Malignant fibrous histiocytoma (MFH) is the most common soft tissue sarcoma. Most of the time, it arises in the extremities and retroperitoneum, but it also occurs in the facial sinuses, nasal and oral cavities, nasopharynx, and soft tissues of the neck.
Explore This Issue
May 2009It is relatively uncommon in the head and neck (about 5 percent of the total), but when it does occur, it is usually in soft tissue or, rarely, in the mandible, said Erich Sturgis, MD, MPH, Associate Professor of Head and Neck Surgery and Epidemiology at M. D. Anderson Cancer Center in Houston. There are only about 500 sarcomas of the head and neck each year in the United States.
The disease occurs more commonly in whites than in blacks or Asians, and males develop it about twice as often as females. MFH has a wide age range (10-90 years), but it is most common from age 50 to 70.
Pathophysiology
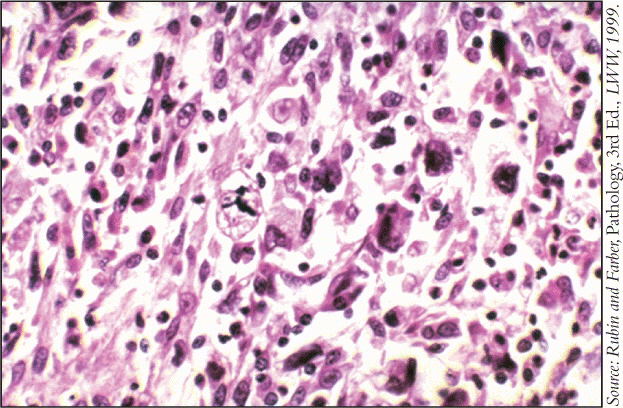
MFH has variable pathophysiology and many subtypes. Tumors contain both fibroblast-like and histiocyte-like cells in varying proportions, giving rise to five major subtypes: storiform/pleomorphic (most common); myxoid; giant cell; inflammatory (usually not seen in the head and neck); and angiomatoid-although the last may be a distinct, more indolent, disease. Dr. Sturgis said that most sarcoma pathologists think that MFH is poorly differentiated.
However, said David W. Clark, MD, of the Department of Otolaryngology-Head and Neck Surgery at University of Texas Health Science Center at Houston, Some people argue that the histiologic subtypes are no longer pertinent and that MFH represents a group of unclassifiable sarcomas, and hence is synonymous with pleomorphic undifferentiated sarcoma.
Myogenically differentiated tumors that suggest muscle origin can behave more aggressively, so a thorough pathology investigation is necessary to ensure accurate classification.
The cause of MFH is unknown, but it is believed that a genetic abnormality on the short arm of chromosome 19 or loss of chromosome 13 may play a role.
The disease also has been linked to radiation treatment for breast cancer, retinoblastoma, Hodgkin’s disease, nasopharyngeal carcinomas, and other head and neck malignancies.
Diagnosis
Patients often present with a painless soft tissue mass in the neck that, before biopsy, may be confused with lymphomas, other soft tissue sarcomas, and metastatic carcinomas. Those on the scalp are often mistaken for desmoplastic melanomas or atypical fibroxanthomas. Those arising in the nose, nasopharynx, and paranasal sinuses can be confused with other sinonasal malignancies.
Patients also may have an elevated eosinophil count, hypoglycemia, fever, and abnormal liver function tests.
The only definitive diagnosis is biopsy, but imaging studies are usually done first.
- MRI provides good contrast between tumor and muscle, excellent definition of the surrounding anatomy, and ease of imaging in multiple planes. It reveals an intramuscular mass with heterogeneous signal intensity on all pulse sequences.
- CT scan is preferred by some, but the definition between tumor and muscle is not as good. It typically shows a large, nonspecific, lobulated soft tissue mass with density close to that of muscle.
- Ultrasonography shows a well-defined heterogeneous mass, but the appearance of tumors on ultrasound is nonspecific. It can, however, facilitate directed needle biopsy.
Biopsy is all-important-and not at all straightforward. For accessible lesions of the upper aerodigestive tract, paranasal sinuses, or scalp, direct biopsy is appropriate. For inaccessible lesions, such as those in the neck, fine needle biopsy should be the first step. Core needle biopsy can usually definitively diagnose sarcoma, and often allows subtyping. If incisional or excisional biopsy is necessary, the surgeon must consider the approach carefully.
Treatment
Assuming a correct diagnosis, early and complete surgical excision is the best initial treatment. The higher the stage of the disease, the wider the margins must be. For larger tumors, preoperative radiation and/or chemotherapy can shrink the tumor.
