Although most respiratory papillomatosis starts in childhood, some patients develop symptoms in adulthood. While adult-onset disease is milder, patients often still require multiple surgeries to be free of the characteristic lesions and the associated hoarseness.
Explore This Issue
July 2006In a joint phone interview, two leading experts in respiratory papillomatosis discussed the diagnosis and management of adult patients. Blake Simpson, MD, is Associate Professor and Deputy Chair of the Otolaryngology–Head and Neck Center at the University of Texas Health Science Center in San Antonio. Clark A. Rosen, MD, is Associate Professor of Otolaryngology at the University of Pittsburgh School of Medicine (Pa.), where he is the Director of the Voice Center.
“Adult respiratory papillomatosis is going to be a much less aggressive course than what otolaryngologists are used to seeing with children,” said Dr. Simpson. “These lesions grow slower, and patients go longer intervals between surgeries. Adult patients do better than children.”
Although the route of transmission is known to be perinatal in children, the transmission of adult-onset disease is unknown, he added. “My theory is that people with adult onset were probably were born with it,” he said. “It lives in the tissue of their larynx and with aging, the immune surveillance system isn’t as vigilant, and the papilloma starts growing.” He noted that this development can happen at any age. “I’ve seen it surface in 70-year-olds.”
People with adult-onset disease, then, may have had a perinatal transmission that has been dormant throughout their lives. “When you take the papilloma lesion off along with some normal adjacent tissue, you’ll find the virus in both the affected and the apparently healthy tissue,” Dr. Simpson said. “I think this phenomenon explains why the condition is milder in adults: they may have been living with it all their lives. There are a couple of theories about how adults get it, but perinatal transmission and subsequent dormancy is the only one that makes sense regarding how adults get the disease.”
Although the route of transmission is known to be perinatal in children, the transmission of adult-onset disease is unknown.
What to Look For
Patients with adult respiratory papillomatosis typically have little unique in their presentation, Dr. Simpson said. “If a 20- to 60-year-old patient says he or she has been hoarse for the past several years, there could be many causes,” he said. “They typically have gradually progressive hoarseness.” Again, this report alone would not lead down the papillomatosis pathway. “However, if the patient says, ‘I’ve had two surgeries with polyps removed,’ papillomatosis may be the cause. The whole differentiating thing about papilloma is that it recurs. If it recurs, it’s almost always papilloma.”
Dr. Rosen agreed. “The only suspicious item in the history would be repeat surgery with rapid recurrence of hoarseness,” he said. “That’s a tip-off.”
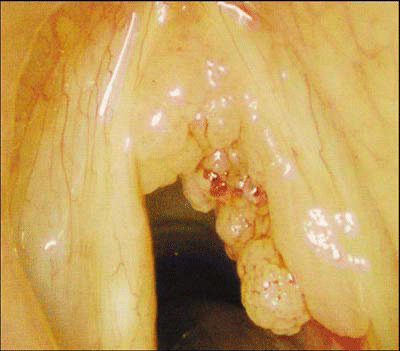
With any report of hoarseness, the otolaryngologist should next view the vocal apparatus with either a laryngoscope or with videostroboscopy. In the patient with papillomatosis, the view on the fiberoptic scope will show multiple lesions with grapelike projections on the vocal cords. The lesions will typically be on the true vocal folds, the intraglottis, and the supraglottic structures. “Each little projection has its own blood vessel,” Dr. Simpson said. “A lot of times you’ll see something that looks like a target, because the vessel creates a dot in the center. When you see multiple red dots inside circular lesions, it’s almost always papilloma. Multiple lesions and a target on the end of the lesion are the telltale signs.”
“The most important issue is how the larynx looks on physical exam,” Dr. Rosen said. “There are a variety of ways papilloma can look: bulky, exophytic, or superficial spreading.” He agreed with small Dr. Simpson that the characteristic that identifies papilloma is the blood vessel in the center of each of the lesions.
