For many years, all vascular anomalies were called hemangiomas. New insights over the past decade into the biology of infantile hemangiomas have led to a revised system of classification for these entities. The majority of hemangiomas appear on the head and neck, and otolaryngologists-head and neck surgeons are often the treating or consulting physicians. It is important for them and other specialists who see these lesions to be aware that there are important distinctions between garden variety hemangiomas (which account for the vast majority) and hemangiomas that can be more serious, even life-threatening.
Explore This Issue
May 2006Embryogenesis and Classification
The field is evolving and hemangiomas are a fertile area of research. Hemangiomas have a fascinating life cycle. They do not grow in utero, but blossom during the first few weeks of life. Most of them grow and resolve on their own. Hemangiomas hold a secret, and if we could understand why they grow and why they resolve, we might find a key for curing cancers, stated Francine Blei, MD, a pediatric hematologist/oncologist and Director of the Vascular Anomalies Program at New York University in New York City.
At present, there is no cohesive theory of the etiology of infantile hemangiomas, and the clinical heterogeneity suggests that there are multifactorial origins, Dr. Blei said. Some evidence suggests that the embryogenesis of hemangiomas involves cells of origin derived from the placenta that migrate into the fetal circulation during the first few weeks of life, when the fetus is mostly head and neck, explained Milton Waner, MD, Director of the Vascular and Birthmark Institute in New York City. Dr. Waner is an otolaryngologist-head and neck surgeon.
All vascular lesions are not hemangiomas. In the old days, hemangioma was a ‘waste basket’ term for any type of vascular malformation. Unfortunately, some physicians still apply that definition, Dr. Waner commented.
Dr. Waner described a new classification system for vascular anomalies that includes three major categories: 1) hemangiomas; 2) vascular malformations; 3) vascular tumors, including RICH (rapidly involuting tumors), NICH (non-involuting tumors), and Kaposiform hemangioendothelioma. GLUT-1 (glucose transporter isoform-1) staining, a recent advance, is used to differentiate between vascular anomalies based on histopathology.
Hemangiomas hold a secret, and if we could understand why they grow and why they resolve, we might find a key for curing cancers. – -Francine Blei, MD
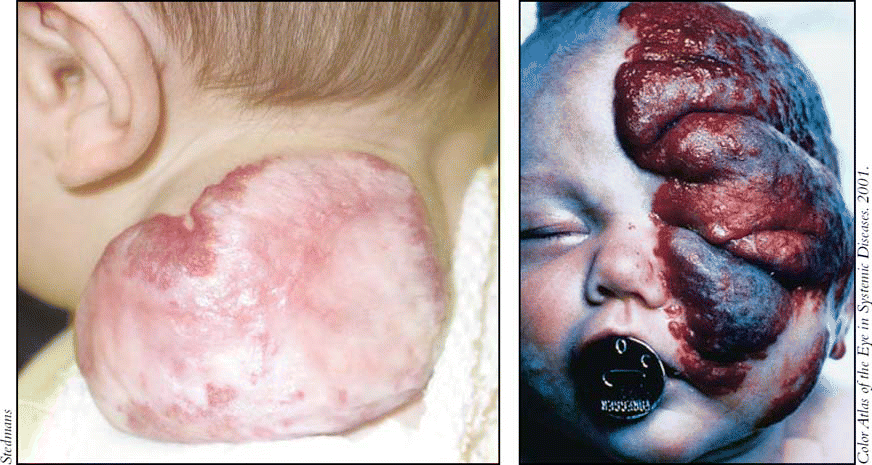
Kaposiform hemangioendotheliomas have a distinct appearance and are radiologically and histologically distinct from hemangiomas. They look like bruises and are boggy, Dr. Blei noted.
Management of Hemangiomas
Management of hemangiomas is cross-disciplinary. Patients with infantile hemangiomas can be seen by otolaryngologists, head and neck surgeons, pediatric dermatologists, pediatric oncologists, hematologists, and general and plastic surgeons. Interviews with experts suggest that the various specialties have different perspectives on the timing and types of treatments that they consider appropriate.
