A man with moderate dementia who is living in a nursing home is diagnosed with laryngeal cancer. The man is still able to talk and interact with other people. But he doesn’t know what year it is and is unable to make decisions on his own.


Otolaryngologists with a desire to broaden their careers beyond traditional medical practice have several options. Programs exist that can open doors into medical leadership, health policy work, clinical and outcomes research and public office. Opportunities are available at all stages of a physician’s career. Here’s a look at a handful of programs that aim to provide physicians with the tools they need to take their careers in a new direction.

In my January 2011 column (“A Seller’s Market: How to prepare your practice for sale to a hospital”), I described the growing trend of physicians selling their practices to hospitals and large health systems and then working for the hospital or health system. This trend is expected to continue in full force through 2012. As I noted in my January article, the physician’s post-sale arrangement is the driver for the growth of the physician’s practice within the hospital or health system.

For residents embarking on their professional careers or physicians changing a career, navigating the many issues involved in making a decision that will significantly affect both their professional and personal lives can be daunting and challenging. To provide some guidance, practicing physicians with many years of experience in their respective careers discussed these issues during a session held here Sept. 13 at the 2011 American Academy of Otolaryngology–Head and Neck Surgery (AAO-HNS) Annual Meeting.

It can be difficult to launch a career as a physician–scientist, especially when budget cuts are making research funding harder to find—and this is doubly true for a small specialty like otolaryngology. That challenge is the reasoning behind the Triological Society’s grant programs. The society, which has awarded more than $2.5 million in grants since 1994, promotes research into the causes and treatments of ear, nose and throat diseases.

Balancing the risks and benefits of concurrent reirradiation and chemotherapy for recurrent head and neck cancers is difficult for physicians at even the most experienced centers. Research recently published in Cancer, however, suggests that selection of patients who may benefit from this therapy should be based on the patient’s previous treatment and the amount of time that has elapsed since initial treatment…

Ten years have passed since the U.S. was attacked on September 11, 2001 and six since Hurricane Katrina slammed into the Gulf Coast. And, while disasters of that magnitude are rare, hundreds of smaller-scale disasters occur every year, including tornadoes, blizzards, fires, earthquakes, airline crashes and chemical spills.

Most microvascular and reconstructive free-flap head and neck surgeons experience at least moderate professional burnout, according to a study published in October 2010 in the Archives of Otolaryngology and Head and Neck Surgery.
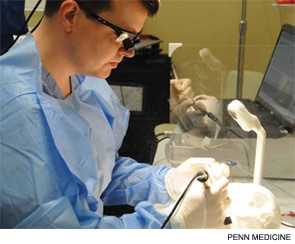
In May, Marcelo Antunes, MD, chief resident of otorhinolaryngology-head and neck surgery at the University of Pennsylvania, was able to practice bilobed flaps on pig’s feet at an ORL Rising Chief Boot Camp held at Penn Medicine Clinical Simulation Center in Philadelphia. While he had previously experienced medical simulation during his otolaryngology residency, the boot camp put the methodology in proper context for Dr. Antunes, who is particularly interested in facial plastics.