Tinnitus, classically defined as the perception of sound that has no external source, and referred to by some as a phantom auditory perception, plagues as many as 50 million Americans, 12 million of them severely; and 2 to 4 million people are debilitated by it. For many years, progress toward effective treatments for tinnitus was hindered by an obscured understanding of its underlying physiologic mechanisms. Although tinnitus was presumed to be primarily a disorder of the ear, findings now are eliciting insights pointing to neurologic origins for tinnitus. Localization of brain activity is now possible by means of positron emission tomography (PET), single photon emission computer tomography (SPECT), functional magnetic resonance imaging (fMRI), and magnetoencephalographic studies (MEG). This research, coupled with intensive study in recently developed animal models, increasingly suggests that tinnitus is most commonly a disorder that can originate in the peripheral and/or central nervous system and brain, and can undoubtedly be triggered by injury to the ear.
Explore This Issue
December 2008Although there is no cure for tinnitus, research from around the world is probing tinnitus’s causes, potential therapies, and management. This intensive work is translating into successful tinnitus management: Up to 85% of treated patients cite a significant incidence of relief. But the perception of tinnitus is a very personal experience.
Tinnitus Components
Experts in tinnitus cite three major components of tinnitus: acoustic, affective, and motor response to the tinnitus sensation, all of which are attention-based. The three interact with each other to varying extents. For example, there is evidence that stress can worsen tinnitus and that tinnitus can interfere with a person’s ability to concentrate. There is also research concluding that tinnitus is caused by neural plastic changes, that there are regions of the brain where tinnitus-related activity has been identified, that there are clues regarding how hearing loss causes brain changes that underlie tinnitus, and that animal studies demonstrate that excessive sound stimulation causes chronic changes in neural activity in the auditory centers of the brain.
Experts recognize that the cascade of psychophysiologic and psychophysical mechanisms underlying tinnitus mandate a multidisciplinary approach incorporating a strong mind-body component. Otologic surgeons are now venturing to study stress, the brain function response, and consciousness. I never thought, as an otologist and ear researcher, that I would be getting involved in areas that border on behavioral neurology and the neuropsychological, said Abraham Shulman, MD, Director of the Martha Entenmann Tinnitus Research Center in Brooklyn, NY, who, with his group, including audiologist Barbara Goldstein, PhD, coined the term tinnitology. But that is where the study of tinnitus has led us.
Operative Theories: Changes
There are presently several competing theories on the origins of tinnitus, all pertaining to changes in the auditory system. The nature of those accompanying changes, however, is the subject of these operative theories.
The first theory is that in patients with tinnitus, there is an increase in neural activity in the auditory system. This theory, said James A. Kaltenbach, PhD, Professor of Otolaryngology at Wayne State University in Detroit, maintains that neurons are firing at a higher rate, similar to the way they respond when sound is presented. There is much supporting evidence for this theory from electrophysiological studies in animals and imaging studies in human subjects.
A second view maintains that an increase in neural synchrony in the brain underlies tinnitus. Tinnitus is hypothesized to be a dysynchronous signal that can arise anywhere in the peripheral and/or central nervous system and uses the auditory system to express its dysfunction.
A third view holds that tinnitus is caused by a reorganization of the frequency map or a change in frequency representation. When part of the input is removed from the cochlea, as often occurs when there is sensorineural hearing loss, the corresponding part of the auditory cortex adopts sensitivity to adjacent, still-intact frequencies. The result is an expanded representation of frequencies bordering on the damaged frequencies of hearing loss. Some investigators believe that overrepresentation or reorganization gives rise to the percept of tinnitus.
A fourth theory is based on postulated temporal changes in the firing of neurons in the auditory pathway.
Neuronal Activity Changes: Causes and Implications
It is generally believed that in subjects with tinnitus, the change in neuronal activity is caused by a shift in the balance of excitatory and inhibitory impulses.
First, research shows that damage to the inner ear, such as that resulting from noise or aging, is associated with a reduction in inhibitory transmitters, especially glycine (at the brainstem level) and γ-amino butyric acid (GABA, in the midbrain and auditory cortex). Depleting these inhibitory neurotransmitters thus causes a disinhibitory effect: Neural activity increases and leads to tinnitus.
The second component causing neuronal changes is the increase in excitatory neurotransmitters, most notably glutamate and acetylcholine, in some structures.
The implications of these changes have led to several avenues of exploration in developing tinnitolytic therapies.
Treating and Managing Tinnitus: Where Do We Go from Here?