“Adult respiratory papillomatosis is going to be a much less aggressive course than what otolaryngologists are used to seeing with children.” – —Blake Simpson, MD
Although viewing such lesions will lead to a strong suspicion of papilloma, the otolaryngologist will typically obtain a biopsy with forceps and either send the specimen to the pathologist or do a frozen section in the operating room. “Squamous cell carcinoma can resemble papilloma, so you really can’t go forward until the diagnosis is confirmed,” Dr. Simpson said.
Choices for Removal
When the papilloma diagnosis has been confirmed, the lesions can be removed by several methods, including laser, microdebriding, and forceps. “There is no clear consensus regarding the best ways to remove papilloma lesions,” Dr. Simpson said. “There are a lot of ways to remove them correctly with good results, so the means of removal depends on what you’re comfortable with.”
Although he has used a CO2 laser to remove papilloma lesions, Dr. Simpson primarily uses a microdebrider or shaver, which shaves off the lesion. “The CO2 laser vaporizes the tissue,” he said. “If used improperly, it can cause damage from heating up of the surrounding tissue and can lead to scarring. Therefore, many people think the microdebrider is safer because it’s a cold instrument.” The microdebrider may also be less expensive, more accessible in settings without a CO2 laser, and it avoids the risk of laser fire.
The risk of viral spreading through the laser plume is still an ongoing controversy. Although live virus particles have been found in the laser plume, and operating room staff can wear protective masks, “I’m not aware of any cases where it’s transmitted to the operating room personnel,” he said. “The precautions with suctioning and the mask would make that extremely rare.”
The lesions should be removed in one or two surgical stages, depending on anterior commissure involvement Dr. Rosen said. “If you are too aggressive and remove disease on both sides, then you may end up with a [web].… So then remove it on one side, wait for a month, and then do the other side, to allow for healing.”
Ongoing Care
After removing the lesions, the otolaryngologist needs to monitor the patient for recurrence. When talking to patients, Dr. Simpson compares the surgery and postoperative monitoring to mowing a lawn. The lawn will grow back, and so does papilloma. “Patients can understand that,” he said. “Most practitioners realize that the nature of the disease is that it’s recurrent.”
Dr. Rosen noted that postoperative monitoring for hoarseness symptoms will help the physician determine how quickly an individual patient’s papilloma returns. “Some have surgery every three to five years,” He said. “Others have it every month. There’s a wide variety in growth rates.”
Cidofovir to Prevent Regrowth
Both agree that repeat surgery is necessary when symptoms return. Some otolaryngologists use the antiviral agent cidofovir (Vistide) on an off-label basis, but its use in this setting is fraught with controversy, Dr. Simpson said. Cidofovir was originally developed to treat patients with human immunodeficiency virus (HIV) with cytomegalovirus (CMV) retinitis. “Some physicians are concerned that we’ll see some malignancies related to the cidofovir,” he said. “We’ve only been using it in adult papilloma for five years.”
“The most important thing is for the surgeries to be done in a conservative, precise fashion.” – —Clark A. Rosen, MD
He noted that in some animal studies, treated rats were more likely to develop breast cancer. “We started using cidofovir in pediatric patients and found it played a major role in slowing growth,” Dr. Simpson said. “But we don’t know the long-term effects. A lot of pediatric otolaryngologists won’t use it at all anymore. The enthusiasm has cooled off, but it’s still a good choice in aggressive disease.”
Dr. Rosen added that he also uses cidofovir but agreed it should be used with great caution and reserved for patients with moderate to severe disease who have been counseled on the treatment’s potential risks.
“The most important thing is for the surgeries to be done in a conservative, precise fashion,” Dr. Rosen said. “Most patients will have repeated surgeries and most will develop scars in the vocal cords,” he said. “The treating otolaryngologist should exercise great care and proceed with the surgery in a non-aggressive fashion. The disease is not eradicated with surgery; it’s kept under control at best. Aggressive surgery and laser won’t keep recurrences from happening.” He added that the use of cidofovir can markedly reduce the frequency with which some patients require repeat surgeries.
©2006 The Triological Society


Leave a Reply