Because of the close relationship her team has developed with the otolaryngologists at Moi Hospital, they elected to do the surgery two days before leaving. “It was not ideal,” Dr. Cordes said, “but we communicated by phone every day while still in the country, and then by e-mail afterward. We went through the entire post-operative plan and reconfirmed each step: ‘This day the drains come out; this day he can start eating,’ etc. And actually, the patient has done well.”
The Rewards and Dilemmas of Surgical Missions
by Gretchen Henkel •
A Surgical Quandary

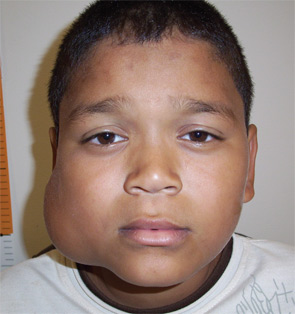
Dr. Boston has participated in eight missions, primarily to Central and South America, and was a coauthor on Drew Horlbeck’s paper on outcomes from otologic surgical missions (Otolaryngol Head Neck Surg. 2009;140(4):559-565). He recalls one difficult case in Panama, a boy with a large facial and neck cystic mass. Dr. Boston had “a pretty good feeling” that the mass was benign, but the only imaging was a basic CAT scan, and a pathology was not available. The boy’s parents wanted something done, since he had endured teasing at school because of his disfigurement.
“We opted to proceed with the surgery,” said Dr. Boston, with the boy’s and the parents’ consent. Intraoperatively, the surgeons found a large cystic mass of the parotid gland, which necessitated performing a total parotidectomy and a very difficult facial nerve dissection. Despite the difficulties, the surgery went well. Dr. Boston counseled the parents about the possibility that the cyst might return, and there was good follow-up care with the Panamanian physicians. A year later, Dr. Boston had the chance to see the boy again. “He was doing well and was extremely happy, with a big smile on his face,” he said.
Route NOT taken
While in Iraq on a mission, Dr. McMains and his team examined a woman with very bad fungal disease, which was pushing in on and eroding a portion of her skull base. She was the person in the most acute need of treatment, so they elected to attempt surgery, even though they would be without image guidance during the procedure. However, on the day of surgery, she presented with uncontrolled hypertension (230/100), and the team had to choose the responsible route: not to attempt what would be a long case under anesthesia. “We had to resist the temptation to view ourselves as the outside experts riding in on the white charger who are going to help this person,” he said of their decision. “Later on, it was going to be safer for her when her other medical conditions were under better control.” According to Dr. McMains, the case illustrates the fact that sometimes, in the words of a character in Abraham Verghese’s novel, Cutting for Stone, “The operation with the best outcome is the one you decide not to do.”
A transformative repair



One patient was 23 years old when Dr. Senders and his team with Operation Restore Hope [headquartered in Australia] saw her in February 2011 in the Philippines. An initial repair for a bilateral cleft lip and palate had left her with a disturbing deformity. At first, the team wondered whether they could help their patient and hesitated to pull her front teeth. After a lot of thought and consultation, Dr. Senders recalled, the team devised a two-step procedure, first repairing her unrepaired palate and removing her nonfunctional front teeth. Three days later, they repaired her lip under local anesthesia. “One surgery would have been too long to be safe,” said Dr. Senders.
Leave a Reply