A multimodal, multidisciplinary approach to treating and managing tinnitus is generally employed. Accurate diagnosis of the etiology and classification of tinnitus, its types and subtypes, as well as related conditions identified in evaluation, are imperative for appropriate and effective recommendations for care: Medical significance of the disorder varies according to the individual patient.
Therapies for tinnitus currently can be categorized as pharmacologic, behavioral, acoustic-physical, and combinations of the above.
Pharmaceuticals are a first-line therapy followed by instrumentation. Drugs used in tinnitus largely target the depression and anxiety that accompany the disorder. Agents used to varying extents include antidepressants, anticonvulsants, antihistamines, dexchlorpheniramine, antiarrhythmics, anesthetics, and the rheologic agent pentoxifylline. The tinnitus itself is usually not reduced or eliminated by the pharmacologic agents, but the effects seem to attenuate the patient’s annoyance. In a select cohort of patients with subjective idiopathic tinnitus (SIT) of central-type severe disabling tinnitus, gabapentin demonstrated safe and effective relief, but this is controversial. Although developing test drugs to reverse neuronal changes-those of neural activity, neural synchrony, and frequency map reorganization-is an obvious direction for exploration, the problem to date is that blocking activity in the auditory system is difficult to achieve without also blocking activity in other vital brain areas.
Psychological counseling is beneficial for a number of reasons. First, it may be used to reorient associations the individual has with the tinnitus signal such that a negative effect can be alleviated to a more neutral response, similar to the way patients are taught to manage chronic pain. Combining counseling, sound therapy (partial masking), and education can be highly effective in neutralizing a patient’s emotional reactions to tinnitus percepts.
Patients are sometimes counseled to avoid tinnitus-causing agents (such as salicylates). Some groups suggest that patients try a step-and dose-wise exploration of alternative therapies, including acupuncture, hypnotherapy, vitamins, and herbs such as gingko biloba extract.
Acoustic therapies (instrumentation) aim at masking or partially masking the tinnitus, or influencing the way the central nervous system works. Instrumentation has advanced for tinnitus patients who have near-normal hearing, mild high-frequency hearing losses, hyperacusis, and high-frequency tinnitus. Effective therapies include masking devices, hearing aids (for those with higher-level hearing loss), and acoustic (filtered music) therapy. If the aforementioned neural changes (increased activity, synchrony, and frequency-map reorganization) are triggered by damage to the inner ear or by hearing loss (regeneration from selectively damaged outer hair cells appears to be a root cause), stimulating the auditory system in a way that better restores activity to the damaged area may have the effect of reversing the plasticity. Instead of neurons remaining hyperactive, oversynchronized, or overselective to certain frequencies, directly stimulating the ear with frequencies that span the frequency range of the hearing loss might diminish those measures of change. In animal studies testing this hypothesis, data seemed to suggest that, in fact, that is what happens: In those with less than severe hearing loss, who have a high-pitched or high-frequency hearing loss similar to the tinnitus, and who still have residual function, stimulation of functional areas demonstrates that all three measures of change are diminished.
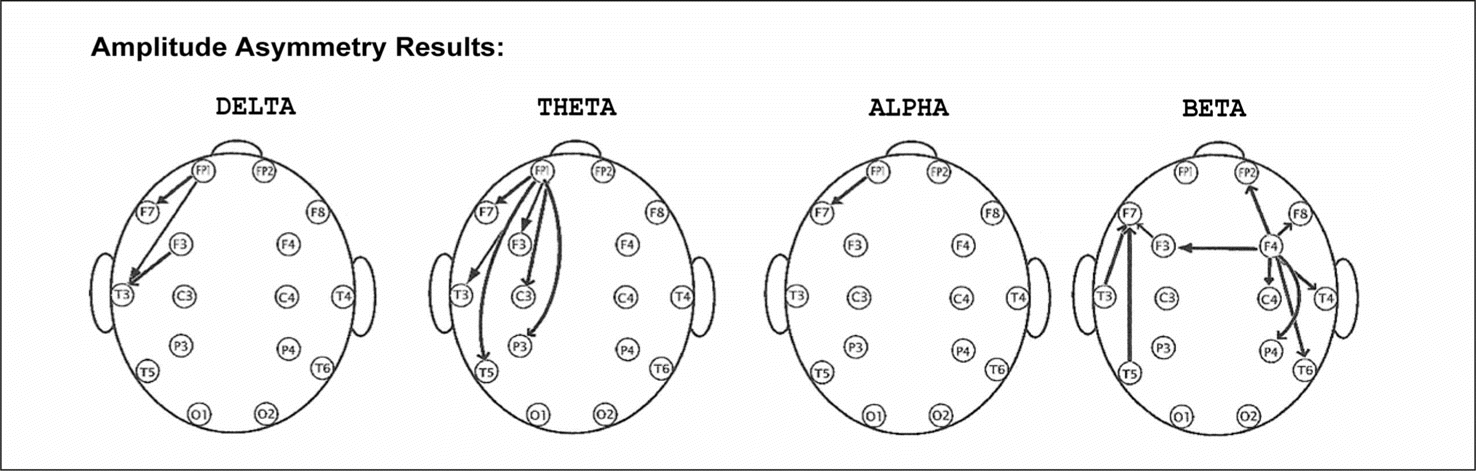
Other acoustic-physical therapies include surface quantitative electroencephalography (QEEG), which uses digital technology to measure electrical patterns on the scalp that reflect cortical activity (Figure 1). QEEG provides insight into underlying cellular, neuronal and interneuronal substrates involved in brain rhythms and their affect in tinnitus production.
