore to record electrical potentials in the cochlea that paralleled sound stimulus waveform. This work suggested the possibility that replicating those potentials could restore hearing.
In the second half of the 20th century, the work of neurophysiologist André Djourno and surgeon Charles Eyriès powered new interest in the direct stimulation of the auditory nervous system. While re-operating on a patient with recurring ear problems, Eyriès placed an electrode designed by Djourno on the stump of the patient’s auditory nerve. An induction coil with a return electrode was placed into the temporalis muscle. Post-operatively, the patient detected different sound intensities and small closed sets of spoken words. After that device and a second one failed, Eyriès refused to implant other patients, but the pair reported their findings in the French medical journal La Press Medicale. When the Los Angeles Times picked up the story, one of Dr. House’s patients read it and brought it to his attention (Anat Record. 2012;295:1967-1980).
The reports stimulated Dr. House to begin work on an auditory prosthesis. In 1961, he teamed with neurosurgeon John Doyle, MD, to place single-electrode gold implants in a few patients. These patients could identify words in small closed sets, but electrode rejection and fear of infection intervened.
In the mid-1960s, Stanford’s Blair Simmons, MD, then associate professor in the division of surgery (otolaryngology), implanted a six-channel device that used a percutaneous plug to enable stimulation of individual electrodes and was able to demonstrate that stimulating different areas of the cochlea could produce different pitch perceptions.
Robert V. Shannon, PhD, a research professor with USC Biomedical Engineering and director of the division of communication and auditory neuroscience at House Research Institute, noted that hermetic sealing technology, which was originally developed for the space program and later adapted by pacemaker companies, solved a major problem in CI technology. “Without a good hermetic seal, any implanted electronics only lasted a few months before leaking body fluids and shorting out.” Improvements in pacemaker technology spurred Dr. House to pursue development of a biocompatible CI. Starting in 1967, he partnered with engineer Jack Urban to produce the first hardwire five-electrode system and placed implants in three patients.
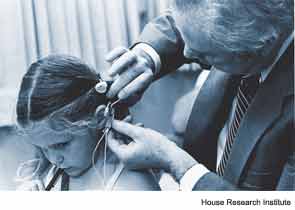
The Fruitful 1970s
Major advances were made in the 1970s, and three of the top investigators were located in California, said Dr. John House. Robin Michelson, MD, working at the University of California San Francisco (UCSF), was also forging ahead, collaborating with C. Robert Pettit, MD, neurophysiologist Michael Merzenich, PhD, and later Storz electrical engineer Mel Bartz, to develop a gold two-electrode system. At the House Ear Institute, Dr. William House and his collaborators produced the first wearable device and the first induction system, featuring a centering coil and an attaching magnet, in 1972.
The multi-electrode strategy gained prominence in the early 1970s due to the work of French otologist Claude-Henri Chouard with the Institut National de la Sante’ et de la Recherche Scientifique in Paris, who had been a student of Eyriès. In 1973, he devised a procedure to implant electrodes through 12 separate openings into the cochlea, thus exploiting the pitch particularity of each section of the hair cell-lined cochlea. In Melbourne, Australia, a team led by Graeme Clark was also working through the 1970s, developing a multi-channel prototype with an array of 20 electrodes; their first successful implantation took place in 1978. Yet another group, working in Vienna, designed and manufactured a passive single-channel broadband analog implant. The Australian efforts coalesced into Cochlear Ltd.; the Austrians’ work became today’s MED-EL.
Scientific Community Pushback
All of this activity resulted in the First International Conference on Electrical Stimulation of the Acoustic Nerve, held in 1974 at UCSF. Investigators on teams from institutions such as HEI, Stanford and UCSF had been collecting evidence on film of their patients perceiving sound for the first time. Still, many in the scientific community were not convinced of the efficacy of implantation, including Harold Schuknecht, MD, chief of otolaryngology at Massachusetts Eye and Ear Infirmary in Boston, who said at the conference: “I interpreted the movies and the case presentations to confirm my suspicion that the prostheses as they are now designed are of very little use.”
Dr. William House was undeterred, and in 1977 devised a new strategy to bring CIs to market. He told Dr. Miyamoto, “The scientists won’t listen to us, but if something good happens for patients, they’re going to have to listen to them.” He hoped the multi-center study would provide definitive proof that patients were benefitting from the procedure. Dr. Miyamoto agreed with this concept.
“Patients [with early implants] kept doing better than they should have,” he recalled. “The signal from the early implants was pretty elementary. But what no one took into account in those early days is that there was a brain at the other end of that signal.” As an academic researcher, Dr. Miyamoto was asked by 3M (which had bought the proprietary rights to the House implant) to present evidence to the FDA, which until this time had never approved a durable medical device. The FDA later used Dr. Miyamoto as a consultant to help generate testing benchmarks for device approval. (He was a member of the FDA committee but did not participate in the final FDA approval of cochlear implants, to prevent any perceived conflict of interest.)
In the meantime, at his institution, Dr. Miyamoto was building a multidisciplinary team of investigators, which included speech scientists and neuroscientists. Earleen Elkins, PhD, director of the National Institutes of Health’s (NIH) hearing portfolio, approached Dr. Miyamoto, asking him to submit a grant proposal to the NIH demonstrating the safety and efficacy of the implants. The safety issues, especially those surrounding the implantation surgery, were quickly resolved, said Dr. Miyamoto. Showing efficacy was another issue entirely. “We spent quite a bit of our early time just working out test measures and ways to assess deaf patients,” he explained. “We weren’t making them normal, so we could not use regular tests of hearing. We had to establish early baselines ourselves to show that implants made a difference. Every time we got an answer, it brought up 10 new questions.”
