TRIO How I Do It articles are reviews from The Laryngoscope designed to provide guidance on clinical and surgical techniques and practice issues from experts in the field.
Explore This Issue
November 2020Introduction
Congenital ear anomalies can be classified in several ways, based on pathogenesis, extent of missing or misshapen tissue, or syndrome association. Malformations are the result of errors during embryogenesis that affect the development of the ultimate structure (Clin Pediatr. 2019;58:798-805). Anomalies may also be the result of a deformation that is an extrinsic factor, such as a mechanical force in utero, that restricts the growth of an organ (Ibid.). Congenital ear anomalies that are the result of contour irregularities with a normal, or near normal, amount of cartilage (unlike in microtia) fall into frequently seen patterns with descriptors matching the observed shape (Ibid.).
A spectrum of otoplasty techniques—including suturing, cartilage modifications, and cartilage grafting—can address congenital auricular anomalies with significant contour improvements. Although often successful, surgical risks include scarring/keloid formation, infection, hematoma, recurrence of the original deformity, and an unnatural-appearing result (Ibid.). Surgical correction is often performed at school age, when the ear has reached near-adult dimensions. By this time, the child may already have experienced psychological stress associated with the noticeable deformity (Ibid.).
Ear molding is a nonsurgical, safe, effective, and cost-efficient option for the correction of congenital ear deformities during infancy. The technique involves splinting of the ear into its ideal anatomic shape, taking advantage of the malleable properties of neonatal ear cartilage.
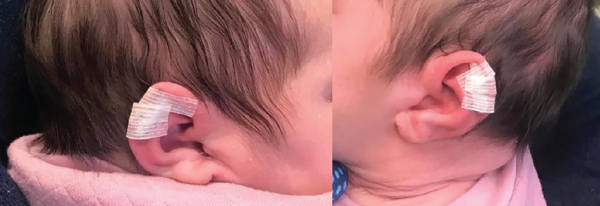
Normal auricular anatomy recreated with application of Steri-Strips.
Methods
The patient presented at 13 days old, referred by her pediatrician for bilateral congenital ear anomalies. The history was negative for any prenatal health problems. There were no complications during spontaneous vaginal delivery. The patient passed her newborn hearing screening, and there was no family history of congenital ear anomalies.
The examination of the ears showed flattening of the middle third of the helical rim and widening of the scaphoid fossae. There were no deficiencies of the auricular cartilage, skin, or soft tissue bilaterally. The external auditory canals and tympanic membranes were normal. The remainder of the physical exam was unremarkable.
Ear molding is a nonsurgical, safe, effective, and cost-efficient option for the correction of congenital ear deformities during infancy.
The option of ear molding was presented with a discussion of the time-sensitive nature of treatment initiation, and possible need for additional procedures in the future. For both ears, the normal curvature of the helix and the concavity of the scaphoid fossae were recreated by folding the helix into its normal anatomical location. Quarter-inch Steri-Strips (3M, St. Paul, Minn.) were used to create a roll placed into the scaphoid fossa and under the helical rim. Steri-Strips were applied to the postauricular surface of the scaphoid fossa, extending over the helical rim to the antihelix to secure the roll. We instructed the family about taping techniques and reapplication of the roll and tapes should they become loose.