Laryngomalacia is a congenital condition consisting of three anatomical abnormalities: short aryepiglottic folds, suprarythenoid redundant tissue, and an epiglottis that prolapses posteriorly during inspiration. The collapse of these tissues during inspiration causes breathing difficulties, and typically occurs in infants. (Another rare form is also observed in neurologically impaired adults.) Only a small percentage of children who experience laryngomalacia will require surgery. Currently, surgeons can choose among several techniques for infants with severe laryngomalacia who require surgery. Microdebrider-assisted supraglottoplasty is gaining favor as a preferred technique, according to two experts interviewed for this article.
Explore This Issue
May 2008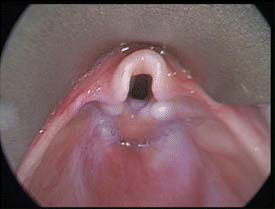
Laryngomalacia is the medical term for a floppy voice box. This is the most common cause of stridor and difficulty breathing in children. On inspiration, tissue from the supraglottis prolapses and obstructs the airway at the level of the larynx, explained William O. Collins, MD, a pediatric otolaryngologist at the University of Florida College of Medicine in Gainesville.
The vast majority of children (about 90%, Dr. Collins said) with this problem will outgrow it in less than two years. About 10% of children with this problem do not improve, with a very small number of these having severe symptoms that will require surgery to alleviate severe airway obstruction. We see hundreds of children with laryngomalacia each year, and only about 10 of them will need surgery, said George H. Zalzal, MD, Professor of Otolaryngology and Pediatrics at George Washington University and Division Chief of Otolaryngology at Children’s National Medical Center in Washington, DC. Dr. Zalzal is the first reported surgeon to use to the microdebrider for supraglottoplasty.
Indications for supraglottoplasty include severe symptoms of stridor and failure to thrive, with or without apnea. Flexible endoscopy should reveal severe laryngomalacia-that is, supraglottic collapse blocking the view of the vocal cords and endolarynx.
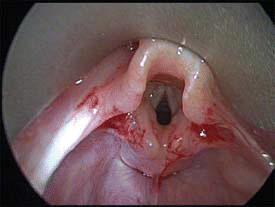
There should be no evidence of another airway lesion on bronchoscopy. This is a prerequisite for surgery, Dr. Zalzal noted. If an infant has laryngomalacia and other airway lesions, a supraglottoplasty alone would not be helpful.
Surgeons should be cautious about performing supraglottoplasty-or any surgery-on children with underlying neurological disease. These children don’t do as well as those without neurological disorders and are likely to require further surgeries, including a tracheostomy, Dr. Collins said.
Surgical Options
Surgical options have evolved from the original gold standard-tracheostomy-to less invasive supraglottoplasty using endoscopic technique. As endoscopic techniques have improved, so have methods for tissue removal, both doctors said.
Tracheostomy is the old-fashioned approach, but this doesn’t directly address the obstruction, Dr. Collins said. Tracheostomy has inherent risks and is less than ideal, especially with the current technologies we have available, he continued.
Supraglottoplasty involves trimming some of the redundant floppy tissue from the supraglottis or the area above the vocal cords. This can be accomplished with microinstruments such as microscissors and micro cup forceps (also called cold instrumentation). The CO2 laser represents a step forward, and the microdebrider has become the technique of choice for both Dr. Zalzal and Dr. Collins. Cold steel instruments are miniaturized instruments for grabbing the redundant tissue and resecting it. With the CO2 laser, the tissue is vaporized. The microdebrider is a small shaving instrument with an oscillating blade for tissue removal combined with suction to pull the tissue into the tip.
Which Technique to Use?
The microdebrider is one of several techniques for supraglottoplasty, Dr. Zalzal said.
All of these tools accomplish the same goal-that is, to remove redundant tissue causing obstruction. I can’t think of situations where a patient [with laryngomalacia] would be a candidate for one of these procedures and not another. The technique of choice depends on surgeon preference. To the best of my knowledge, there is no controversy about using the microdebrider. I trained with Dr. Zalzal using this instrument, and I have had good results, Dr. Collins commented.
