With the advent of fiberoptic and distal-chip scopes and other innovations, otolaryngologists are now able to perform many laryngeal diagnostic and therapeutic procedures on awake patients in the in-office setting rather than on fully anesthetized individuals in the operating room. Different laryngoscope and camera technologies allow surgeons to more easily visualize the larynx and surrounding tissue.
 You need to take your time with topical anesthesia, and you need to let patients know everything you are going to do.
You need to take your time with topical anesthesia, and you need to let patients know everything you are going to do.-Greg Postma, MD
Due to the accessibility of the larynx and new technology, we’re able to perform a variety of procedures in the awake setting, said Adam Klein, MD, Assistant Professor in the Department of Otolaryngology and Emory Voice Center at the Emory University School of Medicine in Atlanta.
Simple biopsies, laser treatments, and injections are the most common in-office laryngeal procedures performed in awake patients, said Steven Zeitels, MD, the Eugene B. Casey Professor of Laryngeal Surgery at Harvard Medical School and the Director of the Center for Laryngeal Surgery and Voice Rehabilitation at Massachusetts General Hospital in Boston.
Diagnosis
To obtain a highly magnified visual assessment of the larynx, otolaryngologists may employ laryngeal videostroboscopy, which uses a strobe light and a specialized digital camera to visually capture individual oscillatory cycles of vocal folds, said Dr. Klein.
Physicians can also evaluate sensory functioning of the laryngopharynx in awake patients by performing functional endoscopic evaluation of swallowing and sensory testing, said Dr. Klein. This can be done utilizing liquids and food of different consistencies as well as puffs of air, he explained.
Airway conditions such as stenosis can also be evaluated with a flexible fiberoptic scope and distal-chip technology, noted Dr. Klein.
This technology also allows doctors to pass a local anesthetic and biopsy forceps through the mouth or nose and to take a tissue sample of the larynx, said Dr. Zeitels. This tissue sample will help pathologists determine whether the patient has cancer or dysplasia, he said.
Cultures of the larynx to look for infection can also be taken this way, added Dr. Klein.
To evaluate vocal fold immobility, otolaryngologists use electromyography (EMG), a test that provides information about the muscles’ innervation, said Dr. Klein.
Physicians may also use EMG to target laryngeal muscles to treat spasmodic dysphonia, added Dr. Zeitels.
Laser Treatments
If a biopsy indicates that the patient has benign or precancerous lesions of the larynx, physicians may use various kinds of lasers placed in the channel of a scope to ablate or shrink them, said Greg Postma, MD, Professor of Otolaryngology and Director of the Medical College of Georgia Center for Voice and Swallowing Disorders in Augusta.
Photoangiolytic laser procedures largely include excision of benign tumors, namely laryngeal papilloma caused by human papillomavirus (HPV) and dysplasia, said Michael Johns III, MD, Director of the Emory Voice Center and Chief of Otolaryngology at the Emory Crawford Long Hospital and Assistant Professor of Otolaryngology at Emory University School of Medicine.
Dysplasia usually occurs diffusely in the larynx and frequently recurs, said Dr. Johns. Consequently, otolaryngologists will need to perform frequent biopsies and follow these with serial endoscopies. With photoangiolytic laser treatments, patients can undergo multiple treatments without general anesthesia and no significant health risk, he explained. Moreover, targeting the lesion’s vascular supply with the laser allows the physician to treat more tissue than with a resection, added Dr. Johns.
Papillomatosis is a recurrent problem for which the traditional approach was direct laryngoscopy and excision in the operating room, continued Dr. Johns. We’d have to wait until the disease was advanced, which could cause large fluctuations in the patient’s voice and quality of life, he said. With lasers, physicians can treat the disease more frequently to keep it at bay and limit wide voice fluctuations, he explained.