In the head and neck, there are many vital structures in a confined area, said Dr. Clark. The classic mantra regarding margins is to resect to a new tissue plane, but with limited space and vital structures, this presents a challenge. Therefore, surgery for larger lesions, those of the skull base, and those adjacent to vital structures, such as the eye, can be quite morbid.
Patients with MFH often have had more than one episode before diagnosis, so the tumor is only partially resected, thus increasing the potential for recurrence and/or distant metastasis.
The usual chemotherapy agents include ifosfamide, high-dose ifosfamide with mesna to prevent hemorrhagic cystitis, cyclophosphamide, doxorubicin, vincristine, adriamycin, gemcitabine, and taxanes. Combination chemotherapy is almost always more effective then use of a single agent.
No one agent has emerged as the treatment of choice, said Dr. Clark. The rarity of the tumor precludes sufficient enrollment in controlled studies, which continues to be a significant limitation.
Tumor size, location, and histology are the major determinants of outcome, but patients with less aggressive myxoid tumors do not require systemic therapy, and patients with nonmyxoid disease are at significant risk for metastases.
MFH is not as sensitive to radiotherapy and chemotherapy as some other cancers, but multidisciplinary therapy must be offered for the overwhelming majority of patients. Salvage following initial treatment failure is difficult.
Prognosis
As with all cancer, the most important prognostic factors for MFH are tumor grade, size, and extent of metastasis, as well as histiologic subtype and surgical margins. About 20% of all cases are associated with previous radiation treatment.
At the January 2009 meeting of the Triological Society, a 40-year retrospective review of 95 MFH patients at M. D. Anderson Cancer Center was presented. It revealed that:
- Twenty-eight percent of patients had surgery alone, 26% had surgery with radiation, 17% had surgery plus chemoradiation, 13% had surgery plus chemotherapy, and 16% did not have surgery.
- After 34 months of follow-up, 36% of patients had recurrence after initial therapy, about three-quarters of which was local.
- Overall five-year survival for patients with MFH was 51%; disease-free survival was 44%.
- Worse survival correlated with being treated before 1990, as well as with larger tumors, tumor site, and previous radiation treatment.
Others have reported that tumor characteristics also affect survival: Patients with low-, intermediate-, and high-grade tumors have 10-year survival rates of 90%, 60%, and 20%, respectively. Tumors smaller than 5 cm at diagnosis (stage 1) have survival of 79% to 82%, those of 5 to 10 cm (stage 2) have rates of 62% to 68%, and tumors larger than 10 cm (stage 3) result in only 41% to 51% survival.
In general, prognosis is poor if the disease has metastasized to the lungs, lymph, or bone; complete tumor removal is not possible; the patient is very old and/or the tumor is very large; and the tumor is deep, rather than superficial.
Sometimes MFH is a second malignant neoplasm. The prognostic factors here have not been well described, but one observational study looked at 50 patients who had had breast cancer, Hodgkin’s disease, lung cancer, and melanoma. The average time between the first malignancy and MFH was 10 years, and half of the cases of MFH developed in irradiated fields. Two-year survival was 33%, and five-year survival was 13%.
Quality of Life
How radical and disfiguring is the surgery? It depends on the location, said Dr. Sturgis. If the tumor is in the scalp or the neck, quality of life and cosmesis may be reasonable. If it occurs in the paranasal sinus, the mandible, or elsewhere in the upper aerodigestive tract, depending on size, disfigurement and functional impairment can be more serious, although the damage can be somewhat repaired by reconstructive surgery.
I agree, said Shreyaskumar Patel, MD, Professor of Sarcoma Medical Oncology at M. D. Anderson Cancer Center. It depends on the exact location and extent of the tumor, which in turn determines the extent of surgery.
Quality-of-life issues for MFH are essentially the same as those for any head and neck cancer. There may be facial disfigurement, swallowing and/or speech deficits, xerostomia, and decreased ability to taste. If the tumor is in the neck, there may be some shoulder dysfunction, said Dr. Sturgis.
Dr. Patel added that there may be chronic pain.
Dr. Clark said that functional outcomes are of great concern. Returning to a normal life is the goal, so we try hard to preserve swallowing and speech, and we pay attention to cosmesis. But, having said this, we can’t lose sight of the goal of disease-free survival.
Virtually all soft tissue sarcomas are aggressive, added Dr. Sturgis, who stressed that patients should be treated in a major cancer center where an experienced sarcoma team is available for examination and treatment. These patients have no business being treated in the community.
©2009 The Triological Society
Leave a Reply