The techniques all have advantages and disadvantages. Tracheostomy is uncomfortable for the patient and carries the risk of bleeding and lung damage with pneumothorax, and poses long-term risks as well. The tracheostomy tube can fall out or become plugged by patient secretions and mucus; infections can arise at the site of insertion, and the patient can develop scar tissue secondary to the tracheostomy tube. Cold instrumentation can cause increased bleeding. The laser technique has the advantage of hemostasis, coagulating blood vessels with little bleeding. However, with the laser, there is always the inherent risk of burning the patient or the staff, as well as the risk of an airway fire.
The main advantage of the CO2 laser is that it is very accurate and practically bloodless, Dr. Zalzal commented. The disadvantages are that it is time-consuming, carries the theoretical risk of fire, some patients have pain for a day or two after laser surgery, and the laser cannot be used with an endotracheal tube because of the risk of fire. Anesthesia for CO2 laser surgery becomes cumbersome because of the need to ventilate the patient, he added.
The microdebrider is a safe instrument in trained hands; there is no risk of airway fire, thermal damage, or associated burn to the tissues. Dr. Zalzal said that the biggest advantage of microdebrider-assisted supraglottoplasty is shortened surgical time-about 15 minutes shorter than with the CO2 laser. The microdebrider is practically painless, and it glides over any cartilage that is present-it does not cut the cartilage or burn it, like the laser, he said.
The main downside of the microdebrider is that its aggressive use can result in the removal of too much tissue; but in trained hands, this rarely, if ever, happens, Dr. Zalzal said. The microdebrider is well tolerated and is used in other types of laryngeal diseases, such as laryngeal papillomas, Dr. Collins added.
Training
Typically, a surgeon would be trained to use the microdebrider during his or her residency. At Dr. Zalzal’s institution, residents come from three medical schools; the division also has a fellowship training program. Once a resident becomes adept at suspension microlaryngoscopy and microlaryngeal instruments, he or she would then observe several cases done with a microdebrider. Then we would teach them where to cut, avoiding the interarytenoid area. Then they would perform their own cases, Dr. Zalzal explained.
Two types of microdebriders are currently on the market-one made by Medtronic and one by Gyrus. Neither Dr. Zalzal nor Dr. Collins has a commercial interest in these products.
More about Microdebriders
A microdebrider consists of three key components:
- Console;
- Handpiece;
- Blade.
The console is controlled by a foot pedal that determines the speed and direction of the rotating blade. The handpiece controls the blade and integrates suction to rapidly remove the debris. Suctioning tubes connect to the handpiece. The blade (or bit) can be smooth or serrated and comes in a variety of sizes; blades can be rotated in forward, reverse, or oscillating modes at various speeds.
The main risk of microdebriders is the possibility of removal of normal tissue, which can happen if overzealous suction pressure is used. The operator should always maintain adequate visualization of the blade or bur and be aware of using the instrument too aggressively.
Microbrider Applications
Studies have shown that the microdebrider can be an effective tool for diverse types of procedures. Researchers state that it is a convenient and efficient tool, with several advantages and only one identified risk-that is, inadvertent removal of normal tissue.
Obstructing airway lesions can be removed by the microdebrider, with the obvious goal of restoring oxygenation to the patient. These lesions may be seen in patients with lung cancer or in patients with certain benign conditions, such as postintubation tracheal stenosis, relapsing polychondritis, and Wegener’s granulomatosis.
Removal of the lesion may be diagnostic as well as palliative; therefore, before doing the procedure, determine whether the tissue needs to be preserved for pathological study.
The microdebrider has also been used for partial tonsillectomy. With traditional tonsillectomy, the capsule enclosing the tonsil is removed, exposing the throat muscles, large blood vessels, and nerves. In one series (Otolaryngol Head Neck Surg January 2005) physicians were able to remove 90% to 95% of the tonsils, leaving the capsule in place to protect the throat muscles, blood vessels, and nerves. In this series, patients treated with the microdebrider had less pain and swelling, as well as shorter recovery times, than those undergoing traditional tonsillectomy. Furthermore, microdebrider-treated patients were three times more likely not to require pain medication three days after surgery and almost twice as likely to resume normal activity at that time than patients treated with traditional tonsillectomy.
In addition to supraglottoplasty, other potential applications of the microdebrider include sinus surgery and microdebrider Eustachian tuboplasty. Preliminary results in these conditions are encouraging.
