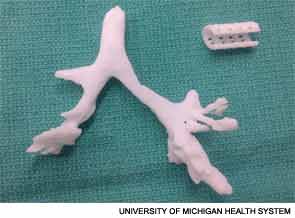
Armed with CT images of the child’s airway, they fashioned the stent according to a bellowed typology design, so that it resembled a tiny vacuum cleaner hose, flexible but sturdy (see image, right) Unlike stem cell-derived tracheas that have also been in the news, “this design specifically does not collapse,” said Dr. Green. “This enhances its applicability. The stent puts the patient’s natural trachea into the correct position, rather than replacing the patient’s tissues with tissue derived from stem cells.” The stent was placed around the collapsed portion of Kaiba’s left bronchus and sutured in place. Although the surgery occurred in February 2012, it was not announced to the general public until last month.
Explore This Issue
July 2013The procedure was not without its risks. Kaiba had multiple comorbidities and “was not the perfect candidate,” said Dr. Green. “But his life was dependent upon it. He was still coding, even with a tracheostomy and mechanical ventilation. It was just a matter of weeks.” Today, he is doing “fabulously,” he said. “He’s had no episodes of cyanosis since the surgery, and he has a normal life expectancy.”
Creating an Ear
Dr. Spector, who specializes in plastic and reconstructive surgery, and his colleagues are using 3D printing to make external ears that capture the biomechanical properties of normal human ears. Their goal is to provide a cosmetically and physiologically sound option for children with microtia.
They use a special 3D camera to gather the original source data, with the child’s opposite ear as a model. This step takes about 30 seconds. “Once the data are obtained and put into the work station, they are manipulated until we have a three-dimensional or digitized rendering of the ear. We then use that information to build the actual 3D replica of the ear,” Dr. Spector said. Their “ink” is a collagen hydrogel seeded with bovine auricular chondrocytes (see images).
This work is still experimental, but in a recent study they compared the cellular prototypes with ears developed from the collagen hydrogel alone, with no added chondrocytes (PLOS ONE. 2013;8:e56506). Ears of each type were implanted subcutaneously on the backs of nude rats. Within one month, the acellular constructs had deteriorated significantly compared with the cell-seeded ears, which retained their size and shape. The differences were even more striking at three months, and the cell-seeded ears had the same biomechanical properties as native auricular cartilage (see image, left).
Leave a Reply