Although physicians used to put patients under general anesthesia in the operating room for these conditions, now we treat in them in the office under local anesthesia in 20 to 30 minutes, said Dr. Zeitels, who, with his colleagues, performed the first office-based laser procedure to treat laryngeal disease in the fall of 2001 using a pulsed-dye laser (PDL). Dr. Zeitels has received free lasers on which to conduct research, but has not accepted funding from manufacturers.
Types of Lasers
Dr. Zeitels noted that both the 585-nm PDL and the 532-nm pulsed potassium-titanyl-phosphate (KTP) are commonly used for vocal cord lesions.
A 2004 study, conducted by Dr. Zeitels and his colleagues,1 found that the PDL was an effective treatment for benign lesions. However, although PDL is effective, the KTP technology is superior, he said.
Most important, the hemostasis provided by the KTP laser is substantially more effective.2-6
Unlike the KTP, the PDL frequently causes bleeding during the procedure due to the technology’s short pulse width, which can cause blood within the vessel wall to heat eccentrically and too quickly, causing it to rupture, explained Dr. Zeitels. The KTP laser, with its adjustable extended pulse width, is less likely to rupture vessel walls.
The extended pulse width also allows for more efficient intravascular coagulation, which results in a significantly more precise and effective surgical procedure, he said.3-6
Additionally, bleeding will inhibit visualization of the treatment area and can cause the patient to cough, both of which can limit the effectiveness of the procedure, noted Dr. Zeitels. Free blood will also absorb the laser energy instead of the targeted diseased tissue.2,4-6
Lasers continue to evolve with increasingly smaller fibers, said Dr. Zeitels. Of particular importance, he noted, is that the smaller glass fibers used in the KTP laser (≃0.3 mm and 0.4 mm) have an advantage over PDL (0.6 mm) because the smaller fibers allow for significantly more suction capability through the working channel of the flexible laryngoscope.2
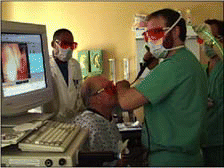
 Figure. Office-based green-light pulsed-KTP laser surgery of vocal cords. Note that the green-light laser energy is transmitted through a 0.3-mm glass fiber into the flexible laryngoscope to reach the patient’s vocal cords. Courtesy of Steven Zeitels, MD
Figure. Office-based green-light pulsed-KTP laser surgery of vocal cords. Note that the green-light laser energy is transmitted through a 0.3-mm glass fiber into the flexible laryngoscope to reach the patient’s vocal cords. Courtesy of Steven Zeitels, MDOther Laser Applications
Lasers can be used to treat polyps in the office, said Dr. Zeitels. However, these lesions are not diseases that are biologically predisposed to recurrence, requiring multiple general anesthesia, as with papillomatosis and dysplasia, he said.
Patients who need surgical treatment of vocal polyps are usually younger so that general anesthesia is not an issue, added Dr. Zeitels. Furthermore, the metric for success in treating vocal polyps since the origin of office-based mirror-guided endolaryngeal surgery in the 1800s is that the polyp is completely removed, he explained.
Leaving portions of the fibrovascular lesion for the convenience of office-based management predisposes the patient to repeated phonotraumatic injury, which would be considered by most physicians to constitute failed surgical management, said Dr. Zeitels.
Finally, said Dr. Zeitels, microlaryngoscopic subepithelial resection of benign lesions of the superficial lamina propria-for example, nodules, hemorrhagic polyps, and cysts-has long been demonstrated to provide the optimal postoperative pliability of the phonatory mucosa, which translates to voice quality.7-9
However, for patients who are truly reluctant to undergo general anesthesia for microlaryngoscopic polyp removal in the operating room, office-based treatment with the pulsed-KTP laser provides a viable, albeit nonoptimal, option, said Dr. Zeitels.
Photoangiolytic laser treatment of carcinoma in situ and early invasive glottic cancers may be a future potential modality, said Dr. Johns. We’re continuing to take a disease that is treated with radiation therapy and saving it for recurrences and more advanced disease, he said.