Although the vast majority of infantile hemangiomas require no treatment except observation, some important exceptions require special consideration. These include large, disfiguring hemangiomas on the face or neck; periocular or periorbital hemangiomas that can affect vision; hemangiomas on the nose that can interfere with breathing; and hemangiomas in the beard distribution-that is, in front of the ears, on the chin and the upper lip, and the anterior neck. Those in the beard distribution carry a high risk of an accompanying symptomatic airway hemangioma, which can cause death due to asphyxiation if large and circumferential, Dr. Blei explained.
If a child presents with recurrent stridor, or stridor when it is not croup season, a subglottic hemangioma should be suspected, Dr. Blei stated. Croup can be treated with a short course oral of steroids and the stridor may resolve for a short period of time, but a recurrence suggests that an airway hemangioma is present. Subglottic hemangiomas are treated with oral steroids and laser surgery; in some cases, laser can avoid the need for steroids. Tracheotomy may be required if steroids are ineffective and the child is in extremis, Dr. Blei said.
Not all large facial hemangiomas will have accompanying anomalies; in fact, large facial hemangiomas without anomalies are probably more common that those associated with PHACES. – -Denise Metry, MD
Unusual or large hemangiomas on the face may be associated with failure to thrive syndrome. Dr. Blei said that children with very large hemangiomas having increased blood flow can have cardiac problems and should be referred to a cardiologist for evaluation. In general, any patient with a complicated hemangioma should be referred to a vascular anomalies center for a treatment plan, which can then be carried out in conjunction with the child’s local doctor.
Typically, surgery should be used to treat any disfiguring hemangioma or one that distorts or destroys a function, where no other modality can correct this. – -Milton Waner, MD
Prompt recognition and referral of large or otherwise problematic hemangiomas to experienced centers is indicated [for unusual or complicated hemangiomas]. Disasters can occur if these are not appropriately managed, Dr. Blei said.
PHACES
All doctors who treat infants should be aware of the PHACES syndrome. PHACES is an acronym used to describe a group of anomalies that was coined by Ilona Frieden, MD, in 1996. More than 90% of those with PHACES are female. The hallmark of PHACES is a large, segmental hemangioma, usually located on the face, plus one or more of the listed congenital abnormalities (see box, bottom left). Thus far, more than 200 cases have been reported in the literature.
PHACES is thought to be due to an error in development that probably occurs some time during the first three to 12 weeks of gestation, explained Denise Metry, MD, Associate Professor of Dermatology and Pediatrics at Texas Children’s Hospital and Baylor College of Medicine in Houston, Tex. Dr. Metry, together with her mentor Dr. Frieden, is considered an expert in PHACES.
Not all large facial hemangiomas will have accompanying anomalies; in fact, large facial hemangiomas without anomalies are probably more common that those associated with PHACES, she said.
Treatment of PHACES is cross disciplinary. Otolaryngologists should know how to diagnose PHACES, Dr. Metry said. The currently recommended work-up is as follows:
- MRI (magnetic resonance imaging) and MRA (magnetic resonance angiography) of the head;
- Formal ophthalmologic exam;
- Cardiac MRA or echocardiography; and
- Skin exam for sternal defects and supraumbilical raphé (linear, scar-like lesion above the umbilicus).
Referral to another specialist depends on the type of accompanying anomalies that are identified during the work-up. At this time, there is no means of prevention. Any potential treatment depends on the specific defects identified, Dr. Metry noted. Hundreds of anomalies are associated with PHACES, she added. Some of these are quite rare and unique.
Dr. Metry and colleagues are in the process of setting up a Web-based patient registry that will help aid collaborative research and serve as an educational resource for families with PHACES children.
The majority of hemangiomas appear on the head and neck, and otolaryngologists are often the treating or consulting physicians.
Treatment
Many vascular lesions may resemble hemangiomas, but a basket of vascular malformations, lymphatic malformations, and venous malformation that resemble hemangiomas require different treatment and have different life cycles, Dr. Blei explained. GLUT-1 staining should be done on surgical specimens when the diagnosis is questionable, she added.
