Infantile hemangiomas and lymphatic malformations (LM) are vascular anomalies that otolaryngologists-head and neck surgeons often encounter in their practices. Infantile hemangiomas and LMs differ from one another in prevalence, etiology, and clinical presentation, but both may be undergoing potential shifts in treatment, depending on research outcomes.
Appropriate classification of vascular anomalies is integral to their successful management, said Nancy M. Bauman, MD, Professor of Otolaryngology-Head and Neck Surgery at Children’s National Medical Center in Washington, DC.
The International Society for the Study of Vascular Anomalies (ISSVA) adopted the classification scheme proposed by John Mulliken and Julie Glowacki in 1996, recognizing vascular tumors as lesions with endothelial cell hyperplasia, or hemangiomas, and vascular malformations as lesions arising due to dysmorphogenesis, or LMs (see table).
Hemangiomas
Infantile hemangiomas are the most common tumor of infancy and arise in 5% to 10% of infants, with two-thirds of lesions involving the head and neck, said Dr. Bauman. Hemangiomas affect females about three times as often as males, and arise more commonly in Caucasians and preterm infants.
Proposed etiologies of hemangiomas include defects in angiogenesis, mutations in growth regulatory genes of endothelial cells, and embolization of placental microvessels, said Dr. Bauman.
Tumors first become clinically apparent when a child is two to four weeks old, said Elaine Siegfried, MD, Professor of Dermatology at St. Louis University. You typically don’t see them at birth, she said. They usually grow for about six to 12 months and then take two to 10 years to involute, she explained.
We once believed that asymptomatic infantile hemangiomas should not be treated, since they will eventually involute, said Dr. Bauman. We now know that some of these hemangiomas-particularly large lesions of the lip or the tip of the nose-will cause permanent disfigurement, and early intervention may improve the cosmetic outcome before the lesions permanently affect the underlying structures.
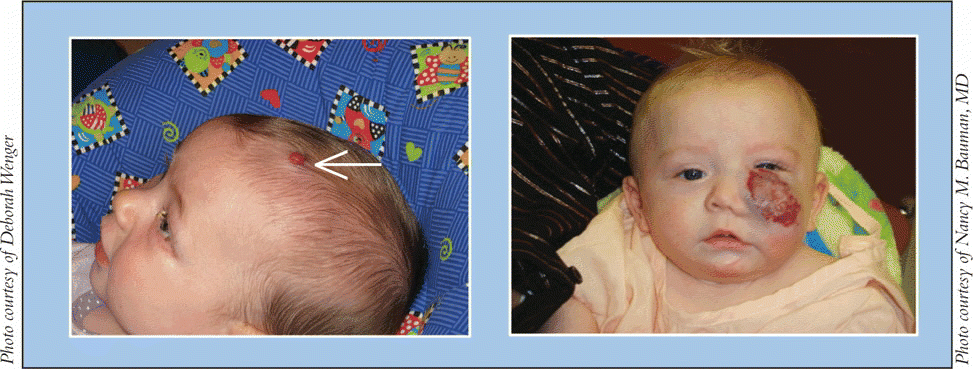
Complications
Textbooks generally don’t describe different types of hemangiomas, but physicians recognize that subsets of high-risk and low-risk tumors exist, said Dr. Siegfried. High-risk hemangiomas tend to be segmental, while low-risk tumors are generally focal, she noted.
Most hemangiomas are relatively asymptomatic and should be allowed to involute on their own, but about 25% produce symptoms related to their size and location, noted Dr. Bauman. For example, periorbital hemangiomas can obstruct the visual axis and affect vision development, she said.
Tumors in the subglottis cause stridor and airway obstruction that can be life-threatening, said Dr. Bauman. Additionally, hemangiomas in the perineal region are prone to ulceration and infection, she said.
Ulceration can be painful enough to require hospitalization and narcotics, added Dr. Siegfried.