The vocal folds are privileged organs, meaning that early malignant lesions very seldom metastasize to lymph nodes in the neck, added Dr. Johns. It’s protected from lymphatic spread, which allows for treating lesions in a graded fashion, he explained. We can treat early carcinoma in stages to slowly get rid of the cancer.
The effectiveness of photoangiolytic laser therapy for carcinoma in situ and early invasive laryngeal cancer needs to be compared to radiotherapy, and data are forthcoming, said Dr. Johns.
Carcinoma in situ has been treated in the office for about seven years, noted Dr. Zeitels. And we have had great success with microlaryngoscopic angiolytic laser treatment of early glottic cancer, he said, citing a study.10
However, reliable office-based flexible laryngoscopic treatment of glottic cancer with optimal voice results is unlikely due to limitations of magnification, flexible laryngoscopic tissue handling and dissection, tangential exposure of the curving glottis, and a moving microcirculatory tissue target, he said.
Laser Cost Considerations
In addition to their proven efficacy, other benefits of in-office laser procedures are that they are faster, safer, and less expensive than operating room procedures requiring full anesthesia, said Dr. Postma, citing a study of which he was one of the authors.11
He and his colleagues evaluated the cost savings of office-based PDL treatment compared with operating room-based laryngoscopy under general anesthesia for the treatment of recurrent respiratory papillomas, granulomas, leukoplakia, and polypoid degeneration. The researchers found that in-office PDL saved more than $5000 per case; however, they noted that current reimbursement rates do not cover the cost of the laser procedure.
The biggest issue for a lot of us is reimbursement, said Dr. Postma. Laser technology is way ahead of the reimbursement system.
Indirect costs, such as lost workdays due to undergoing full anesthesia and surgery, also need to be considered, said Dr. Postma. With in-office procedures, patients often go back to work right away, he said.
Injections
In-office injections are another common and effective in-office procedure for treating a number of laryngeal disorders in awake patients. About 90 percent of my patients who need injections are awake, said Dr. Klein.
Otolaryngologists should learn to perform awake injections for the benefit of the patient, said Dr. Johns. Patients with paralyzed vocal folds can often benefit from injection, especially if they aren’t suitable for general anesthesia, such as those who have undergone cardiac thoracic surgery, he explained. Injections get these individuals out of the hospital faster, gets them eating and swallowing faster, and improves their quality of life, he said.
Dr. Postma and his colleagues perform in-office injections in patients with vocal cord paralysis to bulk up or change the position of the larynx. We can also inject the voice box with different types of augmenting fillers when the vocal folds don’t touch properly, he said.
With the aging population and an increasing number of people having problems with their voice because of vocal cord atrophy, voice therapy and vocal cord augmentation with injections may become more common, noted Dr. Johns.
Botox injections are useful for treating spasmodic dysphonia, whereas steroid injections can reduce vocal cord inflammation, added Dr. Postma.
Botox is also therapeutic for essential tremor that affects the larynx, noted Dr. Klein.
We’ll also inject cidofovir, an antiviral, in patients who have laryngeal papillomas, said Dr. Postma.
Several different methods can be used for administering injections, noted Dr. Klein. Some are given through the mouth or directly through the skin in the neck from various angles, he explained. Some require anesthetizing the patient’s nose to pass a flexible scope down to the vocal fold for visualization of the injection, he said.
Precautions and Contraindications
When conducting these diagnostic and therapeutic procedures, otolaryngologists should be aware that some patients won’t tolerate a scope, said Dr. Postma.
Some patients prefer to undergo full sedation, said Dr. Klein. Some people simply don’t tolerate scopes in their nose and mouth, he said.
Moreover, the patient’s nose may be too small for scope insertion, said Dr. Postma.
We recommend that otolaryngologists put patients who are singers under full sedation to treat lesions on their vocal folds, said Dr. Klein. Because of the nature of their vocal demands, we choose to put them to sleep to allow us to be more meticulous and to increase the chance of a good vocal outcome, he said.
