Part 2 of 2 articles
Explore This Issue
October 2009Cysts on vocal folds can be complicated lesions to manage: Postsurgical healing can be difficult to forecast, and the effects on the voice can also be difficult to determine until after surgery. Even determining whether a lesion is a cyst, a polyp, or a pseudocyst is often problematic. Panelists at the 89th Annual Meeting of the American Broncho-Esophagological Association presented several cases to illustrate the difficulties inherent in treating vocal fold cysts.
Case 1: Severe Glottal Closure
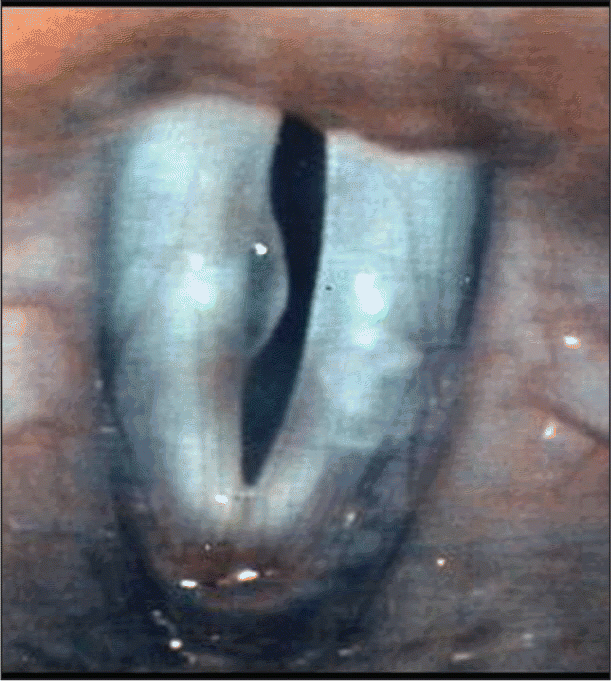
The first case discussed by the panelists involved a 35-year-old elementary school teacher with severe glottal closure symptoms. At the end of the day she had worse vocal fatigue, and by Thursday and Friday afternoons, she had almost no voice. She did not drink or smoke. During an examination, a lesion was found on her right vocal fold (see Figure 1).
The first problem was determining what kind of lesion it was. Michael Pitman, MD, Director of the Voice and Swallowing Institute at the New York Eye and Ear Infirmary, considered it a polyp-almost like a watery, edematous polyp, and I treat them as such.
I think they do sometimes have a chance of going away, especially in someone with a history like this, he said. This person, I think, I would really be put through the wringer in terms of therapy and a voice saver to use at school, and all the other things you can do before having her make the decision about surgery.
I don’t know what I’d call it, said Robert H. Ossoff, DMD, MD, Executive Medical Director of the Vanderbilt Voice Center in Nashville. What’s in a name?
But he did say, I don’t expect the lesion to go away with voice therapy. On the other hand, voice therapy is very helpful with these patients, because it does help them to alleviate some of the cofactors in creating an environment of laryngeal hygiene.
He said he would try to keep the patient able to function on the job as long as possible. My goal is, if I can get them through the week and they have the weekend to rest and they do fine that way, I keep them out of the operating room, he said. Eventually-and it varies in terms of the length of time-all of a sudden they won’t be able to recover over the weekend and it’s going to take a vacation. And then it’s going to take the summer. And then they don’t recover…. I don’t expect that they’re going to go away but I do think we can delay the inevitable surgery for a while and give them a chance to work with a therapist.
Gayle Woodson, MD, Chair of the Otolaryngology-Head and Neck Division at Southern Illinois University in Springfield, said that in cases in which patients have not been abusing their voices and have no history of voice problems, the lesion might be more likely to go away on its own, without surgery. I think the history of the patient makes some difference, she said.
Jamie A. Koufman, MD, Director of the Voice Institute of New York, who moderated the panel and presented the cases, said that she considered the lesion to be a pseudocyst, and not a polyp, because it was unilateral; associated with a bowed, hypomobile vocal fold; and seemed to be seen within that clinical constellation.
Dr. Koufman did remove the lesion, and the patient began voice therapy. After two and a half months, the patient started to develop a new lesion. Dr. Koufman then performed a bilateral medialization and reported, She’s been fine ever since.
I think a lot of these patients have glottal closure problems and that’s why they develop striking-zone pathology, she said.
Dr. Woodson asked how, without enough closure, there could be trauma that leads to the lesion. Her opinion, Dr. Koufman said, was that the strain on the laryngeal muscles from trying to achieve closure creates more severe shearing force. This will lead to injury on one side, which has the effect of protecting the other side, which continues to work and divert the air to the injured side. That, in turn, leads to more injury on the problem side.
It’s very similar to saloon doors, she said. If you were to take one of the wooden doors off and hang a bunch of balloons in its place, and blow air through there, the good door would never move again. The surface area of the injured, balloon side, would take all the heat. So I think that’s what happens.
