As summer draws to a close, the warm-weather message to wear sunblock and shield your skin from UV rays quiets down—but the risk of developing skin cancer remains. ENToday spoke to several skin cancer experts, who shared some tips for evaluating hard-to-diagnose lesions on the head and neck and offered a look at new treatments under investigation.
Explore This Issue
September 2006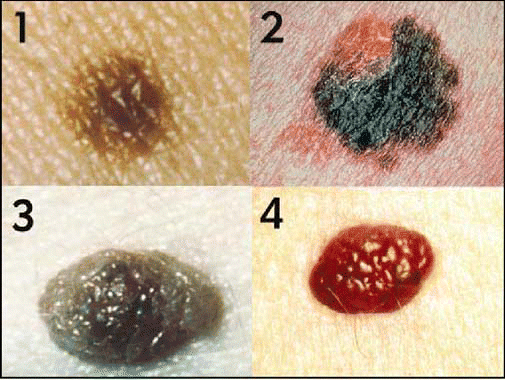
There are three main types of skin cancers found on the head and neck: basal cell carcinoma (BCC), squamous cell carcinoma (SCC), and melanoma. “BCC occurs most frequently, accounting for about 65 to 70 percent of skin cancers,” said Christopher O’Brien, MD, Director of the Sydney Cancer Centre in Australia. “It is usually found on sun-exposed areas of the face—around the cheeks and nose and the inner angle of the eyes and ears.”
Twenty-five to thirty percent of patients have SCC that is usually found on the lower lip and ears. “BCC and SCC are more prevalent in 60+ males of fair complexion,” said Dr. O’Brien. “Although melanoma is seen throughout all of the adult decades, it is more likely to affect younger patients in their 30s and 40s than BCC and SCC.” Skin cancer can also develop in dark-skinned people and people lacking significant sun exposure. Certain patient groups, such as organ transplant recipients, immunosuppressed patients, long-term survivors of childhood and adolescent cancers, and those with xeroderma pigmentosum are at higher risk for developing skin cancers.
Diagnosis: Biopsy Is Gold Standard
Fortunately, BCC and SCC can be treated and cured if detected early. Even melanoma has a high cure rate when diagnosed at the in situ stage, according to the American Cancer Society (ACS). “The gold standard for a definitive diagnosis is still biopsy of the primary with postoperative margin assessment [POMA],” said Randal Weber, MD, Professor and Chairman of the Department of Head and Neck Surgery at University of Texas M.D. Anderson Cancer Center in Houston. “Shave biopsies of pigmented lesions should never be performed.”
For small, local skin cancers, most otolaryngologists–head and neck surgeons do an excisional biopsy incorporating the full thickness of the skin and a minimum of surrounding normal skin. Although the biopsy is done in an office-based surgical procedure using local anesthesia, the tissue must be sent out to a pathologist for verification.
“Most patients will see their primary care physician or a dermatologist first if they suspect skin cancer. Consequently, most otolaryngologists tend to see patients with more advanced stage, larger cutaneous cancers that may have metastasized.” – —Christopher O’Brien, MD
A punch biopsy, which removes a deeper sample of all skin layers, can be used for larger tumors by taking the sample from the most raised area and properly orienting the biopsy specimen for the pathologist. If palpable regional lymph nodes are present, then fine needle aspiration may be necessary. Depending on the extent of the disease and presence of symptoms of local or distant metastases, a chest X-ray and CT, PET, and/or MRI may also be needed. The use of laser scanning devices and ultrasound for biopsy are still in the experimental stage.
Multidisciplinary Approach to Treatment Key
“Most patients will see their primary care physician or a dermatologist first if they suspect skin cancer,” said Dr. O’Brien. “Consequently, most otolaryngologists tend to see patients with more advanced stage, larger cutaneous cancers that may have metastasized.” These patients require a multidisciplinary approach to their treatment that involves not only the head and neck surgeon, but also a surgical dermatologist, facial plastic and reconstructive surgeon, dermatopathologist, and surgical, medical, and radiation oncologists.