Physicians should also be aware that hemangiomas may occur as isolated lesions or in association with other findings, noted Dr. Siegfried. For example, PHACES (posterior fossa, hemangiomas, arterial, cardiac, eye, sternum) involves a large segmental hemangioma on the face or neck in addition to posterior fossa abnormalities, cerebrovascular anomalies of the neck and brain, cardiac defects, and eye and sternal abnormalities.
Physicians must be aware of this constellation of symptoms and evaluate patients appropriately, noted Dr. Bauman. Patients may not exhibit all signs of PHACES, so infants with large facial hemangiomas should undergo brain imaging to exclude intracranial anomalies, she added.
Another association is SACRAL (spinal dysraphism, anogenital, cutaneous, renal/ urologic anomalies, associated with an angioma of lumbosacral localization), said Dr. Bauman.
Imaging Studies
Imaging studies are useful to evaluate hemangiomas whose extent is not readily visible. Computed tomography (CT), ultrasound (US), and magnetic resonance imaging (MRI) are all valuable studies, but MRI is preferred because it clearly shows the relationship of the tumor with adjacent tissues without causing radiation exposure, said Dr. Bauman. Ultrasound is noninvasive, and can be useful in measuring and monitoring peak blood flow through a lesion, she said.
Treatment
If the tumor is small, focal, and not at a site where it interferes with normal function, it may need anticipatory guidance rather than treatment, said Dr. Siegfried. However, because physicians can’t predict how fast hemangiomas will grow, they tend to treat those at high-risk sites.
First-line treatment options include topically applied or intralesionally injected corticosteroids, said Dr. Siegfried.
Systemic corticosteroids are effective in high doses but have side effects such as irritability, reflux, high blood pressure, glaucoma, and immune and adrenal suppression, noted Dr. Siegfried. They can also interfere with sleep and can increase appetite, she said.
Systemic steroids are likely effective in about 75% of cases of infantile hemangiomas, said Dr. Bauman. Steroids are most effective when given during the early phase of rapid tumor growth, she said, adding that she uses alcohol-free prednisolone. Steroids are typically administered for several months, and many babies develop a cushingnoid appearance from temporary redistribution of fat to their back and cheeks. Linear growth may also be temporarily delayed in those taking high-dose corticosteroids for prolonged periods, added Dr. Bauman.
Additionally, physicians should be aware that congenital hemangiomas do not respond to steroids, said Dr. Bauman. Congenital hemangiomas differ from infantile hemangiomas in that they are present at birth and sometimes have a distinctive appearance with a halo of normal appearing skin that slopes upward toward the border of the hemangioma.
Congenital hemangiomas are divided into rapidly involuting lesions (RICH), which resolve during the first year of life, and noninvoluting hemangiomas (NICH), which do not resolve, said Dr. Bauman. The diagnosis is not always clear, but infantile hemangiomas express glucose 1 transporter protein (glut-1 positive), whereas congenital hemagniomas do not, she said.
Corticosteroids remain the standard of care, but researchers are actively investigating a potential new treatment. A recent French study of 11 children summarized in a short communication to the New England Journal of Medicine (2008;358:2649-51) has generated some interest in the use of propranolol for hemangiomas, noted Dr. Siegfried.
Researchers described two children with hemangiomas who received corticosteroids but were given propranolol at 2 mg/kg of body weight per day to address either obstructive hypertrophic cardiomyopathy or increased cardiac output. After receiving propranolol, their hemangiomas improved. Investigators gave propranolol to nine more children with hemangiomas, and all experienced a change in tumor color, from red to purple, and a softening of the lesion within 24 hours.
 We’ve done dozens and dozens of procedures with OK-432 and never had a complication due to its use.
We’ve done dozens and dozens of procedures with OK-432 and never had a complication due to its use.-Joseph E. Kerschner, MD
Vasoconstriction, decreased expression of vascular endothelial growth factor (VEGF) and basic fibroblast growth factor (BFGF), and apoptosis of capillary endothelial cells may explain the therapeutic effect of propranolol, wrote the study authors.