Magnetoencephalography (MEG) (Figure 2) is being used investigatively in a small group of patients to identify tonotopically accurate cortical sites for electromagnetic stimulation. However, MEG is not yet not approved or available as a clinical treatment.
In most people with hearing loss, there are probably perturbed hair cells sending an abnormal signal, said Michael D. Seidman, MD, Director of the Division of Otologic and Neurotologic Surgery and Medical Director of the Center for Integrative Medicine at Henry Ford Health System in Detroit. The intervention works by using both fMRI and, more specifically, MEG. Essentially, the intracranial hot spots that correlate to the pitch of the patient’s tinnitus are targeted, and that sound is played back to the patient so the team can observe where the brain lights up. If I can get into the cortex, or better yet into limbic system, and change the patient’s perception of that symptom by perturbing the signals, I can perhaps improve their perception, Dr. Seidman said.
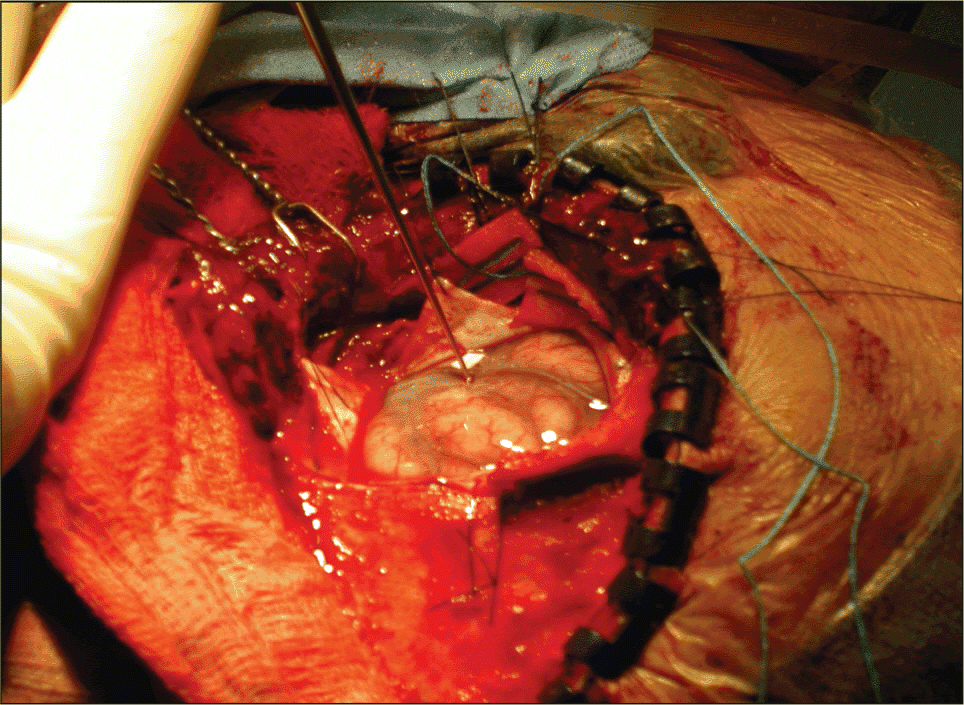
Investigations of electrical stimulation are promising but have yielded mixed results to date. The challenge is determining how to target the specific nerve population that controls the neural activity. Accurate targeting is difficult at this stage, is relegated more to trial and error, and requires precise electrode placement. There is also increasing (yet somewhat equivocal) evidence that individuals with cochlear implants and brainstem implants experience tinnitus suppression with electrical stimulation. Research shows that about 50% of patients with cochlear implants experience improvement of their tinnitus.
