PHILADELPHIA-It is generally accepted that foreign microbial antigens drive the inflammation in chronic rhinosinusitis. Which antigens are responsible, though, is not certain. But researchers are trying to find out.
Explore This Issue
June 2009At Rhinology World 2009, two experts in the field debated the causes of the disease and discussed the prospect of homing on better treatments. But even as they did so, they acknowledged that the way the patient reacts to the antigens ultimately causes the problem.
Jens Ponikau, MD, Assistant Professor of Clinical Otolaryngology at the State University of New York-Buffalo, pointed to eosinophils in making his case that fungi are at the heart of chronic rhinosinusitis, a group of disorders involving inflammation of the mucus of the nose and paranasal sinuses, lasting at least 12 weeks.
Robert Kern, MD, Professor and Chairman of the Department of Otolaryngology-Head and Neck Surgery at the Northwestern University Feinberg School of Medicine in Chicago, argued that the evidence pointing to fungi as the main instigators is thin.
Eosinophils Provide Evidence for Fungi
Dr. Ponikau’s research has shown how eosinophils, which are the main inflammatory agent, attack fungi in patients with CRS. He also pointed out studies showing positive results from antifungal medications in combating the disease.
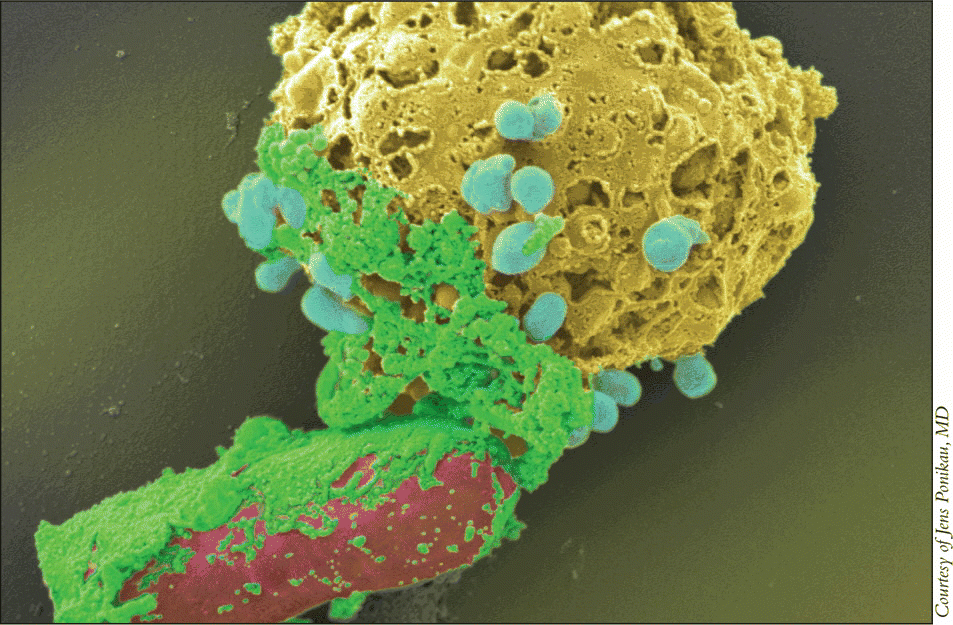
In a video, he showed eosinosphils tearing apart fungal germinating spores when they were stimulated with a signal coming from the lymphocytes of CRS patients. You can nicely see how the eosinophils start to target the fungi, he said. You can see they don’t bother about the hyphae [the mature segment]. They’re going after the germinating spores [which secrete the antigen].
When lymphocytes from healthy controls were used, the eosinophils didn’t get the attack signal and did not react the same way. The eosinophils kind of sniff on there a little bit…and walk away again, Dr. Ponikau said. No attack.
He added, Believe it or not, this became the difference between a patient who had CRS and a healthy person.