“Through multidisciplinary consultation, we can offer patients a wider armamentarium of treatment modalities in order to do what’s best for them,” said Hugh Greenway, Jr., MD, Chairman of Dermatologic/Mohs Surgery and Director of Cutaneous Oncology and the Melanoma Center at Scripps Clinic in San Diego, Calif. Treatment plans will depend on the location, size, and stage of the cancer, status of tumor borders, risk factors for recurrence, and previous irradiation, as well as the patient’s age and general health.
“The primary treatment for cutaneous cancer is excisional surgery, with radiotherapy used as an adjuvant if negative pathological prognostic factors are identified,” said Dr. O’Brien. “Chemotherapy does not have a role in the standard management of skin cancers of the head and neck.”
Treatment Guidelines
Standard treatment of BCC and SCC is outlined in the National Comprehensive Cancer Network’s (NCCN) Clinical Practice Guidelines in Oncology, Basal Cell and Squamous Cell Skin Cancers (available online at www.nccn.org/professionals/physician_gls/PDF/nmsc.pdf ). In general, low-risk local BCC requires an excision with narrower clinical margins (2.0–3.0 mm) than low-risk local SCC (4.0–5.0 mm), when there is no lymph node involvement. If there are palpable regional lymph nodes in SCC, then a regional lymph node dissection may be necessary.
Because removing all cancer cells to minimize the chance of cancer regrowth is as important as achieving optimal cosmetic results from surgery on the head and neck, Mohs micrographic surgery is often the treatment used for patients with localized BCC and SCC. Clinical studies have shown that there is a five-year cure rate of up to 99% for these lesions. For patients with aggressive SCC that demonstrates perineural invasion or parotid gland or cervical metastasis, a head and neck oncologic surgeon and radiation oncologist should be consulted.
“The gold standard for a definitive diagnosis is still biopsy of the primary with postoperative margin assessment. Shave biopsies of pigmented lesions should never be performed.” – —Randal Weber, MD
“This technique requires that the Mohs-trained physician, most often a dermatologist, serve as surgeon, pathologist, and reconstructive surgeon, all at the same time,” said Dr. Greenway. “As each layer of tissue is excised, it is immediately examined under a microscope and color-coded with immunostains for mapping purposes. Tissue is continually removed and examined, one layer at a time, down to the roots, until the samples are cancer-free. This spares the surrounding normal skin tissue and ensures 100-percent clear margins. Reconstruction of the wound can be done at the same time.”
Guidelines for the treatment of melanoma are found in the NCCN’s Clinical Practice Guidelines in Oncology, Melanoma (available online at www.nccn.org/professionals/physician_gls/PDF/melanoma.pdf ). Treatment involves a much wider excision (0.5–2.0 cm), and sentinel node biopsy is recommended for melanomas >1.0 mm. If the sentinel node is negative, then regional lymph node dissection is not indicated. If it is positive, then a completion lymphadenectomy of the nodal basin is recommended. The NCCN-recommended adjuvant options include a clinical trial, high-dose adjuvant interferon alfa-2b or observation for patients with either localized melanomas (>4.0 mm) who are at significant risk for recurrence or positive nodes. CO2 laser ablation may be used in selected patients.
Promising New Treatments
Although BCC and SCC are commonly treated with surgery and radiation, local therapy, such as 5-fluorouracil (5-FU) (Effudex) and imiquimod (Aldara), are now being considered. 5-FU is a standard chemotherapy drug and imiquimod is an immune response modifier that promotes the release of cytokines that help to destroy cancer cells; both are manufactured as a cream, which makes them easy to use.
“5-FU and imiquimod are being applied topically to treat AK [actinic keratoses], superficial BCC, and Bowen’s disease,” said Dr. Greenway. A randomized phase III clinical trial is under way to see how well topical imiquimod works compared to surgery in treating BCC.
“One of the other promising areas of investigation involves the use of varying electrical pulses combined with intralesional drug therapy to treat non-melanoma skin cancers,” said Dr. Greenway. “We have been involved with electrochemotherapy (ECT) utilizing bleomycin sulfate intralesionally with the electrical current in BCC. In our study, six out of seven patients demonstrated complete cure, with a partial response for the other patient.”
