Explore This Issue
July 2013Knowledge is power, an aphorism usually cited in politics and war, can now be applied to the pre-operative diagnosis of midline neck masses in children. In the largest study of its kind to date, researchers have identified three ultrasound features that have 100 percent positive predictive value (PPV) in predicting the presence of thyroglossal duct cysts (TGDCs) over dermoid cysts—two masses that often mimic each other, complicating pre-operative planning and family counseling.
The research, presented by Dupe Oyewumi, MD, an otolaryngology–head and neck surgery resident at The Hospital for Sick Children, University of Toronto at the 2013 annual meeting of the American Society of Pediatric Otolaryngology held April 25-28 in Arlington, Va., was based on a search of pathology reports from 2005 to 2012 that yielded 91 patients who were confirmed post-operatively to have either a TGDC or midline dermoid cyst (53 were TGCD and 38 were dermoid cysts). For the purposes of the study, ultrasound images that had been obtained pre-operatively were given to two radiologists (clinical fellow Emilio Inarejos, MD, and staff supervisor Mary-Louise Greer, MD, both with The Hospital for Sick Children in Toronto) who were blinded to the pathology results.
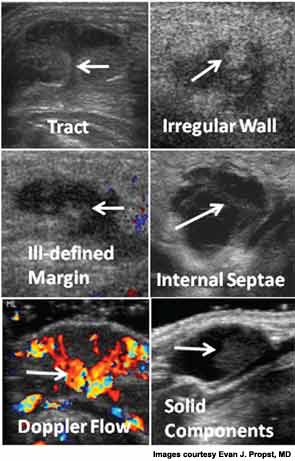
The radiologists were then asked to evaluate the images for 14 different features. According to senior author Evan J. Propst, MD, assistant professor in the department of otolaryngology-head and neck surgery at the University of Toronto and associate surgeon at The Hospital for Sick Children, six of those features were found to have high PPV scores for being TGDC:
- presence of a tract (100 percent PPV; P<0.01);
- irregular wall (100 percent; P<0.01);
- ill-defined margin (100 percent; P<0.05);
- internal septae (91 percent; P<0.02);
- intralesional doppler flow (91 percent; P<0.01); and
- solid components (81 percent; P<0.001).
Having a near-certain pre-operative diagnosis for a midline mass yields multiple benefits, Dr. Propst told ENTtoday. Surgery can be scheduled with greater accuracy, for example—a big plus, because removing a TGDC can take up to two hours, versus 30 minutes for a dermoid cyst, he said. Knowing what type of mass is present also makes counseling parents on what to expect and obtaining their consent much easier, he noted.
Moreover, the longer, more extensive surgery for removing a TGDC (Sistrunk procedure) can be avoided in many cases, said Dr. Propst. He explained that because dermoid cysts and TGDCs are often difficult to distinguish, both on ultrasound and pre-operatively based on physical findings, “some surgeons just do a Sistrunk to cover the bases.” The justification, he noted, is that such an approach will reduce the rate of recurrent disease. “Even if they are fairly certain that it’s a dermoid, some surgeons will still do a Sistrunk because they don’t want to see the mass recur.”
There are several problems with such an overly aggressive approach, Dr. Propst said. First and foremost, the amount of tissue being removed during a Sistrunk is far more extensive than that removed for a dermoid cyst, due to the location of the mass. Furthermore, patients who undergo a Sistrunk often require a postop drain, Dr. Probst added.
Mary Beth Cunnane, MD, a staff radiologist at the Massachusetts Eye and Ear Infirmary and an instructor at Harvard Medical School, both in Boston, said the study findings are potentially practice changing. “Like most of my colleagues, I’ve often struggled with making a differential diagnosis of these masses using ultrasound images,” Dr. Cunnane, who was not involved in the study, told ENTtoday. “Now, using these ultrasound features, I can be much more definitive in my radiology reports. I certainly plan on using this in my practice.”
Clues to Drainage
Leila Mankarious, MD, a pediatric otolaryngologist at Massachusetts Eye and Ear Infirmary, has conducted studies into why patients who undergo a Sistrunk procedure sometimes develop post-operative cervical fluid accumulations (Otolaryngol Head Neck Surg. 2009;140:343-347; 2011;144:888-890). Among her findings is the fact that salivary tissue is often present several milimeters above the hyoid bone.
“That finding was significant because the surgeon may believe he or she is doing a more thorough operative procedure by removing tissue above the hyoid bone, but actually may be disrupting salivary tissue that induces post-operative fluid accumulation,” said Nancy M. Bauman, MD, professor of otolaryngology-head and neck surgery at Children’s National Medical Center in Washington, DC, and an ENTtoday editorial advisory board member. “The treatment of post-operative fluid can be tedious for both the surgeon and family, not only because of discomfort but because it makes one wonder if the TGDC was not completely excised,” Dr. Bauman said. “Dr. Mankarious’ research suggests that it may not be residual TGDC that’s the culprit, but instead disrupted salivary tissue that is causing the fluid accumulation.”
But whatever the cause, the take-home message is clear, said Dr. Bauman. “More accurate pre-operative diagnosis will obviate the need to do a Sistrunk procedure on every midline neck mass.”