Case 2: Recurrent Laryngitis
Another case involved a 45-year-old film producer who was otherwise healthy. She had had lifelong problems with recurrent laryngitis and had had a raspy voice since her school days. In the past year, her voice symptoms had gotten worse and become chronic. Her score on the glottal closure index was a dismal 20, the maximum score.
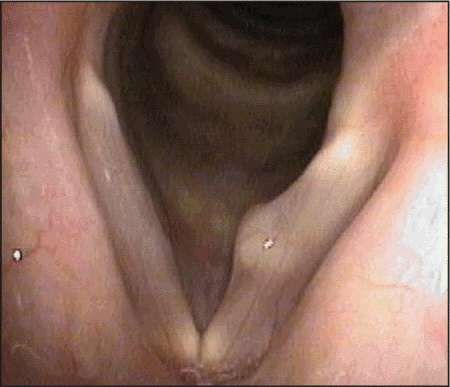
Everyone agreed that what was found on the right vocal fold was a keratin cyst-the real deal cyst, Dr. Koufman said (see Figure 2).
Dr. Ossoff said it might look like an easy procedure, but it probably wouldn’t be. It looks like it should come out easily, he said. It’s like shucking a clam or shucking an oyster. But when you do that there’s always a piece of flesh that stays on the shell and it doesn’t come out so easily. So don’t be seduced.
Dr. Koufman said she realized it was going to be a difficult case once she started the procedure. I realized it was really stuck there. I had just made a hole in it, and now it was decompressed and I had basically this huge fibrous nothing, she said. There was no subepithelial space. All there was was a scarred vocal fold, and digging it out would have just meant digging out all the scar, digging around in muscle. So I put a little deposteroid in it and quit.
I agree with that decision, Dr. Ossoff said. If you inadvertently get into it so early that you’re not going to be able to define it, I think it’s better to quit and start again another day than to try to do all this digging and leave things far worse than you found them.
Two months later, Dr. Koufman said, the patient developed polypoid changes on the good side.
Dr. Pitman said it is predictable that this will be a long road for the patient and that she should be prepared for that. She’s always had a bad voice, he said. When you see a cyst like that, even if everything goes perfectly, they’re still going to have a long recovery. He said it might be best to work on the area around the cyst to avoid a rupture at the very beginning of the procedure.
Dr. Koufman said the patient ended up with quite a good result but still has some polypoid changes.
Sometimes those polypoid changes actually aid the voice, Dr. Ossoff said. You have something to vibrate and that makes a huge difference. At first, I hated to see that but then I said, ‘That’s my helper.’
Case 3: Multiple Cysts
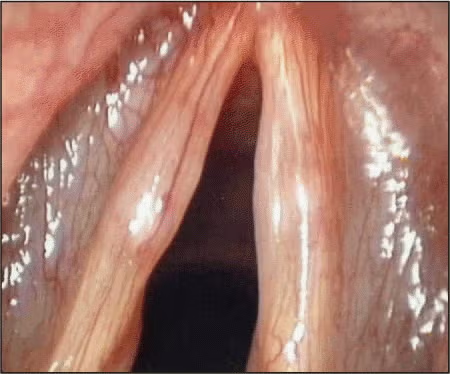
In another case, a 25-year-old businesswoman came to Dr. Koufman with glottal closure symptoms. One side was mostly cyst. On the other side was a partially removed, decompressed cyst (Figure 3). These are the ones I’ve agonized over, Dr. Koufman said.
Dr. Ossoff opined that waiting and evaluating is the best course. The best thing you can do is buy some time and not make a decision the first time that patient comes into the office, he said. You want to clean up the larynx, and that gives you some time.
He said he would put the patient on two weeks of voice rest with a tapering dose of steroids. That would eliminate some of the edema and give him a better view of the problem. These are tough cases, and you want to study them over time and see what happens, Dr. Ossoff said.
C. Blake Simpson, MD, Director of the University of Texas Voice Center in San Antonio, said he would prefer injecting steroids. I’ve had people who have cysts or ruptured cysts where I’ve tried injecting steroids into the vocal fold, he said. In particular, I’m thinking of a teacher. We got her through the semester doing that and actually never ended up taking off the lesion. So I think that’s worked fine. You’re not going to lose anything.
Dr. Koufman asked whether anyone had used a laser, but no one said they had. Dr. Koufman said that surprised her. It seems to help on some of these bad ones, she said. I would only try it in a case like this, where the patient has not a lot to gain from having a resection where you’re taking out most of what would otherwise have been vocal fold.
In this case, she said, she did remove the cyst and the scarring on both sides. Then she used lipoinjection to bulk up the vocal folds, and the patient ended up doing pretty well.
©2009 The Triological Society
Leave a Reply