Attacking Cancer with Light, Chemo
“Photodynamic therapy (PDT) is also being used to treat AK and some non-melanoma skin cancers in clinical trials,” said Dr. Weber. According to the National Cancer Institute, PDT involves a two-step process that uses a photosensitizer drug and light to create a chemical reaction that destroys only the cancer cells. For skin cancer, the drug is administered topically and is absorbed by both healthy and abnormal cells. After a predetermined period of incubation, the photosensitizer is activated by a specific wavelength of light (from a laser or other source, such as light-emitting diodes) that is directed at the cancer and produces oxygen that kills the abnormal cells. Simultaneously, PDT damages the blood vessels in the cancer, thereby cutting off its source of nutrients and it also activates the immune system to attack the cancer cells.
“Through multidisciplinary consultation, we can offer patients a wider armamentarium of treatment modalities in order to do what’s best for them.” – —Hugh Greenway, Jr., MD
“At M.D. Anderson, we have a clinical trial underway to assess the effectiveness of using gefitinib [Iressa] for treating locally aggressive and metastatic SCC,” said Dr. Weber. Gefitinib is a chemotherapy drug currently approved for patients with non-small-cell lung cancer.
“In Australia, where two out of every three people will be affected by skin cancer over their lifetime, we are conducting a prospective randomized clinical trial to see if postoperative concurrent chemoradiotherapy results in improved cure rates compared with postoperative radiotherapy alone in SCC,” said Dr. O’Brien.
Vaccine Trials
Large phase III clinical trials using peptides, gangliosides, and whole-cell tumor antigens are ongoing. Whereas ganglioside vaccines aim to stimulate a B-cell response, peptide vaccines are intended to stimulate T-cell based responses to tumor-specific antigens expressed on the surface of cells through a major histocompatibility complex class-I restricted process.
The NCCN recommends that patients with melanomas 4.0 mm be offered melanoma vaccine clinical trials. Ultimately, the goal is to develop an effective vaccine with a low toxicity that can be given to those at high risk for melanoma or administered to those with high risk of recurrence of melanoma after surgical resection.
Although new treatments are in the pipeline, “it is critical that ENTs be vigilant when it comes to identifying patients with skin cancers, especially high-risk skin cancers, on the head and neck,” said Dr. Weber. “Some of the signs and symptoms of certain skin cancers are subtle, so you should always ask your patients during the exam if they have noticed anything unusual on the skin of their head and neck and scalp; otherwise, they might not mention it or you might miss it.”
Identifying Skin Cancers on the Head and Neck
- Basal cell carcinoma (BCC) appears as a small, slow-growing pale patch of skin that produces a central “dimple” and eventually an ulcer that may scab over and then reulcerate; some BCCs show color changes. Although most BCCs do not metastasize, 35% to 50% of people diagnosed with one BCC will develop a new skin cancer within five years, according to the ACS.
- Squamous cell carcinoma (SCC) is similar in presentation, but tends to be more aggressive and have greater metastatic potential. It may start as actinic keratoses (AK), a precancerous lesion caused by too much sun exposure that appears as a small pink or flesh-colored rough spot on the skin. Bowen disease is SCC in situ and is larger, redder, and more scaly and crusty in appearance. Areas of SCC do not heal and can become open sores.
- About 111,900 new cases of melanoma will be diagnosed in 2006, representing almost a 10% increase since 2005, estimates the American Academy of Dermatology (AAD). Melanomas typically produce dense blue or black discolorations of the skin, like moles, and readily metastasize. If these pigmented lesions change in size or color or begin to bleed, it may signify trouble. (See “ABCDs of Melanoma” for more information on identifying these skin lesions.)
- Melanomas on the scalp may be hidden by hair and easily overlooked, as can those that are non-pigmented. Merkel cell carcinoma, which is a rare non-melanoma skin cancer that generally occurs in older patients and appears pink without pigment, may also be missed.
ABCDs of Melanoma
Asymmetry: One half of a mole is different from the other.
Border Irregularity: The border of melanomas are usually ragged, notched, or blurred.
Color: Benign moles can be any color, but a single mole will be only one color. Melanoma often has a variety of hues and colors within the same lesion.
Diameter: While melanomas are usually greater than 6 mm (a pencil eraser) in diameter when diagnosed, they can be smaller. If a mole is different from others, or it changes, itches, or bleeds, even if it is smaller than 6 mm, see a specialist.
©2006 The Triological Society



Leave a Reply