One drawback of awake, in-office procedures is that physicians lose some precision, said Dr. Johns. Otolaryngologists should be aware that because the larynx is moving, the patient is awake and moving, and instrumentation is being passed through the flexible endoscope, that they don’t have the same precision as in the operating room, he explained. When precision is of utmost importance, then treatment in operating room makes sense, said Dr. Johns.
Otolaryngologists also have to be very careful using lasers for benign lesions that would otherwise require a precise resection under anesthesia, said Dr. Zeitels.
They should also be extremely careful while working with lasers on the internal surface of the vocal folds to avoid scarring, and should treat both vocal folds at the same time in the anterior commissure because it can result in webs and adhesions, Dr. Zeitels added.
Overall, physicians should take their time with awake procedures, advised Dr. Postma. You need to take your time with topical anesthesia, and you need to let patients know everything you are going to do, he said.
Physicians should also keep in mind that some patients who are on certain anticoagulants may need to be under full sedation in case bleeding problems arise, said Dr. Klein.
Treating patients who are anticoagulated was problematic when we used the PDL but has not been a problem with the KTP due to enhanced hemostasis associated with the longer pulse width, said Dr. Zeitels.
Equipment and Training
A number of opportunities exist to acquire experience in performing in-office awake procedures for patients with laryngeal disease, and many otolaryngologists already have some of the needed equipment.
Most otolaryngologists already have a flexible scope in their office, said Dr. Klein. To perform in-office laryngeal procedures using existing equipment, all one needs are scope sheaths that provide side ports through which one can introduce biopsy forceps, topical anesthetic, or a laser fiber, he explained. Also available are flexible endoscopes with side ports that don’t require a sheath, he added.
One is first exposed to these types of procedures in residency, said Dr. Klein. However, a fellowship in laryngeal surgery and care of the professional voice helps the otolaryngologist acquire a better knowledge of the procedures, he said.
For otolaryngologists who are done with their training and have been in practice for a number of years, continuing medical education (CME) courses provide the opportunity to learn more about these procedures, said Dr. Klein.
These courses are available through the American Academy of Otolaryngology-Head and Neck Surgeons, noted Dr. Zeitels. Courses are also available at major medical institutions such as Harvard Medical School (http://cme.hms.harvard.edu/ ) and Massachusetts General Hospital, he said.
With any sort of novel approach, technology, or procedure, it’s important to proceed cautiously as you work your way through the learning curve, concluded Dr. Klein.
What Patients Should Know
Physicians should keep patients well informed about what to expect when undergoing in-office awake procedures, said the experts interviewed for this article.
Patients should be prepared to experience some mild discomfort during awake procedures. But even old or infirm patients tolerate these procedures pretty well, said Dr. Klein.
Patients should be advised not to eat or drink an hour or two before the procedure because they may experience some gagging. Additionally, Dr. Postma recommends that they avoid food and drink postprocedure because their throats may still be numb and they can aspirate.
Generally, patients won’t need narcotics for pain or antibiotics to prevent infection postprocedure. They may, however, need to refrain from taking aspirin or anticoagulants beforehand.
They should also expect a minor sore throat afterward, which can be treated with acetaminophen or ibuprofen, said Dr. Johns.
Mild injury to structures of the nose and mouth may occur but are rare. Any time you work on the voice box, whether with injection or laser, there’s always a risk of scarring, hoarseness, and recurrence of the problem, Dr. Klein explained.
Individuals can also experience a reaction to injection materials, airway compromise, infection, bleeding, or swelling from procedures, although such reactions are rare.
They should also anticipate their voice to wax and wane in clarity for a couple of weeks (whether after an injection or a laser procedure) due to swelling. Voice rest is necessary with laser procedures but not with injection.
Finally, if patients are coughing up blood or having problems breathing, they should come back into the hospital immediately.