Dr. Ponikau’s research has shown that the production by patients’ lymphocytes of interleukin (IL)-5, a key cytokine that activates and prolongs the life of eosinophils, is instigated by the presence of the fungus Alternaria. The same is true with the cytokine IL-13, which is key to recruiting the eosinophils to the sinus tissue. The key was that only patients with CRS were reacting, but healthy controls did not react to the fungi by producing these, he said.
Dr. Ponikau examined several types of fungi, but Alternaria produced the most significant effects. All the other fungi didn’t really matter, he said. It was really a signal that was coming out of Alternaria which was doing that.
Antifungal medications have shown promise in treating chronic rhinosinusitis patients. In a small study including 10 patients taking amphotericin B, an antifungal, and 14 control subjects, those with the disease showed a 10% reduction in nasal blockage, according to CT scans. The control group showed hardly any change. When the same groups were examined using an endoscope, the amphotericin B group showed much better results than a placebo group, after both three months and six months.
Further studies have shown that IL-5 levels were reduced in patients taking amphotericin B.
In a larger study of amphotericin B’s effects, on 299 chronic rhinosinusitis patients, the primary endpoint-complete clearance of congestion and the total loss of headache-was not met. But Dr. Ponikau said that the study still showed promise because of the effects that could be seen in those patients with more severe symptoms.
When you slice this trial apart, it was interesting that, if you look at the patients who had more severe intense inflammation, the trial becomes significant in improving the patients’ symptoms, he said. The more inflammation that they had, the better the antifungals would work.
The reason for the discrepancy was that in the patients with less severe symptoms, the effects of the lavage could not be distinguished from the effects of the drug. The problem, he said, was that there was actually a therapeutic effect of the lavage itself. And the antifungals were working better, but it was very difficult to overcome that therapeutic effect.
Evidence for Bacterial Causes
Dr. Kern expressed doubts that fungi play as critical a role in chronic rhinosinusitis as Dr. Ponikau suggested, pointing instead to studies highlighting the role of bacteria.If you look at the microbiology of CRS, you can look at a number of studies that suggest that staph are disproportionately present in CRS patients with nasal polyps, as opposed to controls, he said, although he acknowledged that fungi are present as well.
The research group at Northwestern isolated staphylococcal toxins in polypoid sinusitis and found evidence of a characteristic T-cell response to those toxins in polyp tissues. There is a fingerprint of the staph effect, Dr. Kern said. The fingerprint is seen in about half of the cases. Nevertheless, this fingerprint is definitely there. The staph effect can be seen.
Despite that finding, Dr. Kern said that the major question should not be whether fungi or bacteria are the central players. Rather, attention should be turned to problems with the nasal mucosal immune barrier of CRS patients.
Remember that staph and fungi are very common, he said. They’re frequently recovered from both normal and CRS patients. It’s inflammation as well, not tissue invasion. So the assumption that we’re making is that microbial pathogens are key to the whole process. I have some problems with that. Rather than debate what the organism is, we should be looking at the host, because it’s really a dysfunctional host- environment interaction. And the key problem is the host, not the bacteria.
The research team at Northwestern, focusing on chronic rhinosinusitis with polyps, examined defects in epithelial integrity and repair, defects in toll receptor signaling, and defects in the transition from an innate response to an acquired response.
When looking at the integrity of the epithelium, they screened a great number of genes. Thus far, we have identified four that seem to be part of the problem: three genes in the S100 group, which are important in repair and also have antimicrobial effects; and Spink 5, a protease inhibitor.
The epithelial cells in sinusitis with polyps are deficient in Spink 5, so they would have a decreased ability to limit or mute the protease effects of fungi or bacteria, which mediates their ability to dissolve the epithelial barrier, Dr. Kern said.
As for S100’s role, he said, If they’re diminished, that would certainly foster colonization of bacteria. So if patients with polypoid sinusitis have this defect, this would lead to slower healing following injury as well as increased microbial colonization. These effects are superimposed on the fragile mechanical barrier mediated by diminished Spink 5, he said.