Dr. Miyamoto’s cochlear implant laboratory has received NIH funding continuously for 25 years now. “So it was a project that never ended, and it’s continuing to go that way,” he said.
In 1979, while a senior resident at the University of Iowa Medical School, Bruce J. Gantz, MD, now head of the department of otolaryngology-head and neck surgery at the University of Iowa Hospitals and Clinics, met and trained with William House. In early 1981, Dr. Gantz performed the first cochlear implant at his institution, and between 1982 and 1983, he interacted with other key CI pioneers, including Dr. Simmons, Ingeborg and Erwin Hochmair in Vienna, Dr. Chouard in Paris and Graeme Clark in Australia. Dr. Gantz’s vision was to establish the University of Iowa as a center for testing different devices, and his department has received continuous NIH funding since that time.
In Rapid Succession
After the FDA’s first approval of the single-channel implant for adults, others quickly followed: The multiple-channel implant was approved for adults in 1987, and a multiple-channel implant was approved for children in 1990. The initial age for children was 2 years, then 18 months in 1998 and 12 months in 2000.
Dr. Shannon noted that the improvements in CI performance in the 1990s were due to advances in understanding brain processing. “Although implants worked well in the 1980s, improvements came when we ‘got out of the way’ and stopped ‘pre-processing’ the signal to pull out the important parts and presented the raw speech signals to the multiple electrodes. The brain, trained over millions of words over a lifetime, is far better at picking out the most important parts of the signal.”
The Future Looks Bright
As manufacturers’ devices become more and more sophisticated (for example, the waterproof Neptune processor manufactured by Advanced Bionics allows users to go swimming), investigators continue to push the boundaries. Current thrusts of research include implantation in very young infants, timing of bilateral implantation, preservation of residual hearing structures and stem cell research. Dr. Miyamoto’s laboratory has just received approval from the FDA to study CIs in infants aged six months to 1 year. In many European countries, especially in Italy, investigators are placing implants in infants as young as three months (See “Cochlear Implants: How Young is Too Young?”).
Currently, the FDA allows implantation in infants at 1 year, but what we now know about brain plasticity in developing infants has led some researchers to conclude that earlier implantation results in better outcomes for children. The six-center
Childhood Development after Cochlear Implantation (CDaCI) Study, led by John Niparko, MD, at Johns Hopkins School of Medicine in Baltimore, was initiated in 2002 to systematically evaluate early cochlear implant outcomes in children. “We were trying to empower families with the strength of prediction and wanted them to know the realistic expectations of withholding cochlear implants until age 3,” said Dr. Niparko. Between 2002 and 2004, investigators enrolled 188 children with profound sensorineural hearing loss who underwent CI implantation, and 97 children with normal hearing.
Extensive baseline assessments and thorough follow-up as the children age are yielding not only observations about language acquisition but also valuable insight into the effects of environmental factors on CI outcomes (JAMA. 2010;303:1498-1506). This is especially important, said Drew Horlbeck, MD, of the division of otolaryngology at Nemours Children’s Clinic in Jacksonville, Fla., because the “real work” starts after placement and programming of the implant. “The important thing with an implant isn’t so much the surgery,” he said, “but the rehab afterwards.” The CDaCI investigators are finding, for instance, that higher socioeconomic status and higher parent-child interactions are associated with greater rates of improvement in comprehension and expression, said Dr. Niparko. Dr. Horlbeck, who trained with Dr. Niparko and has been doing implants since 1999, noted that the comprehensive rehabilitation team at Nemours contributes to the overall success of the program.
Dr. Gantz maintains that there need not be a sense of urgency to implant children prior to the age of eight months, the age when a behavioral audiogram can be performed. Based on 25 years of longitudinal follow-up on children receiving CIs at his institution, he has found that at age 7 years, children who had received implants between the ages of 2 and 4 years did not show significantly different reading, language and speech perception from those who received the implants between 11 months and 2 years of age.” If you implant an infant who might have some low frequency residual hearing, you are destroying it, and that could be very useful to preserve,” he said. “The residual low frequency acoustic hearing might assist the individual to hear better in noisy environments and to appreciate music in the future.”
Adrien A. Eshraghi, MD, associate professor and chief at Jackson Memorial Otology and Neurotology Clinics and director of the University of Miami Hearing Research Laboratory, department of otolaryngology, University of Miami Miller School of Medicine, and colleagues established that the implantation procedure itself can induce apoptosis, thus impeding reestablishment of residual hearing in damaged cochlear structures. Although manufacturers have worked to make coils that are less traumatic, Dr. Eshraghi pointed out that insertion of the CI electrode into the cochlea stimulates the production of inflammatory cytokines and oxidative stress, resulting in irreversible damage. His laboratory, in collaboration with microbiologist Thomas R. van de Water, PhD, professor and director of the Cochlear Implant Research Program at the University of Miami, is now working to better understand apoptosis post-implantation and to develop drug delivery strategies to prevent the problem. By reducing implantation trauma, he said, “you may be able to use electric acoustic stimulation with a hybrid device, or possibly even use the patient’s residual hearing.”

Leave a Reply