Most Patients Prefer Awake Procedures
In addition to the effectiveness of many in-office awake laryngeal procedures, the majority of patients appear prefer this type of treatment versus being in the operating room under full sedation, said Dr. Postma, citing a study of which he was a co-author.12
He and his colleagues studied 131 patients who had 328 unsedated in-office PDL procedures. Eighty-nine of these patients who completed a phone survey reported an average comfort score of 7.4, with 10 representing minimal discomfort. Eighty-seven percent said they would rather have an unsedated in-office procedure than surgery under general anesthesia for any further treatment of their disease.
Patients with recurrent papillomas had to be treated in the operating room three or four times a year, explained Dr. Postma. They love that they can be treated in-office now, he said.
Another reason patients may prefer in-office awake procedure is that they don’t have to take three or four days off from work, noted Dr. Klein.
Older individuals especially want to avoid surgery, commented Dr. Zeitel. Patients benefit from not having an extensive presurgical workup, and they avoid general anesthesia. Moreover, because less surgery takes place, there is often less voice rest, he said.
References
- Zeitels SM, Franco RA Jr, Dailey SH, et al. Office-based treatment of glottal dysplasia and papillomatosis with the 585-nm pulsed dye laser and local anesthesia. Ann Otol Rhinol Laryngol 2004;113:265-76.
[Context Link] - Zeitels SM, Akst LM, Burns JA, et al. Office-based 532-nm pulsed KTP laser treatment of glottal papillomatosis and dysplasia. Ann Otol Rhinol Laryngol 2006;115:679-85.
[Context Link] - Broadhurst MS, Akst LM, Burns JA, et al. Effects of 532 nm pulsed-KTP laser parameters on vessel ablation in the avian chorioallantoic membrane: implications for vocal fold mucosa. Laryngoscope 2007;117:220-5.
[Context Link] - Zeitels SM, Anderson RR, Hillman RE, Burns JA. Experience with office-based pulsed-dye laser (PDL) treatment. Ann Otol Rhinol Laryngol 2007;116:317-8.
[Context Link] - Zeitels SM, Burns JA. Office-based laryngeal laser surgery with local anesthesia. Curr Opin Otolaryngol Head Neck Surg 2007;15:141-7.
[Context Link] - Zeitels SM, Burns JA. Office-based laryngeal laser surgery with the 532-nm pulsed-potassium-titanyl-phosphate laser. Curr Opin Otolaryngol Head Neck Surg 2007;15:394-400.
[Context Link] - Bouchayer M, Cornut G. Microsurgical treatment of benign vocal fold lesions: indications, technique, results. Folia Phoniatr 1992;44:155-84.
[Context Link] - Hochman II, Zeitels SM. Phonomicrosurgical management of vocal fold polyps: the subepithelial microflap resection technique. J Voice 2000;14:112-8.
[Context Link] - Zeitels SM, Hillman RE, Desloge R, et al. Phonomicrosurgery in singers and performing artists: treatment outcomes, management theories, and future directions. Ann Otol Rhinol Laryngol Suppl 2002;190:21-40.
[Context Link] - Zeitels SM, Burns JA, Lopez-Guerra G, et al. Photoangiolytic laser treatment of early glottic cancer: a new management strategy. Ann Otol Rhinol Laryngol Suppl 2008; 199:1-24.
[Context Link] - Rees CJ, Postma GN, Koufman JA. Cost savings of unsedated office-based laser surgery for laryngeal papillomas. Ann Otol Rhinol Laryngol 2007;116:45-8.
[Context Link] - Rees CJ, Halum SL, Wijewickrama RC, Koufman JA, Postma GN. Patient tolerance of in-office pulsed dye laser treatments to the upper aerodigestive tract. Otolaryngol Head Neck Surg 2006;134:1023-7.
[Context Link]
©2008 The Triological Society
Leave a Reply