Have you ever wondered about the reasoning behind hospital discharge paperwork or the requirement that every patient sign a HIPAA form?Here are explanations for some of the health care policies you come across on a daily basis.


Have you ever wondered about the reasoning behind hospital discharge paperwork or the requirement that every patient sign a HIPAA form?Here are explanations for some of the health care policies you come across on a daily basis.
Otolaryngologists with a desire to broaden their careers beyond traditional medical practice have several options. Programs exist that can open doors into medical leadership, health policy work, clinical and outcomes research and public office. Opportunities are available at all stages of a physician’s career. Here’s a look at a handful of programs that aim to provide physicians with the tools they need to take their careers in a new direction.

Close on the heels of the evidence-based medicine movement comes increasing pressure for physicians and health care institutions to develop and implement quality improvement measures that will not only improve quality of care, but also reduce medical costs and provide a way to measure performance by physicians and institutions. Integral to this process is the development of appropriate metrics by which to measure outcomes and physician performance that accurately reflect otolaryngology and its subspecialties. Two sessions at the recent 2011 American Academy of Otolaryngology–Head and Neck Surgery Annual Meeting held here Sept. 13 highlighted issues that are important for otolaryngologists striving to meet the growing demand for quality improvement.
Although the new U.S. health care law does not specifically alter the current fee-for-service payment structure, changes to how physicians and hospitals will be reimbursed for services are under construction. These changes are reflected by the growing focus on the development and implementation of quality improvement and physician and institutional performance measures on which reimbursement will increasingly be made, panelists said here on Sept. 11 at the 2011 American Academy of Otolaryngology-Head and Neck Surgery (AAO-HNS) Annual Meeting.
There is a Chinese proverb that is both a blessing and a curse. The blessing is, “May you live in interesting times,” and the curse is, “May you live in interesting times.” All of us would like things to stabilize into a constant, comfortable and predictable environment for us to live our lives, raise our families and care for our patients. We are entering the most complex and challenging period that medicine has experienced since the 1960s when Medicare was introduced. From now on, everything we have come to know and are comfortable with in our professional lives will change.
Medicare requirements for physician supervision of speech-language pathologists conducting videostroboscopy (CPT 31579) and nasopharyngoscopy (CPT 92511) will move from the strictest level of oversight back to no national supervision level starting in October.
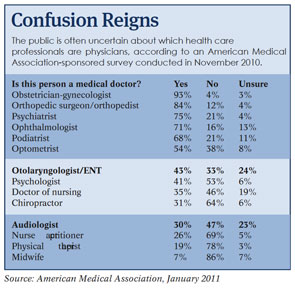
More often than not, members of the public are confused about which health care providers are physicians and which are not. That uncertainty is expected to increase as the trend toward non-physician providers earning doctorate degrees continues and as demand for services grows with the millions of people gaining insurance under the 2010 health reform law.
As in all of medicine, the future of sleep medicine will be defined in part by changes evolving under the health care reform law and by the need to slow the unsustainable cost of medical care, experts said here last month at a session at SLEEP 2011, the 25th Annual Meeting of the Associated Professional Sleep Societies,