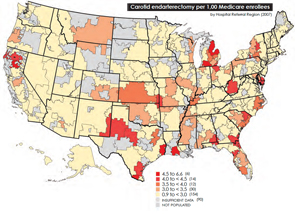
Medicare Battle Heats Up: Geographic Disparities spark look into spending variation
In the wake of this year’s landmark health care reform legislation, one of the most hotly debated topics comes courtesy of the Dartmouth Atlas of Health Care, as politicians, analysts, researchers and physicians grapple over how to resolve the contentious issue of geographical disparities in health care spending.