Advising the Patient with Tinnitus
Although most treatments are concerned with the auditory component of tinnitus, the emotional and attentional components are generally considered to be the most treatable.
We don’t have the magic bullet to knock out the tinnitus signal, said Dr. Kaltenbach, but we have a lot in our armamentarium to help tinnitus sufferers adapt and cope.
Patients will have more trouble coping on their own, as opposed to going to a tinnitus clinic. Any treatment from a concerned provider has been shown to offer a benefit to patients; investigators and clinicians are unclear as to whether that pertains to actually reducing the tinnitus or just supplying psychological support.
Experts agree that the very worst thing for patients is to tell them that there is no cure, there is nothing that can be done for them, and they will just have to learn to live with it. It is clear that a great majority of providers still give patients this negative feedback because by the time patients find the tinnitus experts, they often relate these unfortunate stories. Experts agree that even advising patients of the possibility of trying different modalities and combinations of therapies means something to them. (See Resources.) I cannot overemphasize the importance of avoiding negative counseling, said Pawel J. Jastreboff, PhD, ScD, MBA, a neuroscientist, professor, and Director of the Tinnitus and Hyperacusis Center at Emory University in Atlanta.
Certainly, patients who suffer from severe, disabling tinnitus should be referred to specialized clinics. Clinical information, combined with the basic science of brain and auditory function, is crucial in treating these challenging cases.
The concept that there will be a single drug or device that will cure all symptoms does not fit with what we know about the brain function, said Dr. Shulman. At this point it is important to focus on the positive findings for diagnosis, the positive findings for medical significance, and a rationale for therapy that has arisen from the overall body of investigative work.
Resources
For practitioners and patients:
- The Consumer Handbook on Tinnitus Richard S. Tyler, ed. Harris Communications, 2008.
- Save Your Hearing Now: The Revolutionary Program That Can Prevent and May Even Reverse Hearing Loss Michael D. Seidman, MD, and Marie Moneysmith. Wellness Central, 2007.
For practitioners:
- Tinnitus Diagnosis/Treatment Abraham Shulman, Jean Marie-Aran, Jeurgen Tonndorf, Harald Feldmann, Jack A. Vernon. Lea & Febiger, 1991; Singular Publishing Group, Inc. 1997; Martha Entenmann Tinnitus Research Center, Inc., 2004.
- Tinnitus: Treatment and Relief Jack A. Vernon. Allyn & Bacon, 1997.
- Tinnitus: Theory and Management James B. Snow. BC Decker Inc., 2004.
- Tinnitus: Pathophysiology and Treatment (volume 166) Aage R. Moller, Berthold Langguth (editors). Elsevier Science, 2007.
Additional References
- Bowyer SM, Seidman M, Elisevich K, et al. MEG Localization of the putative cortical generators of tinnitus. In: Cheyne D, Ross B, Stroink G, Weinberg H (eds). International Congress Series: New Frontiers in Biomagnetism: Proceedings of the 15th International Conference on Biomagnetism, Vancouver, BC, Canada, August 21-25, 2006:33-6.
- Bowyer SM, Seidman MD, Moran JE, et al. Coherence analysis of brain activity associated with tinnitus. In: Yokosawa K (ed). Biomagnetism-Transdisciplinary Research and Exploration. Proceedings of the 16th International Conference on Biomagnetism, Sapporo, Japan, August 25-29, 2008; in press.
- Daftary A, Shulman A, Strashun AM, et al. Benzodiazepine receptor distribution in severe disabling tinnitus. Int Tinnitus J 2004;10(1):17-23.
- Jastreboff PJ. Phantom auditory perception (tinnitus): mechanisms of generation and perception. Neuroscience Research 1990;8:221-54.
- Seidman MD, De Ridder D, Elisevich K, et al. Direct electrical stimulation of Heschl’s gyrus for tinnitus treatment. Laryngoscope 2008;118(3):491-500.
- Shulman A. A final common pathway for tinnitus-medial temporal lobe system. Int Tinnitus J 1995;1:115-26.
- Shulman A, Avitable MJ, Goldstein B. Quantitative electroencephalography-Power analysis in subjective idiopathic tinnitus patients: a clinical paradigm shift in the understanding of tinnitus. An electrophysiologic correlate. Int Tinnitus J 2006;12(2): 121-32.
- Shulman A, Goldstein B. Tinnitus dysynchrony theory: a translational concept for diagnosis and treatment. Int Tinnitus J 2006;12(2): 115-20.
©2008 The Triological Society
Leave a Reply