In looking at pattern-recognition receptor signaling, researchers focused on the TLR-2 because it has been associated with staph and fungi. Northwestern researchers exposed epithelial cells to TLR-2 ligands and assayed for cytokines responses. They saw that the IL-8 response was diminished, causing a muted ability to recruit neutrophils as well an enhanced tendency to generate IL-6.
What does this mean? We’re not certain. But if you think about this CRS-with-polyps phenotype, there’s a diminished innate immune response, so this IL-8 would follow into that, Dr. Kern said. On the other hand, one of things that IL-6 does is just that: It shuts off the innate immune response and fosters the acquired immune response. So the combined effect of defects in this pathway could theoretically foster the picture of diminished innate immunity coupled with an enhanced acquired immune response-the picture we see in nasal polyposis.
Dr. Kern also pointed out that, in ongoing research, mRNA for the cytokine TSLP is upregulated in nasal polyps. That would certainly suggest the hypothesis that stimuli-whether it be bacteria, fungi, or whatever-are stimulating toll receptors with an augmented TSLP response, Dr. Kern said. TSLP may secondarily lead to an accentuated TH2 immune response with eosinophil recruitment, additional characteristics of CRS with nasal polyps, he said.
The ligand BAFF, which activates B-cells, also appears to be present in greater amounts in polyp patients, Dr. Kern said. BAFF recruits B-cells and triggers them to secrete IgA. Probably the most potent stimulant for eosinophilic degranulation is IgA, Dr. Kern said.
Taken together, this evidence suggests the hypothesis that nasal polyposis is mediated by a defective innate immune barrier and an excessive compensatory acquired immune response, Dr. Kern said. The latter is characterized by a skewed TH2 and IgA response directed against a variety of microbial antigens, probably both bacterial and fungal. The excessive IgA may be one mechanism for excessive eosinophil degranulation that has been proposed as a final common pathway for polyp formation.
Future treatments are likely going to be targeted to these and other specific defects in the patient, rather than [using] broad-spectrum antibiotics, antifungals, or corticosteroids, he said.
The Debate Continues
Dr. Ponikau defended his hypothesis that fungi are the crucial trigger of chronic rhinosinusitis. I’m able usually to induce an eosinophilic inflammation [with fungi], he said. I have not seen any data that show that actual bacterial antigens are capable to produce eosinophils. I’ve never seen a single study that has demonstrated that. And at the end of the day these are the granulocytes that release the proteins that do the damage to our patients.
But Dr. Kern found that unpersuasive. Showing that activated eosinophils from the bloodstream attack fungi is not particularly surprising. They probably attack everything-they’re activated eosinophils. But the question is: Did the fungi elicit a T-cell mediated response? And we have no evidence of that.
Dr. Ponikau said his data on production of IL-5 and IL-13, which are the cytokines crucial for the eosinophilic inflammation in CRS and are the ones produced by the T-cells, indicates that the fungi are causing that kind of response. These were actually lymphocytes, including the T-cells, which were stimulated by the fungal antigens and they showed those responses, he said. They responded with a production of IL-5 and IL-13. These are exactly the cytokines we see in our patient populations being elevated.
Dr. Kern said that because 78% of the patients in that study also had asthma, there are questions about fungi’s precise role. At heart, that is the single most important piece of evidence in support of the fungal hypothesis, he said. But if you remember, the vast majority of those patients also had asthma. So you’re taking blood from a patient with asthma-how do you know which is causing the response, asthma or polypoid sinusitis?
Dr. Kern also said that Dr. Ponikau’s studies involved massive amounts of antigens, far more than would ever be experienced at the epithelial surface.
So it’s difficult to say that they are specific responses in the sense of relevance to the clinical state, he said.
Dr. Ponikau said later that his lab tested many different concentrations of fungal antigens before carrying out the study; they found that 50 mcg/mL was optimal, and that using a lesser or greater concentration didn’t work as well. He added that nobody knows the actual concentration of the antigen on the T-cells in vivo in CRS patients.
The debate is likely to continue.
In the end, Dr. Kern said, It comes down, I guess, to being a believer or not.
©2009 The Triological Society
Leave a Reply