Caveat
Researchers caution that the tool can remove a great deal of tissue very quickly, so the operator must be aware at all times of the location of the blade and be alert to risks. Although the microdebrider is a promising tool, it should be used with appropriate respect and vigilance for potential complications.
Laryngoscope Highlights
Using a Portable Electromyography Device in Treating Spasmodic Dysphonia
Adductor spasmodic dysphonia (SD) is due to involuntary overcontraction of the thyroarytenoid muscles during speech. Currently, Clostridium botulinum bacterial toxin (Botox) is an effective treatment option when injected into the thyroarytenoid muscle, as it blocks the release of acetylcholine at the neuromuscular junctions, causing denervation of the thyroarytenoid muscle. Electromyography (EMG) monitoring is an essential component in the identification of the thyroarytenoid muscles during Botox injection when the percutaneous approach is used. Benjamin T. Jeffcoat, MD, and John M. Schweinfurth, in a How I Do It article, discuss using a handheld, audible-only EMG device as an efficient, safe method for identification of the thyroarytenoid muscle for Botox injection.
The investigators reviewed the charts of 38 patients who received intramuscular Botox injections in treatment of adductor SD over a three-year period; 13 met the inclusion criteria. Using the handheld, audible-only EMG monitor, Dr. Jeffcoat performed all injections. A missed injection was defined as no improvement in voice quality within two weeks following the injection; a successful injection was defined as subjective or objective improvement in voice quality within two weeks following the injection, for a duration of at least one month.
The portable EMG device was used to audibly monitor muscle activity during the procedure. Location of the thyroarytenoid muscle was confirmed by increased action potential density during phonation, which is audibly interpreted by the operator. When the position was confirmed, Botox was injected into the muscle.
The 13 patients in the study underwent a total of 113 injections. There were 13 missed injections, for a successful injection rate of 88.5%. One patient was noted to have had four missed injections, all on the same side; excluding this patient, the successful injection rate rose to 90.1%. There were no complications following any of the injections.
The authors enumerate the advantages of using the portable EMG monitor: the portable nature of the device allows the physician to take it from room to room; it is less expensive than oscilloscope EMG devices; and it does not require a neurologist to interpret the results, as the audible increase in recruitment ensures proper location of the thyroarytenoid muscle. As demonstrated in this study, the portable EMG device provides an acceptably low miss rate for Botox injection in treating adductor SD.
(Laryngoscope 2008;118:942-3)
Understanding the Biology and Treatment of Choanal Atresia
Choanal atresia (CA) is a congenital obstruction of the posterior nasal apertures. The incidence of CA is estimated to be about 1 in 5000 to 7000 live births. Unilateral defects are more common than bilateral ones, and the female-to-male ratio is about 2:1. Associated congenital anomalies can be found in up to 50% of CA cases, with CHARGE syndrome (coloboma, heart defects, CA, growth and mental retardation, genital and ear anomalies) being the most commonly described associated condition. Arthur S. Hengerer, MD, and colleagues prepared a study to review the basic science and embryology of CA, with emphasis on Dr. Hengerer’s experience, and to discuss the treatment of CA.
The researchers conducted a retrospective review of pediatric patients treated for CA by Dr. Hengerer over a 12-year period; the review yielded a total of 73 patients. Unilateral atresia was more common than bilateral atresia by a ratio of 1.6:1, but the incidence in males and females was statistically equal. CHARGE syndrome was the most common associated condition found.
Three standard approaches were used for management of CA in these 73 cases: transpalatal, transnasal, and endoscopic; however, the trend for the majority of more recent cases was toward endoscopic treatment. Most cases (91.8%) had a partial or complete bony atresia plate; all these patients required significant resection to obtain an adequate or permanent opening. If the initial surgery failed, the number of follow-up procedures could be extensive and prolonged. However, once the surgical opening of the choana was achieved, it was unusual for it to stenose down in the long term.
The authors state that in the long term, a high arched palate and cross-bite deformity are more likely to be present if the patients undergo the transpalatal approach in the first year of life, especially if CHARGE syndrome is also present, but this trend was not seen with the transnasal or endoscopic techniques. Dr. Hengerer states that he favors the nasal endoscopic technique because it has a low restenosis rate, does not violate the palate, and does not cause the cross-bite and palate arch deformities seen with the transpalatal technique.
(Laryngoscope 2008;118:862-6)
©2008 The Triological Society

Leave a Reply