
Explore This Issue
November 2017Background
Multilevel pharyngeal surgery is routinely indicated for patients suffering from obstructive sleep apnea (OSA) as both a first-line treatment and for patients whose disease is refractory to continuous positive airway pressure (CPAP) treatment. Tongue-base reduction surgeries to correct relative macroglasia are rapidly gaining traction as useful treatments for OSA. Novel techniques and technologies such as radio frequency ablation, coblation lingual tonsillectomy, and transoral robotic surgery (TORS)—as well as more traditional tongue-base reduction techniques—are being employed in the operating room to achieve tongue reduction. When offering surgery to a patient, the informed consent process is key in helping the patient understand the risks of the procedure. With regard to surgery of the tongue base of OSA, most consent discussions revolve around risks of bleeding or airway swelling. Because surgery is typically directed to the posterior tongue base and not the anterior tongue, taste dysfunction (TD) typically has not been emphasized in the literature. However, it remains an understandable concern of patients undergoing tongue reduction surgery, and thus physicians should be able to knowledgeably inform patients about this complication.
Best Practice
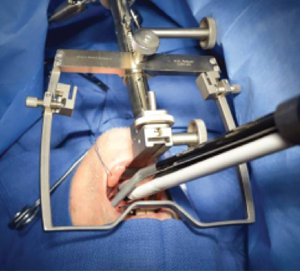
Robotic tongue-base resection.
The literature suggests that the incidence of alteration in taste sensation with coblation lingual tonsillectomy, TORS tongue-base reduction, and submucosal lingualplasty is sufficiently high to warrant warning patients of this complication. For each of these procedures, TD appears to be a complication that frequently resolves after a few months; however, in some cases it can persist for far longer and become problematic. Radiofrequency tongue-base reduction has been the most heavily studied with respect to TD and is considered a safe option that does not seem to increase the risk of TD, whereas the other tongue procedures for OSA all seem to be associated with some degree of TD after surgery. Further investigations are needed to better characterize the TD associated with each procedure and quantify the risk of TD associated with each surgery. In addition, because TD may be associated with the duration of the surgery, as well as tongue retraction instrumentation used (e.g., laryngoscope placement, Boyle-Davis gag placement), these possibilities should be considered when counseling patients (Laryngoscope. 2017;127:1253–1254).