The French study looks promising, but we don’t have enough data to make propanolol a first-line drug, said Dr. Siegfried, who along with several colleagues, wrote a response to the study (NEJM 2008; 359:2846-7). The authors of the paper didn’t have space to talk about how to use the drug, she said, adding that the dosing described could cause bradycardia, hypotension, or sustained hypoglycemia, the last of which has been associated with seizures or cerebral palsy in infants.
In their letter, Dr. Siegfried and her colleagues described a propanolol protocol that includes a baseline echocardiogram and either 48-hour hospitalization or home nursing visits to monitor vital signs and blood glucose levels. Propranolol is given every eight hours, with a starting dose of 0.16 mg/kg. The dose is incrementally doubled to a maximum of 0.67 mg/kg/dose or 2.0 mg/kg daily, if the patient has normal vital signs and glucose levels. The drug is then be tapered over a two-week period.
Dr. Bauman and her colleagues obtained IRB approval to initiate a prospective, randomized study comparing the efficacy of propanolol and prednisolone in treating symptomatic infantile hemangiomas.
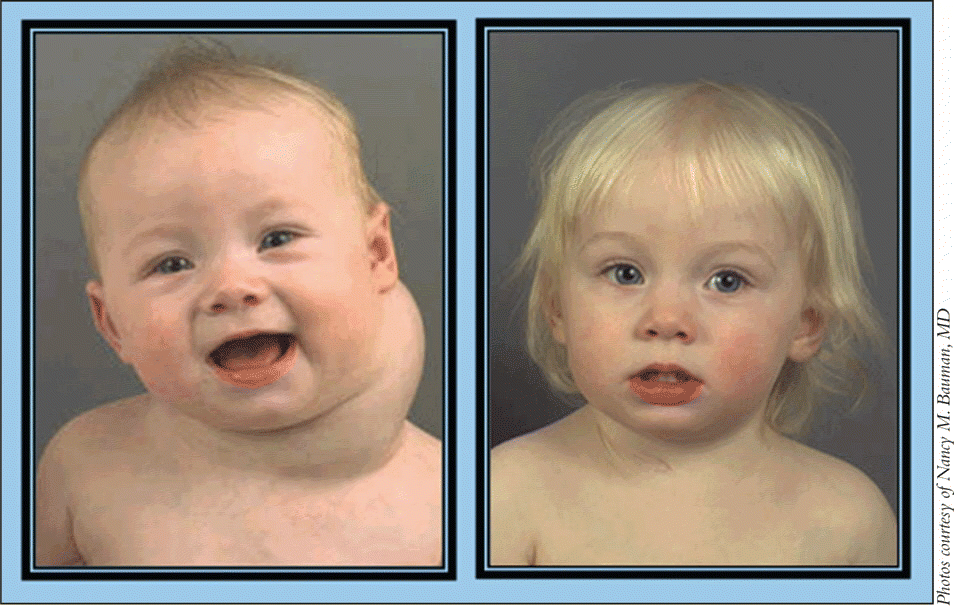
Propranolol appears to be well tolerated and may have fewer side effects than prednisolone therapy, but whether it is as effective as high-dose steroids is still unclear, said Dr. Bauman. What is clear, however, is how difficult it is to organize a prospective study and to randomize patients while controlling for size and site of lesions and age at which therapy is initiated, she added.
Propranolol can interfere with glycogenolysis, which is the normal physiologic response to fasting, noted Dr. Bauman. Obstruction of glycogenolysis in a nonfeeding infant can cause hypoglycemia that can be severe enough to induce seizures, added Dr. Bauman. It is therefore important that infants are fed on a regular schedule and that their blood sugars be carefully monitored if they develop vomiting or diarrhea while on propranolol.
In addition to assessing the clinical response to the medications, Dr. Bauman and her colleague, Diego Preciado, MD, will be collecting urine specimens before, during, and after treatment to perform metabolomics to assess protein metabolite expression that may help identify predictors of response to propanolol and prednisolone. They also will perform microarray gene chip analysis on hemangiomas to better understand why some tumors respond to therapy and others do not.
