Hypertrophy of the inferior turbinates is a frequent cause of chronic nasal obstruction. In the last several years, two new techniques have become available for reducing the tumor volume: radiofrequency volumetric tissue reduction (RFVTR) and coblation. As more data become available, clinical researchers are finding that the techniques work well, are safe, and have fewer short-term side effects than traditional surgical submucosal resection.
Explore This Issue
June 2006The Techniques
With RFVTR, also called Somnoplasty (Gyrus ENT), the physician inserts the probe into the head of the turbinate so that the active tip is completely submucosal. The treatment time and amount of energy delivered can be selected by the physician, with the maximal tissue temperature reaching 60° to 90°C. The energy creates a lesion in the meaty part of the turbinate and causes necrosis or coagulation of the tissue, shrinking it from the inside over the course of the next four to six weeks, said Neil Bhattacharyya, MD, Associate Professor of Otology and Laryngology at Brigham and Women’s Hospital in Boston, Mass.
Coblation (ArthroCare Corporation) is similar but the probe is slightly larger and the way the energy is delivered is somewhat different. The probe is inserted and vaporizes tissue within 0.5 mm of the probe surface with radiofrequency current. The energy from the probe also heats immediately adjacent tissue to 40° to 70°C, but the thermal lesion is smaller than in RFVTR.
As more data become available, clinical researchers are finding that the techniques work well, are safe, and have fewer short-term side effects than traditional surgical submucosal resection.
Both procedures can be performed in the office with local anesthesia. Dr. Bhattacharyya estimated that it takes him about 45 seconds with RFVTR and 10 seconds per pass with coblation. He often does several passes with the coblation probe, however.
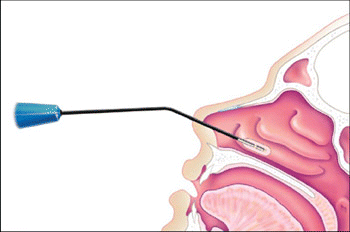
In his experience, coblation results in somewhat faster symptomatic improvement for patients than occurs with RFVTR. On the other hand, he finds that patients feel the coblation more, so if he has a nervous patient, he’ll opt for RFVTR.
Long-Term Outcomes for RFVTR
In the first long-term study on either radiofrequency technique published thus far, Greg A. Krempl, MD, a physician and Clinical Researcher in the Department of Otorhinolaryngology at Oklahoma University Health Sciences Center in Oklahoma City, and colleagues found that the symptomatic benefits from RFVTR were maintained through two years. The authors reported the follow-up data in the April 2006 issue of The Laryngoscope.
The patients evaluated in the current paper were originally treated in a randomized, placebo-controlled trial at the University of Oklahoma. A total of 32 patients were randomized to either active treatment or placebo. To be eligible for the trial, patients had to have prolonged nasal congestion and have been on medical treatment for allergic symptoms for at least six months.
Eight weeks after treatment, patients came into the clinic and, using a visual analog scale (VAS), reported on the degree and frequency of symptom improvement. After filling out the follow-up questionnaire, patients in the placebo arm were told of their sham treatment and allowed to cross over. Twelve elected to do so.
Nineteen of the 28 patients who received treatment were available for a 24-month follow-up. The mean VAS score for the frequency of nasal obstruction was 7.8 at baseline, 4.8 at eight weeks post surgery, 4.6 at six months, and 4.1 at both one and two years. The mean VAS score for the severity of obstruction had a similar drop from 7.7 at baseline to 4.3, 4.9, 4.1, and 4.9 at each time-point, respectively. The mean VAS score for overall ability to breath declined from 7.5 prior to treatment to 4.0, 4.5, 4.0, and 4.2. All changes were statistically significant.
The team did not report any acute or long-term complications with this procedure, though Dr. Krempl noted that most patients have a very runny nose that lasts between two and five days. Furthermore, he did not find any reference to complications such as bleeding or crusting in published studies on RFVTR therapy for turbinate hypertrophy.
The technique, if it is done correctly, just damages undersurface, said Dr. Krempl. If you look at the side effects that occur from working on the turbinates, problems occur either from damaging the surface mucosa, including pain, crusting, and bleeding; from scar tissue on the surface; or from extreme temperature.
Comparing RFVTR to Submucosal Resection of the Turbinates
An Italian group led by Matteo Cavalier, MD, at the Moscati Hospital in Avellino, recently reported the results of a head-to-head comparison of RFVTR and traditional turbinoplasty using submucosal resection. Between January 2003 and December 2003, 75 patients were randomly assigned to one of three treatment arms, surgical resection, RFVTR, or no therapy. To be eligible all patients had to have nasal obstruction that was refractory to medical therapy for at least three months and signs of turbinate hypertrophy.
Patients were evaluated at one week post surgery and after one and three months. Symptoms, including nasal obstruction, sneezing, itchy nose, hyposmia, headache, and snoring, improved in both treatment groups, based on patient-reported VAS scores. The improvements were all statistically significant at three months.
Postoperative pain was higher in the surgery-treated group than in the RFVTR-treated patients, but the difference was not statistically significant.
Crusting was common one week after treatment in the surgery group, with six patients having moderate crusting. The problem had resolved itself by one month after surgery. The side effect was not reported by patients or examining physicians for patients treated with RFVTR.
Finally, the team reported that the nasal mucociliary transport time increased at one week after surgery for the resected patients, while there was no change in those treated with RFVTR. There was no difference in this measure after one month.
Coblation
Fewer studies have been done to look at the effectiveness of coblation in reduction of turbinate hypertrophy. In one study, Dr. Bhattacharyya looked at a consecutive series of 26 patients with medically refractory nasal obstruction due to turbinate hypertrophy. Of the 24 patients who completed the protocol, statistically significant improvements in rhinosinusitis symptoms remained at six months.
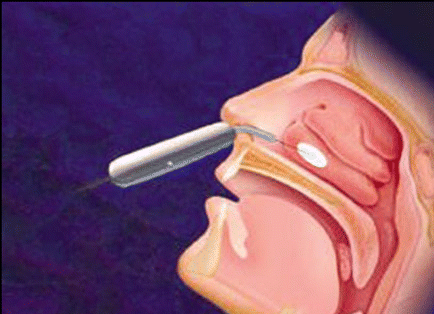
Specifically, the team reported that nasal obstruction, the amount of time obstructed, and nasal stuffiness were improved at six months relative to baseline. However, the team did not see significant improvements in mucus production, postnasal discharge, or snoring at six months.
Two patients had significant bleeding, and crusting occurred in four patients. The crusting was resolved by the three month follow-up exam.
Choosing the Right Patients
So if both techniques work well, how does one choose which to use on a specific patient? Not all turbinates are created equal, said Dr. Bhattacharyya. If the anterior is enlarged he uses coblation, so that he can do the whole procedure in one sitting, using two or three passes. By contrast, if the whole turbinate is enlarged, he opts for RFVTR. He treats the anterior portion in the first appointment and the posterior region six weeks later. Some patients have bony large turbinates in which case neither technique will help. And if either procedure is used in such a case, it can damage the mucosa or expose the bone.
I use radiofrequency for all of my patients who need to be treated for hypertrophy of the turbinates, said Dr. Krempl.
The question is then, do they need to be done in the operating room or not? If all they need is their turbinates addressed, then it can be done as an office procedure. If their airway problems include a deviation in the septum or something else, that would require a trip to the operating room. Most patients have something else wrong, so it is a smaller subset that can be done in the office.
The advantage of the technique, though, is that it can keep patients who only need to be treated for hypertrophy of the turbinates out of the operating room.
©2006 The Triological Society
Leave a Reply