Untreated obstructive sleep apnea carries significant morbidity and mortality and has evolved into a public health problem, yet effective treatment remains elusive for many patients. Surgical treatments, oral applications, and the current gold standard treatment with continuous positive airway pressure (CPAP) work for some patients, but data indicate that up to 50% of patients are not successfully treated with these methods.
Explore This Issue
August 2009Part of the difficulty in developing an effective nonsurgical treatment is not the treatment itself, but the appropriate application and use of the treatment. What is highlighted by the current data on the efficacy of CPAP is that a treatment itself can confer a high degree of effectiveness, but if the patient does not use the treatment appropriately, its efficacy is compromised.
Philip Westbrook, MD, Emeritus Professor of Medicine at UCLA and Chief Medical Officer of Ventus Medical, Inc., in Belmont, CA, emphasized this point in discussing the need to develop alternative treatments. It is really the patient that treats the disease in chronic disease, he said. Because of that, if we prescribe a treatment that the patient won’t use, than that treatment is ineffective no matter how good it looks in the laboratory.
For a chronic condition such as sleep apnea, developing treatments that are effective in addressing the mechanism of disease as well as patient compliance requires both a deep knowledge of the pathophysiology of sleep apnea and the anatomy of the upper airway and an understanding of human psychology and behavior.
This is not a new idea, but one that underlies the development of two new therapies that have emerged to treat sleep apnea and will be applied to measuring the efficacy of these treatments.
PROVENT Therapy
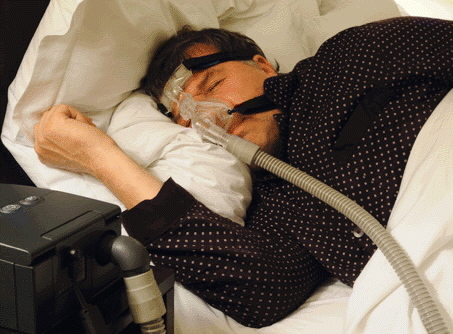
PROVENT therapy (Ventus Medical, Inc.) is one emerging alternative to the therapies currently used to treat sleep apnea. Unlike CPAP, which requires a machine to provide continuous positive airway to keep the nasal airway open during sleep, PROVENT therapy relies on the patient’s own breathing to keep the nasal airway open by using a device that uses nasal expiratory positive airway pressure (EPAP). Placed on each nostril, the device acts like a valve (and looks and feels like a small bandage on each nostril, according to Dr. Westbrook). The valves are open when inhaling to allow for nearly unobstructive airflow, but close when exhaling, directing air through small air channels to limit airflow and increase expiratory pressure.
Leave a Reply