Much has been learned about hemangiomas, particularly through the outstanding contributions of the vascular anomalies team at Boston Children’s Hospital, said Dr. Bauman. We hope to further our understanding of this congenital anomaly that can cause severe problems for many infants, she added.
Lymphatic Malformations
Compared with hemangiomas, LMs are rare, noted Joseph Kerschner, MD, Professor and Chair of Pediatric Otolaryngology at Medical College of Wisconsin. We are a major regional referral center in the Midwest, and we only see about 30 to 40 new cases of LMs a year, he said.
Overall, about two or three cases of LMs occur per 100,000 hospital admissions, said Mark Smith, MD, Director of Pediatric Otolaryngology at Children’s Hospital at Dartmouth, Dartmouth-Hitchcock Medical Center. Larger medical centers with multidisciplinary vascular anomalies clinics will naturally see more, he said.
These lesions, which are developmental anomalies of the lymphatic system, can be further described as macrocystic, microcystic, or mixed macrocystic-microcystic, and are most commonly seen in the head and neck of children, said Dr. Smith. Macrocystic lesions contain spaces filled with at least 2 cc of lymphatic fluid, he explained. Microcystic lesions contain multiple, smaller collections of fluid, and mixed lesions contain fluid collections of both types.
LMs may start to form during the embryonic stage, and the age at which they present in children varies, noted Dr. Smith.
Some lesions present during early childhood, whereas others present during the teen years or even during the adult years, noted Dr. Bauman.
Imaging Studies
Obtaining an MRI with contrast allows physicians to differentiate among the macrocystic, microcystic, and mixed macrocystic-microcystic lymphatic malformation subtypes, said Dr. Smith. CT scans can sometimes be misleading, as truly microcystic lesions may appear as macrocystic, he added.
Ultrasound is usually reserved for intraoperative identification of individual cysts for injection sclerotherapy; it can be used as a diagnostic tool as well, but is not as precise as MRI, he said.
Complications
Most LMs are not life-threatening, but lead to unsightly swellings of the face and neck, said Dr. Smith. Severe complications can develop when LMs expand and obstruct the upper aerodigestive tract, interfering with breathing or eating, he said.
Large LMs can compress the airway and be life-threatening, but they are fairly rare, said Dr. Kerschner. If a large lesion grows in and around the head and neck it can also affect vision, he added.
Treatment
Some physicians opt for watchful waiting of these lesions if they are not causing any functional problems because a small percentage-between 1% and 5%-resolve spontaneously, said Dr. Kerschner.
Surgical excision is a treatment option for problematic macrocystic lesions, he said. However, one challenge of surgery is that LMs tend to be in close proximity to important structures such as major arteries and nerves. Given that LMs are benign lesions, resection needs to preserve as much normal function as possible, he noted.
Although a common form of therapy, surgical excision is frequently incomplete and unsatisfying, said Dr. Smith. These malformations often insinuate themselves around important nerves and blood vessels, so removal is often incomplete and associated with recurrence and morbidity. Even with meticulous dissection, disruption of the tissue lymphatics in the surgical field can lead to poor cosmetic results, he said.
Sclerotherapy is a relatively new treatment approach to macrocystic LMs that has a high success rate, said Dr. Kerschner. This treatment involves injecting a material inside the cyst cavity to irritate its contents and to make the cyst wall collapse on itself to prevent fluid from re-entering, he explained.
Agents injected into the cyst include alcohol and doxycycline, said Dr. Kerschner. However, he and his colleagues primarily use OK-432 (picibanil), an investigational drug that is a derivative of a Streptococcus organism. When injected into the cyst cavity, OK-432 creates an inflammatory response, he explained.
OK-432 also appears to be safe. We’ve done dozens and dozens of procedures with OK-432 and never had a complication due to its use, explained Dr. Kerschner.
More than 400 of these procedures have been done in the United States in the past 15 years, added Dr. Bauman.
 The French study looks promising, but we don’t have enough data to make propanolol a first-line drug.