Dr. Propst shares Dr. Bauman’s concerns that applying the Sistrunk procedure too broadly has several downsides. “We actually put our TGDC patients in an observation bed because of the risk that they may develop swelling of the tongue, which needs to be watched closely,” he said. “This really complicates post-op care.” Thus, “it would be a huge benefit if we could limit those more extensive excisions to cases where we really are nearly 100 percent certain that a TGDC is in fact a TGDC, and not a dermoid cyst in disguise.”
A 2006 report in Seminars in Pediatric Surgery suggests that such masquerading is not uncommon, in part because dermoid cysts, which account for about 25 percent of all midline cervical abnormalities, often occur in the same midline neck region as TGDCs (Semin Pediatr Surg. 2006;15:70-75). Thus, location alone, assessed pre-operatively by surgeons, is a poor diagnostic indicator; hence, the use of pre-operative ultrasound.
Unfortunately, if ultrasound characteristics such as the ones identified by Dr. Propst are not factored in, the imaging modality has proven flawed at best. In a retrospective study coauthored by Nina L. Shapiro, MD, the director of pediatric otolaryngology at the University of California, Los Angeles School of Medicine, pre-operative ultrasound tests in 40 patients with midline neck masses were compared with pathologic results of tissue from the removed mass. The study showed a poor correlation between the results of conventionally interpreted pre-operative ultrasonography (e.g., anechoic, homogenous cysts and pseudosolid, heterogenous masses) and pathology findings (Otolaryngol Head Neck Surg. 2011;144:431-434). The investigators concluded that “the diagnostic accuracy of this imaging modality [ultrasound] may have significant limitations.”
Asked to review the study conducted by Dr. Propst and colleagues, Dr. Shapiro commented that the Toronto researchers “clearly had similar concerns to ours, in that ultrasound findings associated with TGDCs have been notably inconsistent.” That inconsistency is due in part, she noted, to variations in how ultrasound is used to diagnose these masses from one institution to another. Thus, “establishing more widespread [pre-operative ultrasound] criteria may improve the accuracy of this imaging modality.” Such an advance, she agreed, would also help improve the pre-operative counseling of families whose children present with midline neck masses.
But Dr. Shapiro added one caveat. “One must not forget that clinical history, physical examination and intra-operative findings may, in the end, be superior to radiologic studies in these scenarios,” she said. “In our experience, no child underwent unnecessary Sistrunk procedure in the setting of an inflamed lymph node or dermoid/epidermoid cyst. The superficial nature of these lesions, location and gross intra-operative characteristics should point the surgeon in the right direction.”
Other Approaches, Another Fix
Not all pre-operative physical findings can be relied upon to nail down a diagnosis of TGDC or dermoid cyst. One common method that could be problematic is giving patients a swallowing test, according to the 2006 Seminars in Pediatric Surgery review article. If the midline mass in question moves when the patient swallows, then it is often thought to be a TGDC because only that particular mass involves the hyoid bone and the base of the tongue, which elevates during swallowing. But there’s a drawback to the test, the authors noted: It can be very difficult to get younger children to swallow while a physician tries to palpate the mass in question.
Three additional diagnostic and management techniques are often used in patients with midline neck masses, and they all have flaws, Dr. Propst noted. “Some surgeons stretch the skin over the cyst and if a white colored mass shows through, it is believed that it will more likely be a dermoid cust than TGDC,” he said. Unfortunately, this method has not proven reliable in the literature. “Others automatically do a Sistrunk for every cyst in the midline region. And a third way is to base your decision on the ultrasound report and do the appropriate surgery, but, as previous studies have shown, those reports can be wrong.”
Dr. Propst said he has been using a fourth technique to distinguish between TGDCs and dermoid cysts. During surgery, he said, he will minimally expose the cyst and then aspirate it with a needle. Whatever substance is removed tells him what type of cyst is present. “If it’s mucus, then it’s a TGDC; if it’s white and ‘cottage cheesy’ in appearance, then it’s a dermoid,” he said. This simple finding has a very high predictive value, Dr. Propst said, and thus helps him reduce the need for more extensive surgery than the patient requires. But it doesn’t solve the larger problem of needing to know definitively ahead of time what type of midline mass is present to help counsel parents and plan peri-operative management. For that, Dr. Propst’s new method for interpreting ultrasound findings is the best option. But is it ready for prime time?
“We have a bit more work to do in terms of reproducing our results, but I am very confident that this will ultimately make it into clinical practice,” Dr. Propst said. Part of that confidence, he noted, comes from the quality of the current study design. “What we ended up with was a prospective, blinded evaluation of retrospectively acquired ultrasound imaging; I don’t think this has been done before in these patients,” he said. Moreover, “no previous study has included as many patients as we did, to assess ultrasound’s ability to differentiate between these two masses.”
Dr. Cunnane agreed that more research is needed. Still, she stressed that the study by Dr. Propst and his colleagues “has more cases of its type than any other study I know of.” She also gave the researchers kudos for coupling ultrasound readings with pathology reports. “Overall, this is a very well-done study,” she said. “I look forward to their efforts at replicating the results in a prospective fashion.”
Leave a Reply