In general, treatment of facial hemangiomas that are disfiguring and affect function relies on oral corticosteroids, strong topical steroids, or intralesional steroid injections; surgery or laser surgery may be needed to prevent morbidity. Complicated hemangiomas that continue to grow aggressively, either internally or externally, are first treated with oral steroids. If there is no response, vincristine has been used. Ulcerated hemangiomas often respond well to topical recombinant platelet-derived growth factor (Regranex), and those associated with bleeding respond to a hemostatic gelatin sponge (Surgifoam), Dr. Blei explained.
Surgery
The need for surgery depends on your endpoint, said Dr. Waner, who considers the appropriate endpoint to be restoration of a completely normal appearance.
Typically, surgery should be used to treat any disfiguring hemangioma or one that distorts or destroys a function, where no other modality can correct this, he stated.
In his experience, fewer than 50% of hemangiomas will involute (i.e., stop proliferating and shrink) to the point where laser plus or minus surgery will not be necessary. The vast majority of hemangiomas that do involute leave a residual fibrofatty area with loss of pigmentation and atrophic scarring, he noted. Further, it can take five, seven, or even 12 years for a hemangioma to involute completely.
Nowadays children attend preschool and are subjected to peer pressure very early in their lives. A disfiguring lesion that can be embarrassing and distressing for the child should be removed as early as possible, said Dr. Waner. The younger the patient, the less scarring and the easier it is for primary closure, he noted. However, if complete excision is not feasible, then surgery should be postponed at least nine months until the lesion has stopped growing.
Surgery should be considered as early in life as possible for lesions that cause functional problems, agreed Jonathan Perkins, DO, an otolaryngologist-head and neck surgeon at the University of Washington and Children’s Hospital in Seattle. In general, he said that in infants under the age of six months, hemangiomas of the eye and airway are the most common ones that require surgery.
When asked about success rates for surgery, Dr. Perkins said that there are no reports on large series of patients who have undergone surgery for hemangiomas. It depends on how you define success and the goals of surgery. For an airway hemangioma, success equals preventing tracheotomy, and surgery can accomplish this 90% of the time. For periocular hemangioma, success equals preventing amblyopia. We are able to do that with surgery or steroid injections up to 70% of the time.
For disfiguring hemangiomas of the face, the timing of surgery is controversial, according to Dr. Perkins. Dr. Waner is a proponent of very early surgery, while other experts believe that surgery should be delayed until after 10 months of age, or lower when the hemangioma has stopped proliferating.
We don’t know what the optimal timing is, Dr. Perkins stated.
He said that facial hemangiomas can be superficial (formerly called strawberry, red in color), deep (formerly called cavernous, often blue in color), or mixed. Superficial lesions can be treated with pulsed dye laser to reduce redness. Deeper lesions may require lifting the skin, excising the lesion, and replacing the skin over the area. Mixed lesions can be treated with laser to remove the redness and scarify the skin so that the superficial and deep portions of the lesions can be safely removed and the incision securely closed.
Other Vascular Lesions
It is important to recognize which vascular lesions are RICH (rapidly involuting tumors), because these do not require any treatment, Dr. Waner said. RICH tumors will involute completely by age two. By contrast, NICH (non-involuting tumors) may be persistent and continue to proliferate. The best treatment for these is not clear, Dr. Waner said, but systemic vincristine or interferon or embolization may be used. Kaposiform hemangioepithelioma are managed medically, usually with vincristine. Dr. Waner said that a high proportion of Kaposiform patients who are treated with interferon will develop spastic diplegia.
Even though much has been learned about hemangiomas over the past decade, it can take as long as a decade for medical practice to keep pace with new knowledge. According to Dr. Blei, otolaryngologists need to know that not every vascular lesion is a hemangioma, and that it is important to recognize which hemangiomas are problematic and refer them to the appropriate specialists.
PHACES: An Association of Varied Symptoms
- Posterior fossa and other structural brain abnormalities
- Hemangioma of the cervicofacial region
- Arterial cerebrovascular anomalies
- Cardiac defects and Co-arctation/other aortic abnormalities
- Eye abnormalities
- Sternal defects and/or Supraumbilical raphe
©2006 The Triological Society



Leave a Reply