The French study looks promising, but we don’t have enough data to make propanolol a first-line drug.-Elaine C. Siegfried, MD
Sclerotherapy may sometimes be used in conjunction with surgery. For example, physicians can use OK-432 in especially large lesions to reduce their size, making surgical resection easier, noted Dr. Kerschner.
Additionally, using sclerotherapy to treat especially large LMs that partially obstruct the airway may make borderline airway obstruction worse, and tracheotomy may be temporarily necessary, noted Dr. Smith.
In general, OK-432 appears to be more effective in achieving resolution of macrocystic LMs than other sclerotherapy agents, said Dr. Kerschner.
Most studies of doxycycline for treatment of LMs have included small numbers of patients and are retrospective, noted Dr. Smith. What would be really interesting is to organize a multi-institutional sclerotherapy study, with half the patients receiving OK-432 and half receiving doxycycline, he said, adding that the two drugs probably work differently. Whereas OK-432 is an immunostimulant that causes the body to attack the inner lining of the LM, the mechanism of doxcycline is poorly understood, and it may act more as a direct irritant, he said.
One advantage of doxycycline is that it is easier to obtain than OK-432, which requires enrollment in a clinical study. Most people aren’t willing to jump through the hoops of pre-study and post-study work, noted Dr. Smith.
The most recent data from the OK-432 Collaborative Study Group (Laryngoscope 2009;119:107-15) concluded that OK-432 immunotherapy is an effective, safe, and simple treatment option for the management of macrocystic cervicofacial lymphatic malformations.
The group conducted a prospective, randomized, multi-institutional, phase II clinical trial at 27 U.S. academic medical centers between January 1998 and November 2004. One hundred seventeen patients were randomized into immediate or delayed treatment groups, and 34 patients were assigned to an open-label group.
Treatment consisted of up to four intralesional OK-432 injections (0.2 mg per injection) delivered at eight-week intervals. Some children would respond well to just a single injection, especially for macrocystic lesions comprised of a single large cyst like a water balloon under the skin, said Dr. Smith, who was one of the study authors.
Change in lesion size was graded as complete (90%-100%), substantial (60%-89%), intermediate (20%-59%), or none (<20%). Ninety-four percent of patients with macrocystic tumors had a complete or substantial response, whereas 63% of those with mixed LMs responded.
Patients with microcystic LMs did not respond to the treatment. Microcysts don’t respond well to sclerotherapy because it is impossible to inject the material into such a small cavity, said Dr. Smith. We’re still trying to determine how best to treat children with microcystic lymphatic malformations, he said, adding that watchful waiting is often used in these patients.
The OK-432 Collaborative Study Group also found that fewer than 2% of patients experienced spontaneous resolution. A 9% recurrence rate was observed during a median follow-up of 2.9 years. Eleven patients experienced adverse effects, such as airway obstruction, edema, and infection related to therapy. When compared with available surgical data, OK-432 is more effective and has a lower morbidity for the treatment of LMs, they wrote.
Obtaining US Food and Drug Administration approval of OK-432 is the next big step in trying to more successfully treat children with LMs, said Dr. Smith. Obtaining FDA approval is expensive and difficult for drugs used to treat orphan diseases like LM, but we remain optimistic that it will occur, said Dr. Bauman.
Vascular Anomalies
Vascular Tumors
- Infantile hemangiomas
- Congenital hemangiomas
- Rapidly involuting congenital hemangiomas (RICH)
- Non-involuting congenital hemangiomas (NICH)
- Other rare vascular tumors
- Kaposiform hemangioendotheliomas
- Tufted angiomas
- Hemangiopericytomas
- Angiosarcomas
Vascular Malformations
- High-flow lesions with arterial component
- Low-flow lesions
- Venous malformations
- Lymphatic malformation
- Microcystic
- Macrocystic
- Mixed-flow lesions
- Send Us Your Feedback
We’d like to know what you think about our articles. Please feel free to respond to our stories by e-mailing ENToday@lwwny.com. When writing in, please include your full name, title, phone number, and e-mail address.
©2009 The Triological Society
Leave a Reply