There were different views on margins in these cases. Panelist Nilesh Vasan, MD, associate professor of otolaryngology-head and neck surgery at Oklahoma Health Sciences Center in Oklahoma City, said he likes to use the sutures as well, but prefers 1.5-cm margins—a study he worked on showed that this size margin resulted in a clear margin in 96% of cases.
Explore This Issue
November 2016In these cases, he acknowledged, sometimes a flap is needed to reconstruct. “We do have wide margins but oftentimes, depending on what the status of the neck is, they may not need any further adjuvant treatment,” he said. “I’ve never really worried about the defect. My job is to get that cancer out with clear margins.”
Dr. Deschler said he would be worried about “bringing in uninvolved tongue at either edge to get it around the back” and that he can often have patients leave with no perineural and no perivascular involvement and clear margins with more minimal morbidity.
TORS for Tonsillectomy and Neck Dissection
Jeremy Richmon, MD, director of head and neck surgery robotic surgery at Massachusetts Eye and Ear Infirmary in Boston, offered these suggestions for transoral robotic surgery for tonsillectomy and neck dissection:
- Never bury the tip. “As soon as the tip of your instrument is buried and you can’t see what it’s cutting into, there are going to be issues with bleeding.”
- Always perform a lot of blunt dissection when you’re looking for vessels.
- Make sure the incision isn’t too low, too high, or too small. “You don’t want to work in tunnels, especially cleaning out Level IIb.”
- Consider avoiding the marginal mandibular nerve. “For true level I neck dissection, it’s not necessary.”
- Dr. Richmon prefers not to use muscle relaxation. “I want to know whether that shoulder is being stimulated during the case.”
- Tension is critical when dissecting over the internal jugular vein. “The two areas of danger are high in the IJ and low, where you’re pulling the IJ over and could end up corkscrewing it, folding it on itself. So you have to identify the IJ high and low so you know where you’re dissecting and make sure you don’t accidentally nick that.”
Parotidectomy
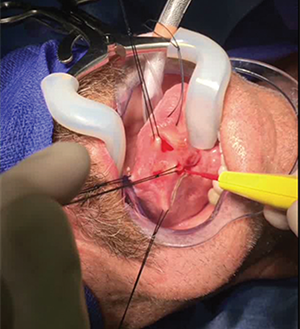
“Geppetto” technique for partial glossectomy.
© Courtesy Daniel Deschler, MD
Dr. Vasan offered these suggestions for parotidectomy in the case of a 60-year-old patient with bilateral masses:
- Generally, he suggested a fine needle aspiration for these lesions, but he agreed that if the analysis is done outside your own center and the accuracy rate is low, it could call into question whether the procedure is worth it.
- Preserve the greater auricular nerve, if possible, which it usually is if the lesion is benign and not massive.
- With your incision, don’t go all the way into the neck, but just anterior to the palpable mass. “You don’t have to make a really large incision,” he said.
- Make a lot of headway with the first incision. After that first cut, have your resident or assistant retract the tissue toward you rather than away from you, he said. “If you would just do all of those retractions toward the surgeon, the parotid is back into its normal anatomical shape,” he said. If the seventh cranial nerve is visible, you can divide a lot of tissue right away.
- Consider using a dermal fat graft on reconstruction. “A dermal fat graft actually gets quite long-term beneficial results.”
Dr. Deschler said that, in his experience, it’s possible to get good results without using a dermal fat graft, which is a very involved process.