WASHINGTON, DC-At its annual meeting, the American Academy of Otolaryngology-Head and Neck Surgery released its long-awaited multispecialty practice guidelines for treatment of adult rhinosinusitis.
Explore This Issue
November 2007The ailment affects one in seven adults, has a profound effect on the quality of life, and costs the health care system almost $6 billion every year, said Richard M. Rosenfeld, MD, of the Department of Otolaryngology at State University of New York Downstate Medical Center in Brooklyn, who was chairman of the guidelines panel and lead author of the guidelines. The panel was composed of members of a number of medical specialties: allergy, emergency medicine, family medicine, health insurance, immunology, infectious disease, internal medicine, medical informatics, nursing, otolaryngology, head and neck surgery, and radiology.
Beyond its financial impact, sinusitis is responsible for 20% of all antibiotics prescribed in the United States, as well as half a million surgical procedures each year.
Characteristics of the Guidelines
Considerable practice variations exist among the physicians who treat sinusitis, and although there is no one absolutely correct way to proceed, some practices are better and more effective than others, said Dr. Rosenfeld. Therefore, the guidelines consist of 17 evidence-based statements with associated levels of statement strength-for example, strong recommendation, recommendation, recommendation against, or optional.
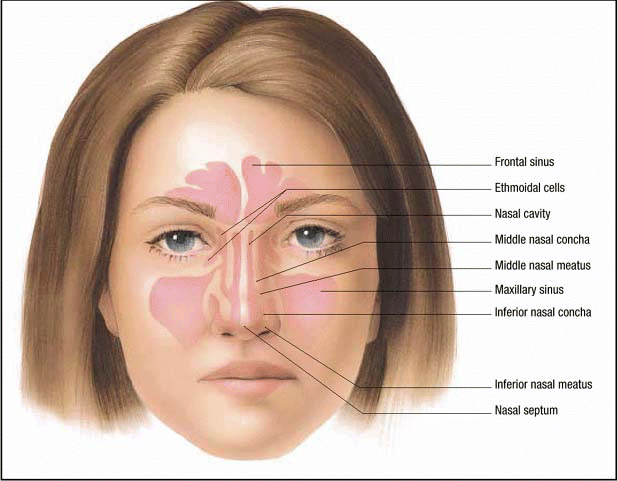
The guidelines are targeted toward patients aged 18 or older with a clinical diagnosis of uncomplicated rhinosinusitis. Rhinosinusitis is defined as symptomatic inflammation of the paranasal sinuses and nasal cavity. The term rhinosinusitis is preferred because sinusitis is almost always accompanied by inflammation of the contiguous nasal mucosa. When the ailment is called uncomplicated it means that there is no inflammation outside the paranasal sinuses and nasal cavity at the time of diagnosis.
Rhinosinusitis can be further classified by duration as acute (less than 4 weeks), subacute (4 to 12 weeks), or chronic (more than 12 weeks, with or without acute exacerbation).
Most acute rhinosinusitis begins when a viral upper respiratory infection (URI) extends into the paranasal sinuses, which may be followed by bacterial infection. About 20 million cases occur each year, which makes it one of the most common conditions that send people to the physician’s office. Its importance in health care relates not only to its prevalence but also to the potential for rare but serious sequelae: meningitis, brain abscess, orbital cellulitis, and orbital abscess.
A strong recommendation means that a treatment’s benefits clearly exceed the harms-or that the harms clearly exceed the benefits in the case of a strong negative recommendation-and that the quality of the supporting evidence is excellent. Clinicians should follow a strong recommendation unless there is a clear and compelling reason for an alternative.
A recommendation means that the benefits exceed the harms-or the reverse for a negative recommendation-but the quality of evidence is not as strong. Clinicians should generally follow a recommendation but should remain alert to new information and be sensitive to patient preferences.
An option means that either the quality of the existing evidence is suspect or that well-done studies show little clear advantage of one approach over another. Clinicians should be flexible in decision making about appropriate practice. Although they may set bounds on alternatives, patient preference should have a substantial influencing role.
If no recommendation is made, it means that the committee found no pertinent evidence and an unclear balance between benefits and harms. Clinicians should feel little constraint in decision making and be alert to new published evidence that clarifies the balance of benefit and harm. Patient preference should have a substantial influencing role.
Guidelines in a Nutshell
The guidelines emphasize appropriate diagnosis, and provide management options that include observation, antibiotic therapy, and additional testing. The guidelines include:
- Distinguishing acute bacterial sinusitis from that caused by colds, viruses, and non-infectious conditions. Strong recommendation.
- Defining acute sinusitis as lasting up to four weeks with purulent nasal drainage accompanied by obstruction, facial pain, pressure, fullness, or all. Strong recommendation.
- Eschewing X-rays. Recommendation.
- Prescribing symptomatic relief for viral rhinositis. Optional because randomized trials had limited cohorts and an unclear balance of benefit and harm.
- Observing without antibiotics (but assuring follow-up) for selected patients who have mild illness. Optional because double-blind, randomized trials had heterogeneous populations based on diagnostic criteria and illness severity. Benefit and risk were about the same.
- Prescribing symptomatic relief for acute bacterial rhinosinusitis. Optional because randomized trials were conducted with heterogeneous populations and diagnostic criteria. Outcomes showed a balance of benefit and harm.
- Using amoxicillin as first-line therapy for seven days. Recommendation.
- Distinguishing between chronic sinusitis (lasting 12 weeks or longer) and recurrent acute sinusitis (four episodes per year with no symptoms in between) by means of CT scan, nasal endoscopy, and allergy assessment. Recommendation, although nasal endoscopy is an option, despite expert opinion of benefit over harm.
- Encouraging patients to stop smoking and to use saline nasal irrigation. Recommendation.
Observation Option
Dr. Rosenfeld told the audience that some physicians might be reluctant to use the observation option for acute bacterial rhinosinusitis because they (as well as their patients) believe that bacterial illnesses should be treated with antibiotics. These barriers can be overcome with educational pamphlets and information sheets that outline the favorable natural history of nonsevere bacterial rhinosinusitis, the moderate incremental benefit of antibiotics on clinical outcomes, and the potential adverse effects of orally administered antibiotics, especially induced bacterial resistance.
He added that some patients and clinicians might object to amoxicillin as first-line therapy and cited the well-known false belief that newer and more expensive antibiotics are necessarily more effective. However, randomized trials do not support the benefit of one antibiotic over another for initial empirical treatment.
©2007 The Triological Society
Leave a Reply